Hemangiosarcoma can hide until a sudden crisis. Learn early warning signs, emergency rupture symptoms, how vets diagnose and stage HSA, treatment options, pr...
Article
•
Designer Mixes
Splenic Tumors in Dogs: Symptoms, Emergencies, and Treatment

Shari Shidate
Designer Mixes contributor
As a veterinary assistant, I have seen how quickly a “normal day” can turn into an emergency when a dog has a splenic mass. The tricky part is that splenic tumors may not cause obvious signs until bleeding occurs, and then the symptoms can look like sudden weakness, collapse, or a dog who “just seems off.”
This article will walk you through what splenic masses are (benign vs malignant), the subtle early signs many families miss, the red-flag emergency symptoms of rupture, how veterinarians diagnose the problem, what to expect at the ER, what splenectomy recovery looks like, and what prognosis typically depends on.
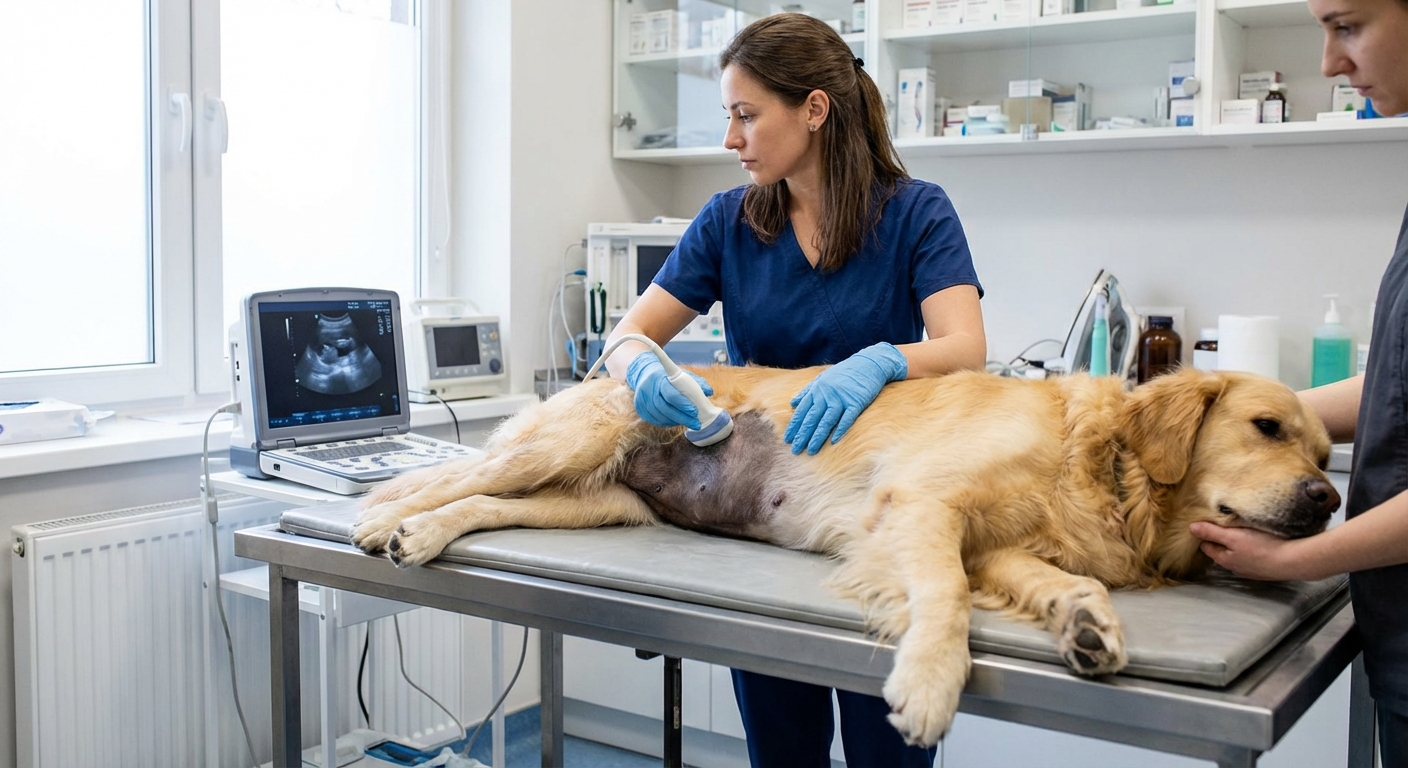
What is a splenic mass in a dog?
