Learn what to feed a cat with pancreatitis, from wet GI diets and hydration-boosting strategies to small frequent meals, safe transitions, and foods to avoid.
Article
•
Designer Mixes
Pancreatitis in Cats

Shari Shidate
Designer Mixes contributor
Pancreatitis in cats can feel confusing and scary because the signs are often subtle. One day your cat is a little “off,” and the next you are dealing with nausea, hiding, and a cat who just will not eat. As a veterinary assistant, I can tell you this can be an emergency, especially if your cat will not eat or is becoming dehydrated. The good news is that many cats do recover with the right veterinary plan and smart home support.
This guide will walk you through what pancreatitis is, what can trigger it, how it is treated, and practical care and training tips that make recovery less stressful for you and your cat. (This information is educational and not a substitute for diagnosis or treatment from your veterinarian.)

What it is
The pancreas is a small organ tucked near the stomach and intestines. It has two big jobs:
- Digestive help: It releases enzymes that break down fat, protein, and carbohydrates.
- Blood sugar control: It produces hormones like insulin.
Pancreatitis means inflammation of the pancreas. When the pancreas becomes inflamed, digestive enzymes can activate too early and irritate surrounding tissue. In cats, pancreatitis is often subtle and may be chronic or relapsing, though some cats can become severely ill with acute episodes.
Signs (often subtle)
Cats rarely read the textbook. Many do not vomit like dogs commonly do. The most common signs I see owners report are:
- Reduced appetite or refusing food entirely
- Hiding more than usual
- Low energy, “just not themselves”
- Nausea signs: lip smacking, drooling, sniffing food then walking away
- Dehydration
- Weight loss (especially with repeated episodes)
- Vomiting or diarrhea (may happen, but not always)
- Abdominal discomfort (some cats become grouchy when picked up)
- Fever in some cases
Important: If your cat is not eating for 24 hours, call your vet. Cats are at risk for hepatic lipidosis (fatty liver disease) when they stop eating, and that can become life-threatening. Call sooner if your cat is a kitten, a senior, diabetic, has known liver disease, or is vomiting repeatedly.
Causes and risk factors
In cats, pancreatitis is often labeled “idiopathic,” which simply means we do not find one single clear cause. Still, there are known patterns and risk factors.
1) IBD and triaditis
Cats can develop inflammation in more than one area at once, often called triaditis:
- Pancreatitis (pancreas)
- Cholangitis or cholangiohepatitis (liver and bile ducts)
- Inflammatory bowel disease (intestines)
Because these organs are connected anatomically, inflammation in one region can be associated with inflammation in the others.
2) Infections and parasites (uncommon)
Infectious causes are generally uncommon and often depend on geography and lifestyle, but they can be considered. Examples sometimes discussed include Toxoplasma gondii and certain liver flukes in endemic areas. Your vet will decide what to test for based on your cat’s history, region, and risk factors.
3) Trauma
Falls, being stepped on, or other abdominal trauma can potentially inflame the pancreas.
4) Medications and toxins
Some medications or toxins may be suspected in select cases, especially when the timing fits. Never give human medications to cats unless your veterinarian specifically instructs you to.
5) Metabolic and systemic illness
Pancreatitis can occur alongside other conditions such as diabetes mellitus or broader systemic inflammation. Sometimes it is hard to know what came first, which is why your vet often runs a wider set of tests.
How vets diagnose it
Diagnosing pancreatitis in cats usually requires combining several pieces of information. No single test is perfect.
- Physical exam and history: appetite changes, nausea, weight loss, dehydration.
- Bloodwork: checks hydration, liver values, blood sugar, electrolytes, and inflammation patterns.
- fPLI (often Spec fPL): a pancreas-focused blood test used to support diagnosis. Like any test, it can have false positives and false negatives, so it is interpreted alongside the full picture.
