SRMA in Dogs: Neck Pain and Fever

Steroid-Responsive Meningitis-Arteritis, usually shortened to SRMA, is one of those conditions that can feel like it comes out of nowhere. A previously happy, bouncy young dog suddenly acts painful, stiff, and miserable. You may see fever that comes and goes, a tucked posture, and a very specific complaint: they do not want to lower their head to eat, sniff, or take treats.
As a veterinary assistant, I want you to hear this clearly: SRMA is treatable, and many dogs do very well, but early ER care matters. Severe pain and high fever can escalate quickly, and a fast diagnosis helps your veterinarian start the right therapy and rule out other emergencies that can look similar.
Quick note: This article is for education and support, not a diagnosis. Neck pain and fever need a veterinarian’s hands-on exam.

What SRMA is
SRMA is an immune-mediated inflammatory disease that affects the membranes around the brain and spinal cord and the blood vessels associated with them. In day-to-day terms, it causes:
- Intense neck pain
- Fever that may spike and then settle
- Systemic inflammation, which can make dogs act profoundly tired or “not themselves”
SRMA is not the same thing as “regular arthritis” or a simple muscle strain. It is also different from seizure disorders. Most SRMA dogs are painful and febrile, not having convulsions.
Signs at home
The most common SRMA story I hear sounds like this: “My dog was fine yesterday, and today they will not move their neck.” These are the signs that should put SRMA on the radar, especially in young dogs:
- Sudden neck pain, often severe. Dogs may yelp when picked up or when turning their head.
- Reluctance to lower the head to eat from a bowl, sniff the ground, or grab a toy.
- Stiff, hunched posture, sometimes with a rigid gait.
- Fever. You might notice hot ears, panting at rest, shivering, or your dog seeking cool floors.
- Lethargy and not wanting to play, even in normally high-energy pups.
- Reduced appetite, sometimes because bending the neck to eat hurts.
Some dogs also develop a painful, tight abdomen or look generally uncomfortable all over. That can happen because inflammation does not always stay in one place.

Why young dogs
SRMA is classically seen in young dogs and is thought to involve an abnormal immune response. Certain breeds and mixes are reported more often, including beagles and boxers. Other medium to large breeds, including Bernese mountain dogs, have also been reported, but any breed or mix can be affected.
If your dog is under about 2 years old and has neck pain plus fever, SRMA becomes a more important “rule-out.”
When to go to the ER
Neck pain can have many causes, ranging from mild strain to spinal cord injury or serious infection. SRMA itself is painful and inflammatory, and it also overlaps with other conditions that can be dangerous if delayed.
Go to an emergency vet today if you see:
- Severe neck pain (crying out, trembling, unable to settle)
- Fever, especially if your dog feels very hot or is profoundly lethargic
- Weakness, wobbliness, collapse, or trouble standing
- Signs of shock such as pale gums, rapid breathing, or extreme weakness
- Any history of trauma (fall, rough play, hit by car) combined with neck pain
If you are unsure, call your vet or an ER and describe two key details: neck pain severity and possible fever. Those two pieces of information help triage quickly.
If your dog is painful and febrile, it is safer to assume it is urgent until a veterinarian proves otherwise.
What vets rule out
SRMA can mimic, and be mimicked by, other serious problems. Your veterinary team may discuss several possibilities, such as:
- Disk disease (intervertebral disk herniation), which can cause neck pain and neurologic deficits
- Infectious meningitis (bacterial, fungal, tick-borne causes), which needs different treatment than SRMA
- Neck trauma or vertebral injury
- Immune-mediated polyarthritis, which can cause fever and pain, sometimes shifting between legs
- Cervical spondylomyelopathy (wobbler) in some larger breeds, which can cause neck pain and wobbly walking
- Other inflammatory brain or spinal cord disease, including conditions within the meningoencephalitis spectrum
- Deep infections near the throat or ears (such as middle or inner ear disease or a retropharyngeal abscess) that can occasionally present as neck pain
This is why “just trying steroids at home” without diagnostic guidance can be risky. Steroids can temporarily mask signs of infection and delay the correct care.