The spleen sits in the abdomen and helps with blood filtration and immune function. A splenic mass is an abnormal growth or lesion on (or within) the spleen. Some masses are benign, while others are malignant (cancerous).
Benign vs malignant
Many owners ask, “Is it cancer?” The honest answer is that we often cannot know with certainty from imaging alone. Your vet may be able to make a strong, educated suspicion based on ultrasound findings and the overall clinical picture, but the most reliable way to confirm the exact diagnosis is usually histopathology after the mass (or spleen) is removed.
- Benign causes may include hematomas (blood-filled areas), nodular hyperplasia (age-related benign changes), or other non-cancerous growths.
- Malignant causes commonly include hemangiosarcoma (a cancer of blood vessel cells), plus other tumor types such as lymphoma, leiomyosarcoma, and metastatic cancers that spread from elsewhere.
Why it matters: Some benign splenic masses can still bleed severely and become life-threatening, so “benign” does not always mean “safe.”
Early symptoms owners often miss
Splenic tumors can grow slowly, and early symptoms are often vague. Many families tell me they assumed their dog was just “slowing down with age.” These are the subtle signs to take seriously, especially in older, large-breed dogs:
- Lower energy or tiring faster on walks
- Decreased appetite or picky eating that is new
- Weight loss or muscle loss over weeks to months
- Intermittent weakness that improves after rest (this can happen with small bleeds that temporarily stabilize)
- Panting at rest or seeming uncomfortable without a clear reason
- Occasional vomiting or mild belly discomfort
- Gums that look lighter than usual (not always obvious unless you check)
If you have a senior dog, I recommend getting comfortable doing quick “home health checks” a couple of times a week: gum color, breathing rate at rest, appetite, and overall energy.
Emergency signs of rupture
A splenic mass can rupture and bleed into the abdomen, causing hemoperitoneum (blood in the belly). This is an emergency. Dogs can deteriorate fast.
Go to an ER now if you notice
- Collapse or sudden inability to stand
- Pale, white, or gray gums
- Weakness, stumbling, or “drunk-looking” walking
- Abdomen that can look swollen or suddenly bigger than usual
- Rapid breathing or labored breathing
- Rapid heart rate or a pounding heartbeat
- Cold legs, ears, or paws (poor circulation)
- Sudden restlessness or inability to get comfortable
If your dog is weak and has pale gums, do not wait it out. Internal bleeding is not something you can safely monitor at home.
What to do on the way: Keep your dog warm, limit movement, and head in immediately. If possible, call the ER while driving so they can prepare. Do not give human pain medication.
Which dogs are most at risk?
Splenic masses can occur in any dog, but they are especially common in middle-aged to senior dogs and in large and giant breeds. In practice, we often see these cases in dogs like (including but not limited to):
- German Shepherd Dogs
- Golden Retrievers
- Labrador Retrievers
- Boxers
- Bernese Mountain Dogs
- Great Pyrenees
- Doberman Pinschers
Breed risk depends on the tumor type, and lists can vary by study and region. If you have an older, large-breed dog, it is worth taking vague symptoms seriously even if your dog is not on any “classic” list.
That said, smaller dogs can absolutely develop splenic tumors too.
How vets diagnose splenic masses
Diagnosis usually happens in one of two ways: either a mass is found incidentally during an exam or imaging, or the dog comes in unstable due to bleeding.
Common diagnostic steps
- Physical exam: checking gum color, heart rate, belly pain or distension, and overall stability
- Bloodwork: CBC and chemistry to evaluate anemia, platelet levels, organ function, and overall surgical safety
- Clotting tests (in some cases): especially if bleeding risk is a concern
- Abdominal ultrasound: often the most helpful test to identify a splenic mass and look for abdominal fluid that could be blood
- FAST scan (focused ultrasound): a quick “is there fluid?” check often used in emergencies
- Abdominocentesis (belly tap): sampling abdominal fluid to see if it is blood
- X-rays and chest imaging: used to look for evidence of spread to the lungs or other concerns
- ECG: some dogs (especially after bleeding) can develop heart rhythm abnormalities
Can a needle sample confirm cancer?
You may hear a few different terms here, and they matter:
- Fine needle aspirate (FNA): a small needle is used to collect cells for cytology. This is more common than true biopsy.
- Core biopsy: a larger needle is used to collect a tissue sample. This typically carries a higher bleeding risk in the spleen.
