Periodontal disease is common in cats and often hides in plain sight. Learn the 4 stages, subtle warning signs, and how to prevent pain with brushing, VOHC p...
Article
•
Designer Mixes
Tooth Resorption in Cats

Shari Shidate
Designer Mixes contributor
Tooth resorption in cats is one of those problems that can hide in plain sight. Many cats keep eating, keep grooming, and keep acting “mostly normal” while a tooth is being broken down by the body’s own resorptive cells. As a veterinary assistant, I can tell you this is incredibly common, and it is also very treatable once it is found.
Tooth resorption, sometimes called FORLs (feline odontoclastic resorptive lesions), is one of the most common reasons cats need tooth extractions in practice. Prevalence estimates vary widely by study and the population examined, but many veterinary dentistry studies report that a substantial portion of adult cats are affected at some point, with risk increasing with age. Some lesions are subtle or hidden until dental radiographs reveal what is happening below the gumline.

What it is
Tooth resorption happens when specialized cells (odontoclasts) begin to break down the hard structures of the tooth. In many cats, this starts near the gumline and slowly progresses. Over time, the body treats part of the tooth like it should be removed, and the tooth structure is replaced by inflammatory tissue or bone.
Veterinarians commonly describe two main patterns, and you may also hear about mixed lesions that show features of both:
- Type 1 (inflammatory): The tooth root is being destroyed and there is often inflammation and periodontal disease present. These teeth typically require full extraction of the root.
- Type 2 (replacement): The tooth root is being resorbed and replaced by bone. Some of these cases may be treated with crown amputation in specific situations, but the decision depends on dental radiographs.
- Mixed (Type 1 and Type 2): Parts of the root may look inflammatory while other areas show replacement changes. Treatment is individualized based on radiographs and what the roots are doing.
The exact cause is not fully understood. What we do know is that it is not just “tartar”, and it is not something you can brush away once it starts. Home care is still valuable for overall oral health, but resorptive lesions themselves need veterinary treatment.
Why it hurts
Resorptive lesions often expose sensitive dentin and can eventually involve the pulp, which contains nerves and blood supply. That is why these teeth can be extremely painful.
Cats are masters at hiding discomfort. In the clinic, a cat may purr, sit quietly, or even head-butt you, and still have significant oral pain. Many families only notice subtle changes, or they assume their cat is “just getting picky.”
Pain from tooth resorption is real and intense. If you suspect it, do not wait for obvious crying or refusal to eat.
Signs to watch for
Some cats show obvious mouth discomfort, but many do not. Here are the signs I encourage cat parents to take seriously, even if they come and go:
- Drooling, especially new or increased drool
- Head tilting while eating or eating on one side
- Jaw chattering (sometimes right after chewing)
- “Chew and drop” behavior, picking up kibble then dropping it
- Slower eating or walking away from the bowl more often
- Pawing at the mouth or face rubbing
- Bleeding from the mouth or blood on toys
- Bad breath that is persistent
- Behavior changes: hiding more, grumpiness, less play, not wanting to be touched around the face
- Decreased grooming or a messier coat (pain can make grooming feel like too much work)
- Weight loss in chronic cases
Important note: many cats with tooth resorption still eat. They may simply swallow food more quickly, chew less, or prefer softer options.
Also, please do not force your cat’s mouth open at home if you suspect dental pain. A quick peek is fine if your cat allows it, but pushing the issue can get you bitten and can worsen your cat’s stress.

What it looks like
Sometimes you can see a small pink or red spot at the gumline, often on the cheek side of the tooth. Other times the gum grows up and over the lesion, which can hide what is going on underneath.
But here is the tricky part: the worst damage is often below the gumline, where you cannot see it at home. This is also why cats can look “fine” until the lesion is advanced.
When I see these in the clinic, the teeth that are commonly involved are the premolars and molars, although any tooth can be affected.