How SRMA is diagnosed
SRMA diagnosis is usually a combination of clinical pattern and testing. Many dogs need a referral hospital or specialty center because the most informative tests require advanced equipment and careful monitoring.
Common tests include:
- Physical and neurologic exam to localize pain and check for deficits
- Temperature check to document fever
- Bloodwork (CBC and chemistry). SRMA often shows a strong inflammatory pattern, such as elevated white blood cells and elevated inflammatory markers (acute-phase proteins such as CRP).
- Infectious disease testing based on region and risk, including tick-borne disease screening where appropriate
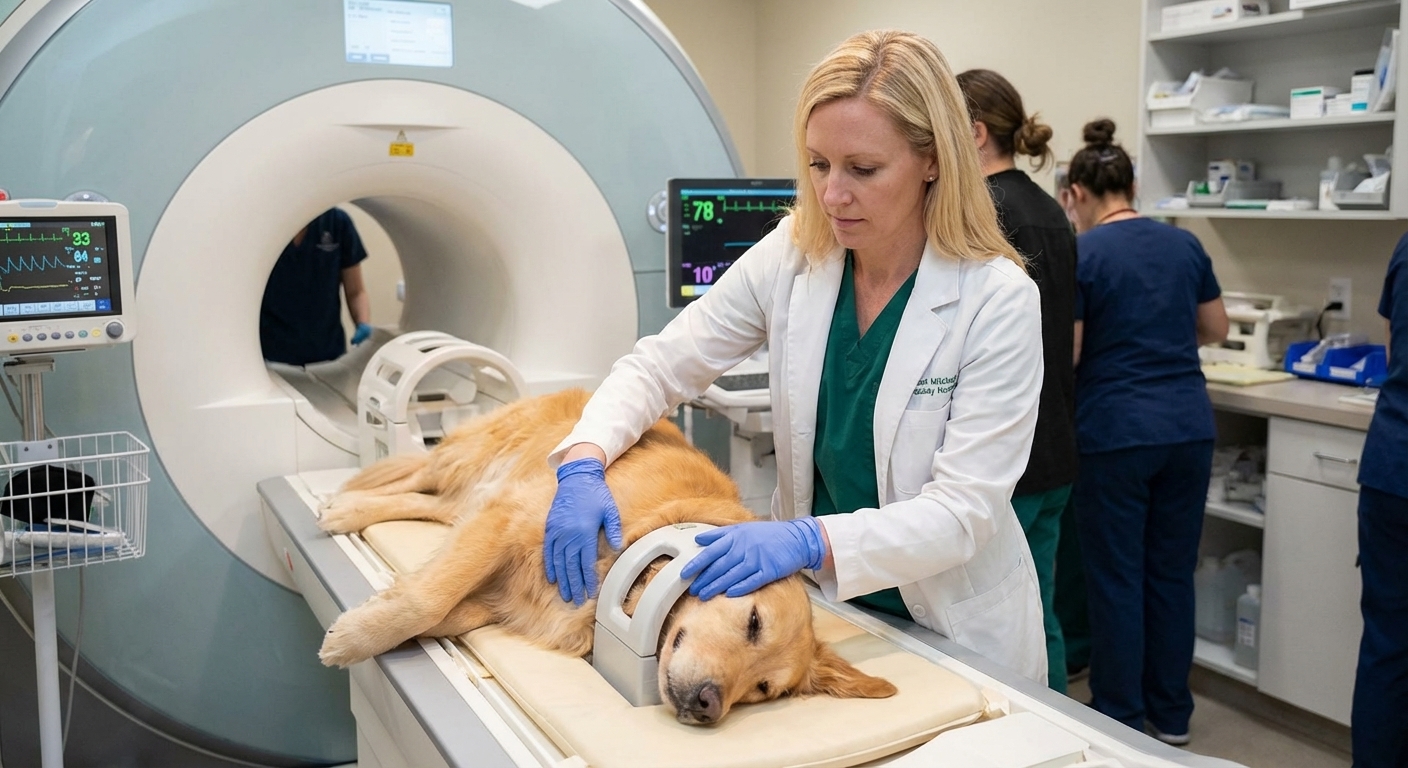
- Advanced imaging like MRI to evaluate the neck and rule out structural causes
- CSF tap (cerebrospinal fluid analysis) to look for characteristic inflammation and to help distinguish SRMA from infectious causes
- Optional adjunct testing in some cases, such as serum or CSF IgA levels, depending on the clinician and lab availability. This is not required for diagnosis.