FNAs of splenic masses can be helpful in some situations, but they can also be non-diagnostic, and splenic tissue can bleed. Practices vary, and many clinicians avoid aspirating a mass that looks highly suspicious for hemangiosarcoma because of hemorrhage risk and because results are often low yield.
Importantly, cytology is more likely to identify certain cancers (for example, some round cell tumors such as lymphoma or mast cell tumor) than it is to definitively confirm hemangiosarcoma. In some cases, lymphoma or other round cell tumors can be diagnosed on cytology without splenectomy. In many cases, though, the clearest answer still comes from histopathology after surgical removal.
What else can look similar?
I also like to say this out loud, especially when families are understandably terrified: a splenic mass is not the only cause of blood in the abdomen or sudden collapse.
Some common “look-alikes” or related emergencies include:
- Trauma (hit by car, fall, dog fight injuries) that causes internal bleeding
- Coagulopathies (clotting disorders), including rodenticide toxicity
- Splenic torsion (twisting of the spleen), which can cause shock and abdominal pain
- Liver masses or other abdominal tumors that bleed
This is one reason vets lean on ultrasound, bloodwork, and abdominal fluid analysis before making big decisions when time allows.
What happens at the ER
If your dog comes in weak, pale, or collapsed, the ER team usually moves fast and in a fairly predictable order. Knowing the “why” can make it a little less scary.
A typical ER flow
- Triage and vitals: gum color, heart rate, breathing, temperature, blood pressure
- IV catheter: for fluids, medications, and blood draws
- Quick labs: often PCV/TS (red blood cell level and protein), lactate, glucose, and sometimes a quick platelet estimate
- FAST scan: to check for abdominal fluid
- Stabilization: pain control, oxygen, and fluid therapy and/or blood products depending on shock severity (when hemorrhage is significant, transfusion is commonly prioritized)
- Decision point: if bleeding is suspected and your dog is a surgical candidate, the team may recommend urgent surgery (splenectomy)
You may be asked to make rapid choices about diagnostics, transfusion, and surgery. It is okay to ask for a clear explanation of the goal of each step and what information it will change.
Treatment options
Treatment depends on your dog’s stability, the appearance of the mass, and whether there are signs of spread.
Emergency stabilization
If a dog is actively bleeding, the medical team may start:
- IV fluids and/or blood products as needed to support circulation
- Blood transfusion if anemia is severe or shock is worsening
- Oxygen support
- Pain control (dog-safe medications)
- Fast-track surgery planning if the dog is a surgical candidate
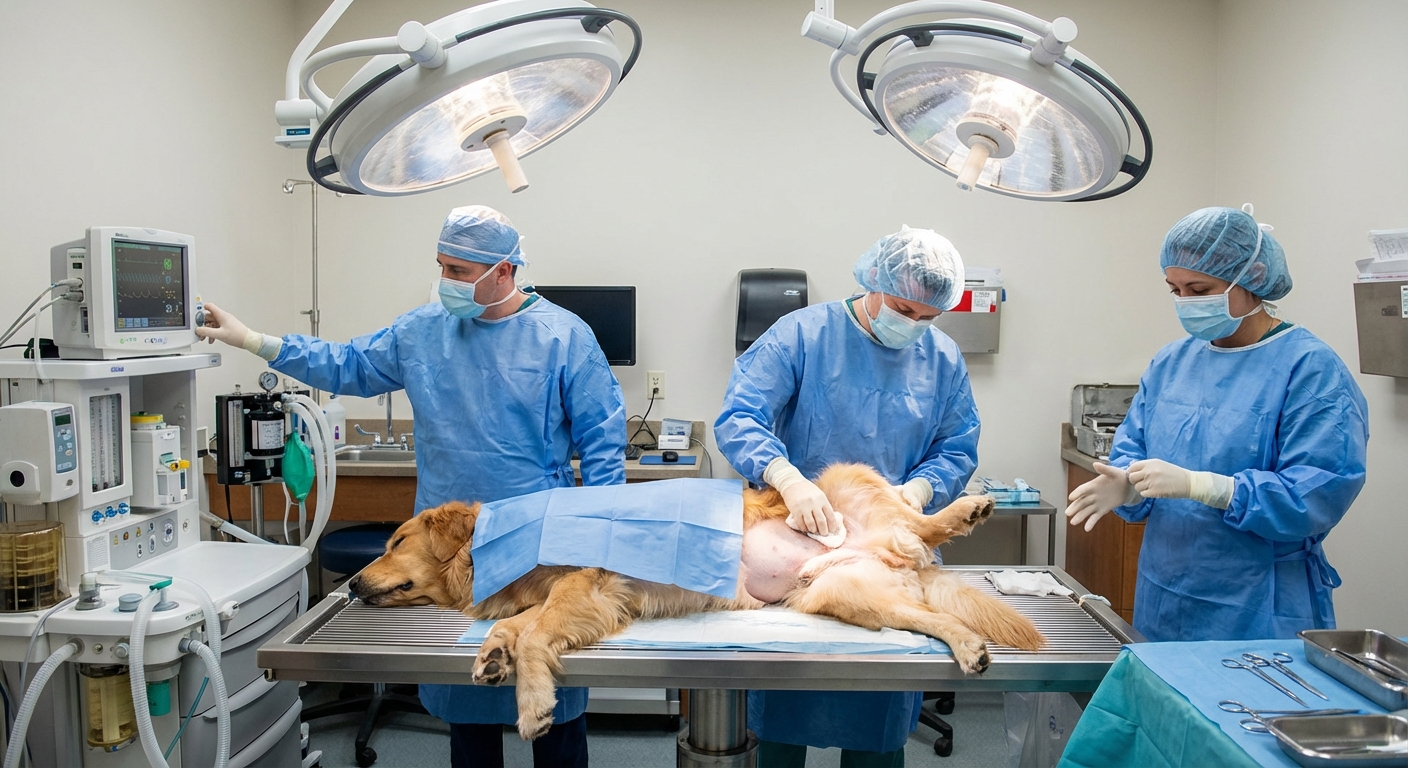
Splenectomy (spleen removal)
A splenectomy is the most common treatment for a splenic mass, especially when bleeding is suspected or confirmed. Dogs can live without a spleen, and many feel noticeably better once they recover, especially if the mass was causing chronic blood loss or discomfort.
