Rocky Mountain Spotted Fever in Dogs

Ticks can carry several different diseases, and they do not all behave the same way. Rocky Mountain spotted fever (RMSF) is one of the most urgent tick-related illnesses we see discussed in veterinary medicine because dogs can get very sick very fast without treatment.
This page is here to help you recognize the classic signs, understand the testing process, and know what to do next. It is educational only and not a substitute for veterinary care. If you suspect RMSF, call your veterinarian or an emergency clinic right away.
What is RMSF?
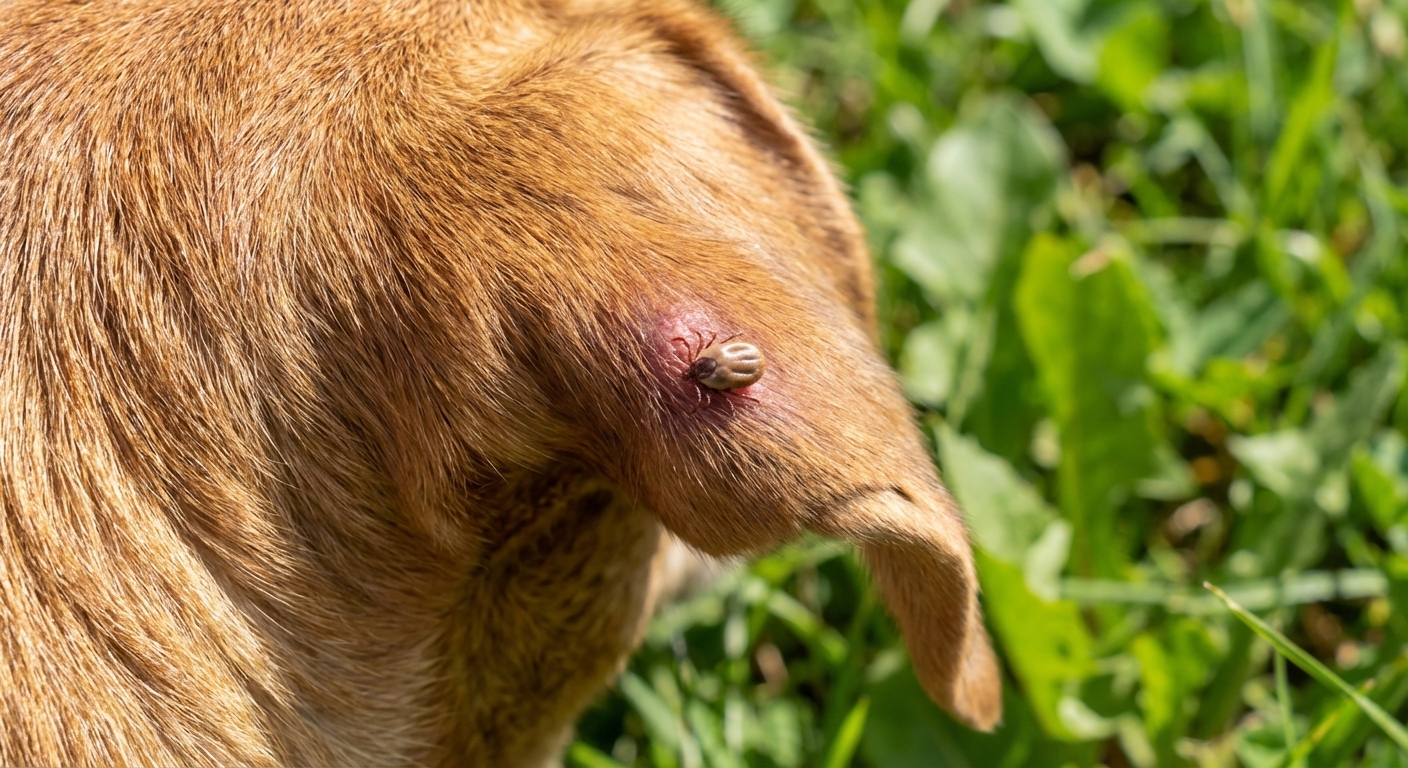
Rocky Mountain spotted fever is caused by a bacterium called Rickettsia rickettsii. Dogs get infected after being bitten by an infected tick. Despite the name, RMSF is not limited to the Rocky Mountain region. Cases are reported across the U.S., including the South and Midwest, and risk can vary year to year based on tick activity.