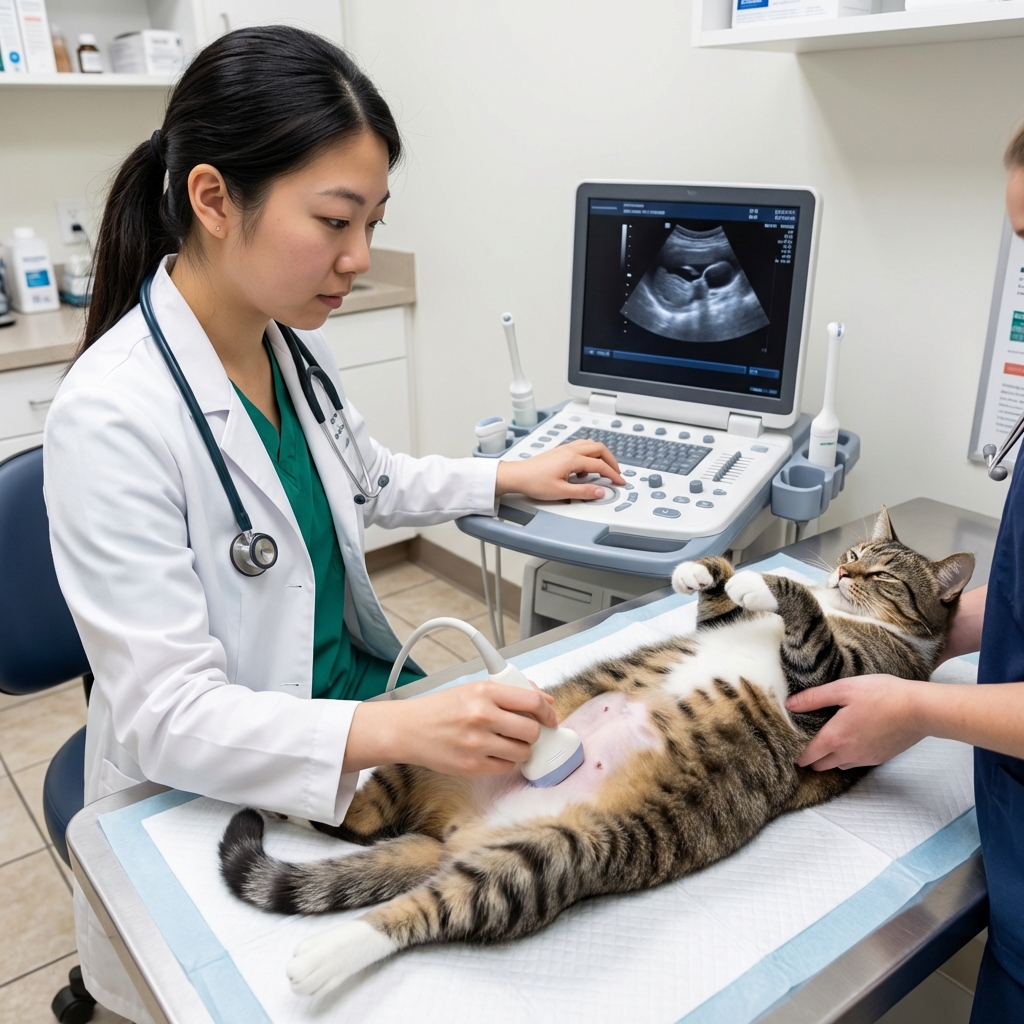
- Ultrasound: can show pancreatic swelling, fluid, or changes in nearby organs. Accuracy depends on timing and the skill of the person performing the scan.
- Rule-outs: your vet may also check for intestinal disease, liver disease, foreign material, and other causes of appetite loss.
If you are feeling frustrated by “it might be pancreatitis,” you are not alone. In cats, veterinarians often have to build the diagnosis like a puzzle.
Treatment and support
There is no one-size-fits-all treatment, because pancreatitis ranges from mild to severe, and many cats have overlapping issues. In general, treatment focuses on supporting the body while the pancreas heals.
Fluids and hydration
Dehydration makes nausea worse and slows healing. Many cats benefit from:
- IV fluids in hospital for moderate to severe cases
- Subcutaneous fluids at home for some stable cases, when your vet instructs you
Nausea control
Nausea is a huge reason cats stop eating. Your vet may prescribe anti-nausea medication to make food feel possible again. Examples your vet may choose include maropitant or ondansetron.
Pain control
Pancreatitis can be painful. Pain lowers appetite, increases stress, and slows recovery. Safe, veterinary-prescribed pain relief is one of the kindest and most important parts of care. A common example is buprenorphine, but your vet will tailor choices to your cat.
