Understand how vets diagnose and treat canine Lyme disease, including doxycycline dosing tips, safe pain relief, kidney monitoring, and smart tick prevention...
Article
•
Designer Mixes
Treating Dogs for Lyme Disease

Shari Shidate
Designer Mixes contributor

Lyme disease in dogs: what’s true, what’s hype
As a veterinary assistant here in North Texas, I’ve seen how confusing Lyme disease can feel for dog parents. The internet is full of “miracle cures,” but Lyme disease is one of those conditions where the safest path is also the most effective: early veterinary care, evidence-based medication when needed, and thoughtful at-home support.
The most overlooked part is that treating Lyme is not just about “killing bacteria.” It is also about recognizing symptoms early, watching the kidneys, and preventing reinfection with excellent tick control.
Quick refresher: what Lyme is
Lyme disease is caused by the bacterium Borrelia burgdorferi, spread through bites from infected ticks. In the U.S., the main vectors are black-legged ticks (also called deer ticks, Ixodes species). This detail matters because many owners find American dog ticks, and those are not the typical Lyme carriers.
Geography matters, too. Lyme is most common in the Northeast, Upper Midwest, and parts of the Mid-Atlantic. Here in Texas, we still see tick-borne disease concerns, but Lyme risk can vary a lot by county, travel history, and lifestyle.
Not every tick carries Lyme, and not every exposed dog becomes sick. Some dogs test positive but never show symptoms, while others develop painful, sudden signs.
Common symptoms can include:
- Lameness that shifts legs or comes and goes
- Stiffness, trouble getting up, reluctance to run or jump
- Fever, fatigue, reduced appetite
- Swollen joints
One of the biggest concerns is a less common but serious complication called Lyme nephritis, a kidney-related syndrome that can become life-threatening.
Key steps for treating Lyme
1) Focus on comfort and prevention
Treatment is often recommended when a dog is clinically ill (showing symptoms). In many symptomatic cases, veterinarians prescribe antibiotics, most commonly doxycycline, often for about 28 days (your vet may adjust based on your dog’s situation).
Many dogs improve quickly, sometimes within days, but that improvement mainly means inflammation is settling down and your dog is feeling better. Some dogs can remain seropositive (show antibodies) for months or even longer after exposure or treatment, so follow-up is about the whole dog, not just a single test result.
2) A positive test is not always an emergency
This surprises a lot of people. Some dogs test positive on a screening test and feel completely fine. Depending on the test used, your dog’s risk factors, local prevalence, and your veterinarian’s clinical judgment, your vet may recommend additional testing and monitoring rather than automatic antibiotics. Other veterinarians may treat certain asymptomatic positives, especially if there are other concerns. The point is: it should be a deliberate decision, not a panic decision.
3) Testing is more nuanced than most posts admit
Many clinics start with a screening test (often a SNAP-style test) that detects antibodies. Antibodies can reflect exposure, not necessarily active disease today. Your veterinarian may recommend additional steps based on the full picture, which could include a quantitative Lyme test (such as a C6 test), repeat testing, and checking for other tick-borne diseases.
4) Kidney monitoring is the part many people skip
If your dog is positive for Lyme, ask your veterinarian what kidney monitoring they recommend. This may include a urinalysis (often to check for protein in the urine), a urine protein:creatinine (UPC) ratio, bloodwork to evaluate kidney function, and sometimes blood pressure checks if protein loss is a concern. Catching kidney issues early can significantly improve outcomes.
5) Pain control matters and must be chosen carefully
Some dogs need help getting comfortable while antibiotics do their job. Your veterinarian may recommend an anti-inflammatory medication or other pain support. Never give human pain relievers to dogs unless your veterinarian specifically directs it. Several common over-the-counter options can be dangerous for pets.
6) Reinfection prevention is part of treatment
Even if your dog recovers beautifully, a new infected tick can bite tomorrow. Effective tick prevention is not optional in Lyme country. Your best long-term plan is prevention.