Chemotherapy and additional care
If the tumor is malignant, especially hemangiosarcoma, an oncologist may recommend chemotherapy after surgery. Chemo in dogs is usually aimed at maintaining quality of life, and most dogs tolerate it better than many people expect.
Cost note
Costs vary widely by region, whether your dog needs a transfusion, and whether this is emergency after-hours surgery. If money is part of the decision (and for most families it is), tell the team early. A good ER will talk through options, expected ranges, and what each option changes.
Splenectomy recovery
Recovery varies by dog, but here is what most families can plan for after splenectomy.
The first 24 to 72 hours
- Sleepiness and reduced appetite are common
- Your dog may need help standing and walking at first
- Some dogs have mild nausea from anesthesia or pain meds
Activity restrictions
Most veterinarians recommend strict rest for about 10 to 14 days, sometimes longer depending on incision healing and how complicated the surgery was.
- Short leash walks only for potty breaks
- No running, jumping, stairs (when possible), or rough play
- Use a cone or recovery collar to prevent licking the incision
Recheck timeline
Most dogs need a recheck visit to assess healing, and if your dog has external skin sutures or staples, removal is often around 10 to 14 days after surgery. Your clinic will give you a specific plan based on the incision and your dog’s progress.
What to watch for
In addition to incision issues, these are some post-op concerns your vet may warn you about:
- Ongoing or recurrent weakness (could indicate anemia or continued bleeding)
- Pale gums
- Swollen abdomen
- Fast breathing or struggling to breathe
- Irregular heartbeat or sudden fainting (some dogs develop arrhythmias after major bleeding or surgery)
- Fever, worsening lethargy, or foul-smelling incision discharge (possible infection)
Home monitoring checklist
- Check the incision twice daily for redness, swelling, discharge, or opening
- Monitor gum color and energy level
- Watch for vomiting, refusal to eat longer than a day, or worsening weakness
- Take all medications exactly as prescribed
Call your veterinarian right away if you see pale gums, a swollen abdomen, collapse, trouble breathing, black tarry stool, or bleeding from the incision.

Prognosis
Prognosis depends on several factors: the tumor type, whether it ruptured, whether there is evidence of spread, and your dog’s overall health. Your veterinary team will be the best source of realistic expectations for your dog specifically.
Benign lesions
If the mass is benign and fully removed, many dogs do very well and can return to a normal quality of life after recovery.
Hemangiosarcoma
Hemangiosarcoma is, unfortunately, one of the most aggressive splenic cancers. Even with surgery, it often has already spread microscopically by the time it is discovered. Chemotherapy may extend survival time for some dogs and can support comfort, but outcomes are still guarded overall.