Appetite support and nutrition
In cats, not eating is dangerous. Your vet may recommend:
- Tempting foods, warmed and offered in small portions
- Prescription diets if there is concurrent GI or liver disease
- Appetite stimulants when appropriate
- Feeding tube support in some cases (this can be a lifesaver and is not a “failure”)
Antibiotics (only when indicated)
Pancreatitis itself is usually inflammatory, not automatically bacterial. Antibiotics may be used if your vet suspects infection, cholangitis, or there is another clear reason to treat.
Hospital care when needed
Some cats need hospitalization for IV fluids, injectable medications, and close monitoring. If your vet recommends it, it is typically because the risk of dehydration, electrolyte imbalance, uncontrolled pain, or not eating is high.
Possible complications to watch for
Your vet may talk with you about complications or overlapping issues such as electrolyte imbalances, worsening dehydration, diabetes onset or destabilization, and concurrent liver or intestinal inflammation.
Home care that helps
Once your cat is stable and your veterinarian sends you home with a plan, your job becomes simple but important: reduce nausea triggers, protect eating habits, and track progress.
Set up a calm space
- Choose a quiet room with a comfortable hiding option and soft bedding.
- Keep the litter box and water nearby to reduce effort.
- Separate from other pets if your cat is easily bothered.

Make food feel safe
After nausea, cats can develop food aversions. You can help by:
- Offering small meals more often instead of one large meal.
- Warming wet food slightly to increase aroma.
- Using a flat plate for cats who dislike whisker contact with bowls.
- Keeping meal time calm and predictable.
- Asking your vet before making big diet changes. Sudden switches can backfire.
Meds without a fight
This is where “training tips” matter. You are not trying to dominate your cat. You are teaching a predictable routine that reduces fear.
- Pair meds with a reward: a tiny lick of Churu-style treat, a favorite wet food, or gentle brushing right after.
- Practice calm handling: touch cheeks, lift lips briefly, then reward. Do this when you are not giving meds so it stays neutral.
- Use a towel wrap if needed: it is safer and often calmer than wrestling. Keep it quick and confident.
- Ask about compounded options: some medications can be compounded into flavored liquids or smaller capsules. Not all meds can, but it is worth asking.
Track the right things
Write notes once or twice a day. It helps you and your vet spot trends early.
- Food eaten (how much, what type)
- Water intake
- Vomiting or diarrhea
- Energy level and hiding
- Urination and stool
- Weight checks if your vet recommends it
What to expect
Many cats start to feel more interested in food over a few days once nausea and pain are controlled, but timelines vary. Your vet may recommend a recheck within days to a couple of weeks depending on severity, and sooner if appetite drops again.
Call the vet now if
Trust your instincts. Call your veterinarian or an emergency clinic if you notice:
- No eating for 24 hours, or markedly less eating for more than a day
- Repeated vomiting, especially if your cat cannot keep water down
- Signs of dehydration: tacky gums, sunken eyes, weakness
- Severe lethargy, collapse, or trouble breathing
- Yellowing of the gums, eyes, or skin (jaundice)
- Hiding plus growling or pain when touched
Pancreatitis is not a “wait and see” problem if your cat stops eating. Early support can prevent a much bigger crisis.
Diet questions
You will see a lot of advice online, and some of it is geared toward dogs. Cats are different. The “best” diet depends on whether your cat also has IBD, liver inflammation, diabetes, or food sensitivities.
General evidence-based goals many veterinarians aim for include:
- Highly digestible nutrition to reduce GI workload
- Consistent, adequate calories to help prevent fatty liver disease
- Individualized fat level based on your cat’s full medical picture (cats are not automatically placed on low-fat diets the way dogs often are)
- Wet food support when possible to improve hydration
If you want to feed homemade or add whole foods, please involve your vet or a veterinary nutritionist. Cats have very specific nutrient needs (taurine is a big one), and pancreatitis is not the time for trial-and-error diets.
Preventing flare-ups
Not every case can be prevented, but you can reduce risk and catch relapses earlier.
Stay consistent
- Keep diet changes gradual and veterinarian-guided.
- Use measured portions to maintain a healthy body condition.
Reduce stress
Stress can affect appetite and GI function. Helpful strategies include:
- Consistent feeding times
- Safe hiding spaces
- Separate resources in multi-cat homes (more than one litter box, more than one feeding station)
Do rechecks
Follow-up appointments matter, especially if your cat has recurring episodes or related issues like IBD or diabetes. Rechecks can identify weight loss, dehydration, and lab changes before your cat feels truly awful.