A CSF tap is one of the key reasons dogs may be referred. It is typically performed under anesthesia with strict safety protocols, often after imaging confirms it is appropriate to proceed.
Treatment
SRMA is called “steroid-responsive” because many dogs improve dramatically once the immune overreaction is controlled. Treatment is not always one-and-done, though. It commonly involves:
- Immunosuppressive corticosteroids (often prednisone or prednisolone) at an initial high dose
- A slow, veterinarian-guided taper over weeks to months, and often several months, to reduce relapse risk
- Pain control, sometimes including additional medications early on
- Hospitalization if pain, fever, or dehydration is significant
- Recheck exams and repeat bloodwork to monitor response and side effects
Timeline: many dogs improve within 24 to 72 hours once the correct therapy is started, but not every case follows the textbook. Some dogs need medication adjustments, longer courses, or additional immunosuppressants.
Relapses can happen, especially if steroids are stopped too soon or tapered too quickly. That taper period is not optional, even when your dog seems “back to normal.”
At-home care
Once your veterinarian has diagnosed SRMA and started treatment, your job becomes supportive care and careful observation.
Helpful, practical steps:
- Use a harness, not a neck collar, to avoid pressure on a painful neck.
- Elevate food and water bowls so your dog does not have to lower the head.
- Keep activity calm and controlled, with short leash potty breaks.
- Give medications exactly as prescribed. If you miss a dose or your dog vomits a dose, call your vet for instructions.
- Track symptoms daily: appetite, energy, neck stiffness, temperature if instructed, and any side effects.
Steroids can cause increased thirst, urination, panting, appetite changes, and restlessness. These can be expected, but your veterinarian still needs to know if side effects are intense or worsening.
Because steroids suppress the immune system, your dog can be more prone to infections while on treatment. Call your vet promptly if you notice new cough, nasal discharge, painful urination, skin lesions, or any sudden decline.

What not to do
- Do not force neck movement to “check range of motion.” Pain responses can be strong.
- Do not give leftover human pain meds. Many are toxic to dogs.
- Do not give NSAIDs unless your veterinarian specifically instructs you to, especially if your dog is receiving steroids. Combining NSAIDs and steroids can cause serious GI ulceration and bleeding.
- Do not delay care because symptoms fluctuate. Fever and pain can come and go.
- Do not start steroids without veterinary guidance if infection has not been ruled out.
Go back to the ER urgently if your dog has black, tarry stool, vomiting or diarrhea with blood, repeated vomiting, severe weakness, collapse, or worsening pain despite medication.
Questions to ask
If you are in the exam room and feeling overwhelmed, these questions can keep things clear:
- What are the top conditions you are considering and why?
- Does my dog have a documented fever right now?
- Do you recommend MRI, a CSF tap, or both?
- Which infectious diseases do you need to rule out in our area?
- What is the plan for pain control tonight?
- How long do you expect treatment and tapering to take for my dog?
- What signs should send us back to the ER during recovery?
The bottom line
SRMA is a serious, painful inflammatory condition that often affects young dogs and commonly shows up as severe neck pain plus fever and a dog who keeps their head and neck very stiff. The encouraging part is that with prompt veterinary evaluation, appropriate testing, and a careful treatment plan, many dogs recover and return to their normal selves.
If your dog is painful, feverish, or suddenly stiff through the neck, trust your instincts and seek urgent veterinary care. Early intervention can mean faster relief and fewer complications.