Diagnosis and radiographs
A thorough diagnosis usually involves:
- Oral exam: often under anesthesia because cats will not tolerate a full, pain-free inspection while awake
- Dental probing: to check the gumline and identify defects
- Full-mouth dental radiographs: the gold standard for confirming tooth resorption and determining the type and severity
Dental radiographs are not an “extra” in these cases. They guide the treatment plan and help your veterinarian decide whether a tooth needs complete extraction or whether a crown amputation could be appropriate for a specific Type 2 lesion. They also help detect lesions that are hidden under the gums.
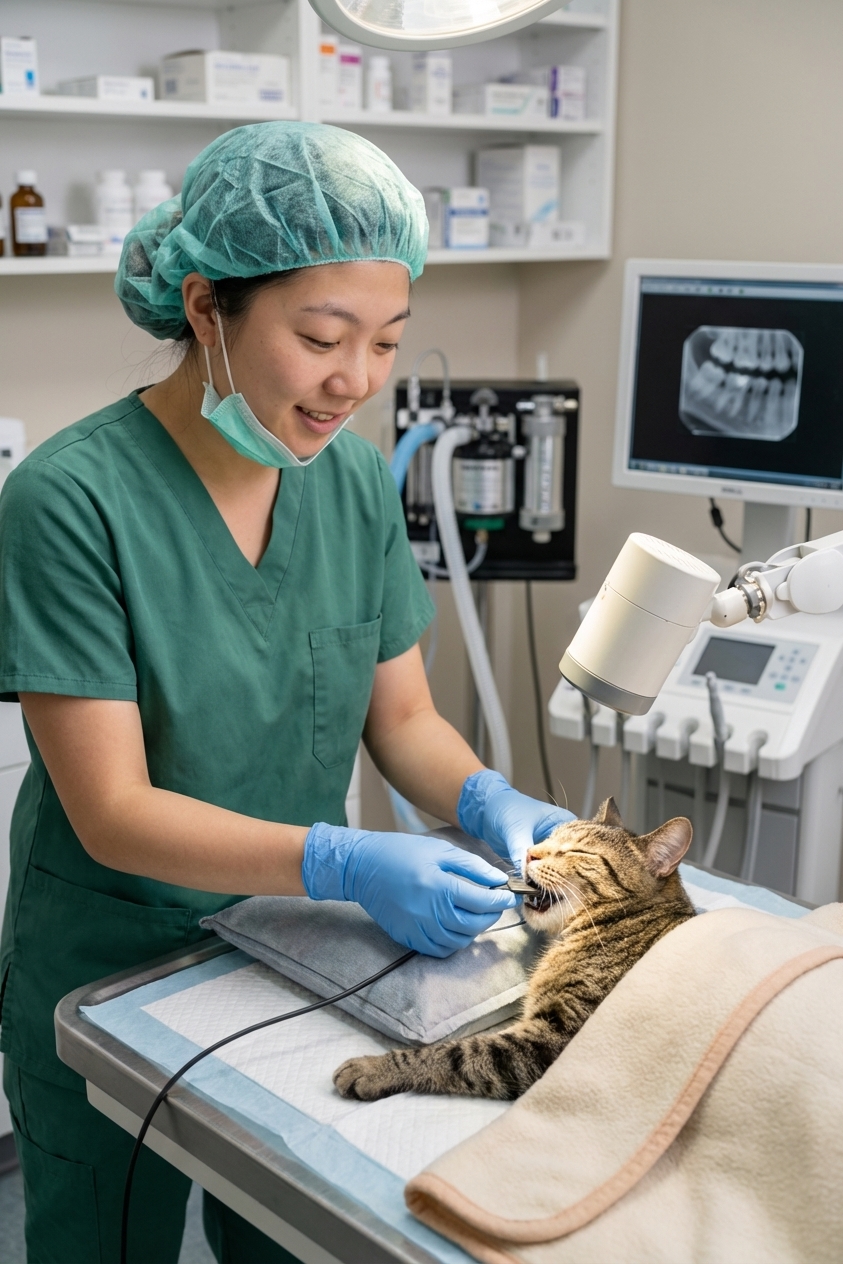
Treatment options
I know “extraction” can sound scary, especially if you are picturing what a tooth removal feels like in a human. The key difference is this: the tooth being treated is already painful. Definitive dental treatment is how we remove the pain source.