If you see survival timelines online, you will notice they vary a lot. That is because factors like rupture, staging results, heart rhythm, and response to treatment can change the picture. If you want numbers, ask your vet or oncologist to share typical ranges based on current studies and your dog’s staging results.
Other malignant tumors
Lymphoma and other sarcomas can vary widely. Some respond to chemotherapy or other targeted plans. The most helpful next step is usually a clear staging plan (often including chest imaging and sometimes additional ultrasound evaluation) and a consultation with oncology once biopsy results return.
Staging after surgery
After splenectomy, many teams recommend some version of “staging” to look for spread and to guide next steps. This often includes chest imaging, an abdominal ultrasound review, and, in select cases, an echocardiogram.
The most compassionate north star is quality of life. A good veterinary team will help you weigh time, comfort, cost, and what your dog is telling you day to day.
Questions to ask your vet
When you are stressed, it is easy to forget what you wanted to ask. Here are practical questions you can bring to the appointment or ER:
- Is my dog stable right now, or actively bleeding?
- Do you see abdominal fluid, and does it look like blood?
- What tests do you recommend today, and what can wait?
- Is surgery recommended, and what are the biggest risks for my dog specifically?
- Will my dog likely need a transfusion?
- Can you send the spleen for histopathology automatically?
- If it is malignant, what staging tests do you recommend?
- What does aftercare look like at home, and what signs mean “return immediately”?
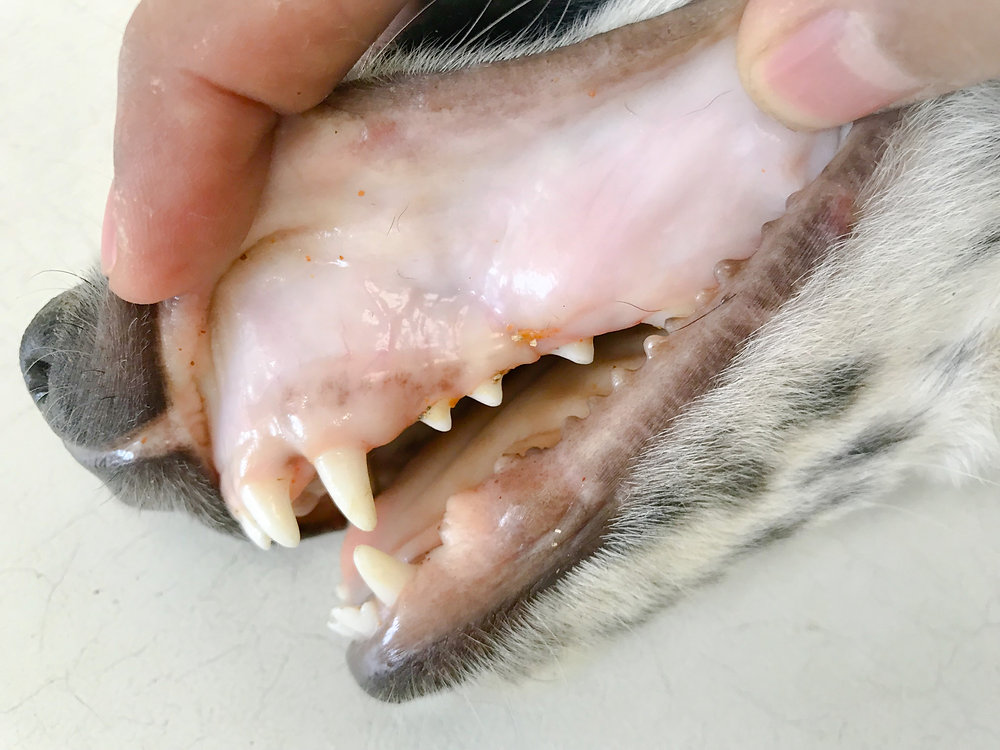
When in doubt, check gum color
If you take only one actionable tip from this page, let it be this: learn your dog’s normal gum color. Healthy gums are usually bubblegum pink (pigmented gums are a separate conversation). Pale gums combined with weakness is one important at-home warning sign that a dog may be in trouble and needs urgent veterinary care.
If your dog is older, large-breed, and suddenly weak, do not assume it is “just age.” It is always safer to let a veterinary team rule out a serious problem than to miss a narrow window for treatment.
Medical disclaimer: This content is for education and is not a substitute for veterinary diagnosis or treatment. If you think your dog is having an emergency, seek veterinary care immediately.