When to call the vet fast
Lyme can look like many other problems. Please call your veterinarian promptly if you notice:
- Sudden limping, especially shifting leg lameness
- High fever, lethargy, or refusing meals
- Swollen joints or obvious pain
- Vomiting, diarrhea, or dehydration
- Increased thirst or urination, accidents in the house
- Swelling in the legs or belly
- Unusual bruising or bleeding (not specific to Lyme, but a red flag for serious illness)
Those last few can be red flags for kidney involvement or other serious illness and should not wait.
Evidence-based home support
Home care does not replace veterinary treatment, but it can support recovery and comfort.
Hydration and simple, nourishing meals
When dogs feel achy, they often drink less. Encourage water intake, offer broth made for pets, and focus on easy-to-digest, high-quality food. If you use broth, avoid ingredients like onion, garlic, or excess salt. Many store-bought broths contain onion and garlic, which are toxic to dogs. If your dog has any kidney concerns, follow your vet’s diet guidance closely.
Rest, then a gradual return to activity
Joint pain can flare if a dog returns to hard play too quickly. Short leash walks, gentle movement, and slow increases are usually the safest approach until your dog is consistently comfortable.
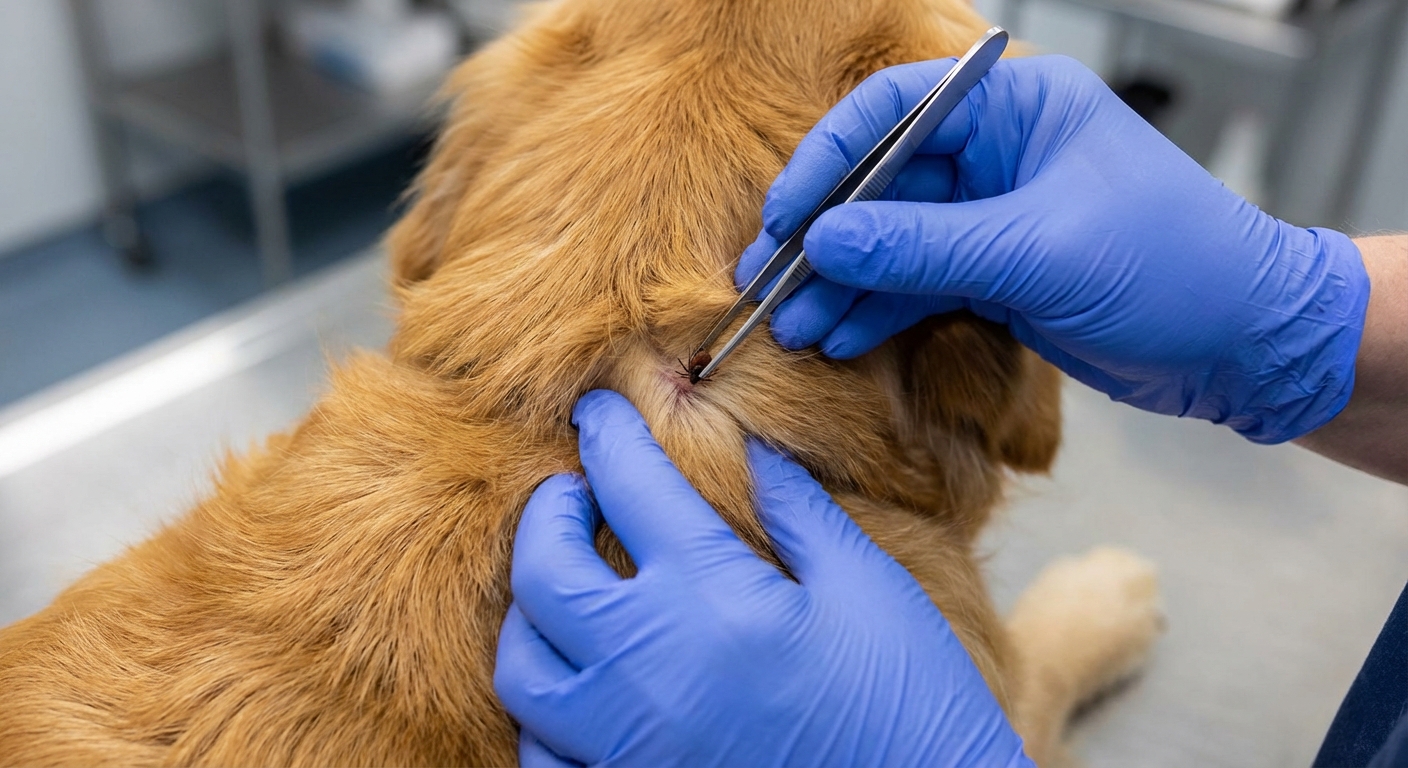
Daily tick checks (timing matters)
Especially after walks in tall grass or wooded areas, run your hands through your dog’s coat and check common hiding spots: ears, under the collar, between toes, armpits, and the groin area. Removing ticks promptly lowers the chance of disease transmission. For Lyme specifically, the tick typically needs to be attached for about 24 to 48 hours before transmission becomes much more likely, which is a big reason daily checks are so powerful.
Helpful mindset: Treat Lyme like you would treat a fire. Put it out (medical care), clean up the smoke damage (monitor joints and kidneys), and then prevent another spark (tick prevention).
What to avoid
- Stopping antibiotics early because the dog looks better. Always finish medication exactly as prescribed unless your veterinarian instructs otherwise.
- Using essential oils on your dog without veterinary guidance. Some are irritating or toxic, and topical use can cause skin issues or even neurologic signs if ingested during grooming.
- Assuming every limp is Lyme. ACL tears, arthritis, spinal pain, and other infections can look similar. Other tick-borne illnesses like Anaplasma and Ehrlichia can also cause overlapping signs.
- Skipping follow-up. Rechecks and kidney monitoring are part of responsible Lyme care.

Prevention
Talk with your veterinarian about the best prevention plan for your dog, which can include:
- Year-round tick preventives (topical or oral options)
- Landscape changes like keeping grass trimmed and reducing brushy areas
- Tick-smart walking routes during peak seasons
- Lyme vaccination for dogs at higher risk, based on your location and lifestyle (this is generally considered non-core and it does not replace tick prevention)
If you live in an area with a heavy tick burden or you travel with your dog, prevention is usually far less stressful and far less expensive than treating illness later.
Common questions for your vet
- Is my dog’s positive test consistent with active Lyme disease or past exposure?
- What test was used, and do you recommend any follow-up or confirmatory testing (such as a quantitative C6)?
- Do you recommend antibiotics in this case, and why?
- How long should treatment last, and what side effects should I watch for?
- What follow-up testing do you recommend, especially for kidney monitoring (urinalysis, UPC, bloodwork, blood pressure)?
- Should we test for other tick-borne diseases like Anaplasma or Ehrlichia?
- What signs at home would mean my dog needs to be seen urgently?
- What tick prevention is best for my dog’s age, size, and medical history?
People in the home: a quick note
Dogs do not directly transmit Lyme disease to people, but ticks can hitch a ride into the house on pets. Tick prevention and tick checks protect the whole household.
The bottom line
Lyme disease can be very treatable, and many dogs go on to live full, active lives. The most powerful approach is not a secret herb or a one-time pill. It is a smart combination of veterinary diagnosis, the right medication when appropriate, follow-up monitoring, and serious tick prevention.
If you’re worried your dog may have Lyme disease, schedule a vet visit and bring notes about symptoms, travel history, and any tick exposure. Your observations truly help your care team.