Why fillings do not work
In cats, resorptive disease is not just a surface cavity. The body is actively breaking the tooth down. If you simply patch the surface, the resorption process usually continues underneath.
Common treatments
- Surgical extraction: very common, especially for Type 1 lesions where the root must be removed
- Crown amputation: can be appropriate for some Type 2 lesions when dental radiographs confirm the roots are undergoing replacement resorption and there is no radiographic evidence that would require full extraction
Pain control and recovery
Most cats feel noticeably better once the painful tooth is addressed. Your veterinarian will typically send home:
- Pain medication for several days (sometimes longer)
- Soft food instructions during healing
- Antibiotics only when indicated (for example, certain infections or significant inflammation). Antibiotics are case-dependent and not a substitute for definitive dental treatment.
Many cat parents are surprised by how quickly their cat returns to normal behaviors, and sometimes they realize their cat had been “quietly uncomfortable” for a long time.
What to expect at a dental
If you have never had a cat go through a professional dental procedure, here is what it often looks like (details vary by clinic):
- Pre-anesthetic planning: physical exam, and commonly bloodwork based on age and health history
- Anesthesia and monitoring: careful monitoring of heart rate, breathing, oxygenation, temperature, and blood pressure
- Full-mouth dental radiographs: to find lesions and plan treatment
- Dental cleaning and charting: probing, measuring, and recording findings
- Local anesthesia (nerve blocks): frequently used to improve comfort during and after extractions
- Definitive treatment: extraction and/or crown amputation depending on what radiographs show
- Same-day discharge: many cats go home the same day with pain control and feeding instructions
If you are nervous, that is normal. Ask your clinic how they monitor anesthesia and what pain-control steps they use. Those conversations help a lot.
Long-term outlook
The prognosis after proper treatment is generally excellent for comfort and quality of life. Cats can eat well even with fewer teeth, and many do great on both wet and dry diets once they are healed.
What you do want to keep in mind is that tooth resorption can be a progressive condition. Treating the affected tooth does not guarantee that another tooth will not develop lesions later.
Long-term plan
- Regular dental exams: ask your vet how often your cat should be checked based on age and history
- Dental radiographs as recommended: especially if your cat has had resorption before
- At-home monitoring: watch for subtle eating changes, drooling, or jaw chattering
- Dental-friendly routine: tooth brushing (if your cat tolerates it), VOHC-accepted dental diets or treats, and water additives recommended by your veterinarian
When to call your vet
Please contact your veterinarian promptly if you notice:
- Not eating for 24 hours (or any time in a kitten or medically fragile cat)
- Open-mouth breathing, significant facial swelling, or bleeding
- Crying out when eating or sudden aggression when the face is touched
- Drooling that is heavy, foul-smelling, or blood-tinged
Dental pain is not just uncomfortable. It can lead to weight loss, stress, and worsening inflammation in the mouth.
Questions to ask
- Will you be taking full-mouth dental radiographs?
- How many teeth look suspicious for resorption?
- Do the lesions look more like Type 1, Type 2, or mixed changes?
- What pain medications will my cat receive during and after the procedure?
- What should my cat eat during recovery, and for how long?
- How often should we recheck to catch new lesions early?

The takeaway
Tooth resorption is one of the most common dental diseases in cats, and it is a leading reason we end up removing teeth: it hurts. If you have noticed drooling, head tilting while eating, jaw chattering, or any subtle change in your cat’s appetite or attitude, you are not being “overly worried.” You are paying attention.
With dental radiographs, an appropriate treatment plan, and good pain control, most cats recover beautifully and feel better than they have in a long time.
References
- American Veterinary Dental College (AVDC). Feline Tooth Resorption (client education resources).
- International feline dentistry literature describing TR classification and prevalence variability by age and study population.