RMSF is distinct from Lyme disease and Ehrlichiosis. They are all tick-borne, but they involve different organisms, can have different timelines, and can affect the body differently. Practically speaking, that means a dog can look “tick sick” and still need targeted testing and treatment decisions from a veterinarian.
- RMSF: often a sudden, flu-like illness with fever, pain, and possible bleeding or neurologic signs if severe.
- Lyme disease: commonly associated with lameness that may shift legs, fever, and lethargy; many dogs exposed never show signs.
- Ehrlichiosis: can cause fever, low platelets, bruising or bleeding, and can become chronic if untreated.
Because signs overlap, it is very normal for vets to consider multiple tick-borne infections at the same time, especially if your dog has had tick exposure.
How dogs get infected
RMSF is transmitted through tick bites. In the U.S., major vectors include the American dog tick (Dermacentor variabilis), the Rocky Mountain wood tick (Dermacentor andersoni), and in some regions the brown dog tick (Rhipicephalus sanguineus). Which ticks matter most depends on where you live and where your dog spends time.
The key takeaway is this: you do not need to find a tick to have a tick-borne infection. Ticks can be missed, they can fall off, and some dogs have thick coats that make detection difficult.
If your dog spends time in tall grass, brushy trails, wooded areas, hunting areas, or even suburban yards with wildlife traffic, tick prevention is worth taking seriously.

RMSF symptoms in dogs
Many dogs start with vague signs that can look like a common virus or simple stomach upset. What raises concern is tick exposure risk plus a fast change in your dog’s energy, appetite, comfort, and temperature.
Common early signs
- Fever (often significant, and many vets consider over about 103°F (39.4°C) concerning, depending on the dog and how the temperature was taken)
- Lethargy, “not themselves,” hiding, sleeping more
- Decreased appetite
- Muscle or joint pain (reluctance to move, stiffness, whining when picked up)
- Vomiting and sometimes diarrhea
- Swollen lymph nodes
Signs that can suggest more severe disease
- Bruising on the skin or gums, tiny red or purple dots (petechiae)
- Nosebleeds or bleeding gums
- Eye changes (redness, discharge, squinting, vision concerns)
- Neurologic signs (stumbling, tremors, seizures, marked weakness)
- Labored breathing or collapse
People often ask about a “spotted” rash like humans can get. Dogs can develop skin findings, but it is not reliable and is easy to miss under fur. In dogs, we focus more on fever, pain, low platelet related bleeding signs, and overall illness.
A quick note about household risk: Dogs do not directly transmit RMSF to people, but ticks that hitch a ride indoors can bite humans. Tick control on pets and safe tick removal help protect the whole household.
Timeline
Here is a practical timeline that many veterinarians use when thinking about RMSF. Individual dogs vary, and co-infections can change the picture, so think of this as a guide, not a guarantee.
After the tick bite
- Incubation period: often about 2 to 14 days from tick bite to symptoms, and sometimes longer (some references cite up to roughly 21 days).
Early illness
- Fever, low energy, and pain tend to be the most noticeable.
- Some dogs have vomiting, decreased appetite, and general flu-like signs.
Progression if untreated
- Inflammation of blood vessels can lead to complications, including bruising or bleeding, organ stress, and neurologic signs.
- This is why vets often treat suspected RMSF promptly rather than waiting weeks for perfect proof.
After starting treatment
- With appropriate antibiotics, dogs often begin to improve within 24 to 48 hours, but severe cases may take longer and some dogs need hospitalization and supportive care.
- If your dog is not improving on schedule, your vet may recheck labs, look for complications, or consider additional diagnoses.
If your dog has a fever and a sudden drop in energy after possible tick exposure, it is worth calling your vet the same day. When it comes to RMSF, time matters.
When to seek emergency care
Veterinarians often tell families this: it is better to be “too cautious” with tick-borne infections than to wait and hope. Seek urgent or emergency veterinary care if you notice any of the following:
- Difficulty breathing, collapse, severe weakness, or inability to stand
- Seizures, severe disorientation, or sudden loss of coordination
- Bleeding from the nose or mouth, black tarry stool, or widespread bruising
- Very pale gums or gums that look white or gray
- Repeated vomiting, inability to keep water down, or signs of dehydration
- Known tick bite plus a high fever and marked lethargy

How vets test for RMSF
Diagnosis is a combination of history, physical exam, and testing. Because early RMSF can look like several illnesses, your vet may recommend a broader fever and tick-borne workup, especially if your dog is very uncomfortable or has abnormal bleeding signs. Other non tick causes of similar signs (like pancreatitis, other infections, or gastrointestinal disease) can also be on the list, which is another reason an exam matters.
History and exam
- Tick prevention used or not used
- Recent hiking, boarding, grooming, wildlife exposure, travel
- Fever, pain, bruising, neurologic changes
Common lab findings
- Low platelets (thrombocytopenia) is common in many tick-borne diseases and can help explain bruising or bleeding.
- Changes in white blood cells or red blood cells
- Elevated liver values or other signs of inflammation
- Urinalysis changes if kidneys are stressed
RMSF specific testing
- Antibody testing (serology): Antibodies can take time to rise, so an early test may be negative even when a dog is truly infected. Many vets recommend paired titers (an initial sample and another sample 2 to 3 weeks later). A fourfold rise between samples supports recent infection. A single positive antibody test can sometimes reflect past exposure rather than current illness, so results must be interpreted in context.
- PCR testing: Looks for the organism’s DNA. PCR can be helpful, but results depend on timing and sample, and a negative PCR does not always rule RMSF out.
Because waiting can be risky, many veterinarians start treatment when suspicion is high, even while results are pending. This is common in responsible tick-borne care.
Treatment overview
Only a veterinarian can diagnose and treat RMSF. That said, it helps to know what typical treatment looks like so you are not caught off guard.
Antibiotics
Doxycycline is commonly considered the first-line antibiotic for RMSF and several other tick-borne infections. Course length varies by case, but many dogs are treated for roughly 10 to 14 days (and sometimes longer if your veterinarian recommends it). Do not give leftover antibiotics or human medications without veterinary guidance.
Supportive care
Some dogs need more than antibiotics, especially if they are dehydrated, vomiting, or showing bleeding issues.
- Fluids for hydration and organ support
- Anti-nausea medication and appetite support
- Pain control as appropriate
- Hospitalization for monitoring in severe cases
- Repeat bloodwork to track platelet count and organ values
Prognosis
Many dogs recover well when treated early. Delayed treatment increases the risk of complications. Your veterinary team can give the most accurate outlook based on exam findings and labwork.
At-home care during recovery
If your veterinarian sends your dog home on treatment, these gentle steps can help recovery stay on track:
- Give medications exactly as prescribed. If doxycycline upsets your dog’s stomach, ask your vet what to do before stopping it.
- Encourage hydration. Offer fresh water often. Ask your vet about electrolyte solutions if appetite is low.
- Keep activity calm. Short leash potty breaks and lots of rest are usually best during fever and weakness.
- Watch gums and energy. Pale gums, worsening bruising, or a sudden crash deserves a same-day call.
- Schedule rechecks. Follow-up bloodwork can be important, especially if platelets were low.
Tick prevention
The best way to avoid RMSF is to prevent tick bites. In Texas and many other states, ticks can be active for long stretches of the year.
- Use a veterinarian-recommended tick preventive consistently. The best product depends on your dog’s age, lifestyle, and health history.
- Do tick checks after outdoor time, especially around ears, under the collar, armpits, groin, and between toes.
- Keep yards less tick-friendly by trimming tall grass, reducing brush piles, and discouraging wildlife that carry ticks.
- Remove ticks promptly with fine-tipped tweezers or a tick tool, grasping close to the skin and pulling steadily. Prompt removal can reduce risk for some tick-borne infections. RMSF transmission may occur faster than Lyme disease, so do not rely on a specific time window as “safe.”

Questions to ask your vet
If RMSF is on the table, these questions can help you feel informed and steady:
- Do my dog’s signs fit RMSF, or another tick-borne disease, or more than one problem?
- What tests are you running today, and what can they miss early on?
- Are you starting doxycycline now, and for how long?
- Are my dog’s platelets low? Is there a bleeding risk?
- What symptoms mean I should go to the ER tonight?
- When should we recheck bloodwork?
The bottom line
Rocky Mountain spotted fever is a serious tick-borne illness, and it is not the same as Lyme disease or Ehrlichiosis. The signs can start out subtle, but the disease can escalate quickly. If your dog has fever, sudden lethargy, pain, vomiting, bruising, or neurologic changes after possible tick exposure, contact your veterinarian promptly or go to an emergency clinic.
With fast treatment and good supportive care, many dogs do very well. Going forward, consistent tick prevention is one of the kindest, simplest ways to protect your dog’s long-term health.
