Melanoma in Dogs: Mouth, Skin, and Nail Bed

Melanoma is a common tumor type in dogs, especially in the mouth, and it can look very different depending on where it shows up. As a veterinary assistant here in Frisco, Texas, I have seen how quickly families can go from “It’s probably nothing” to a scary diagnosis, especially with oral melanoma.
The most helpful thing to know right away is this: melanoma in the mouth (oral melanoma) is usually more aggressive than many melanomas found on haired skin. That said, some skin melanomas (especially those on the lips, other mucocutaneous areas, footpads, or with concerning biopsy features) can absolutely behave aggressively too. Nail bed (digital) melanoma often behaves more like oral melanoma than typical haired-skin melanoma, which is why toe and nail problems deserve extra attention.
Quick note on roles: I can help you understand what we commonly see and why vets recommend certain tests, but your veterinarian (and a board-certified oncologist if needed) will tailor diagnostics and treatment to your dog.
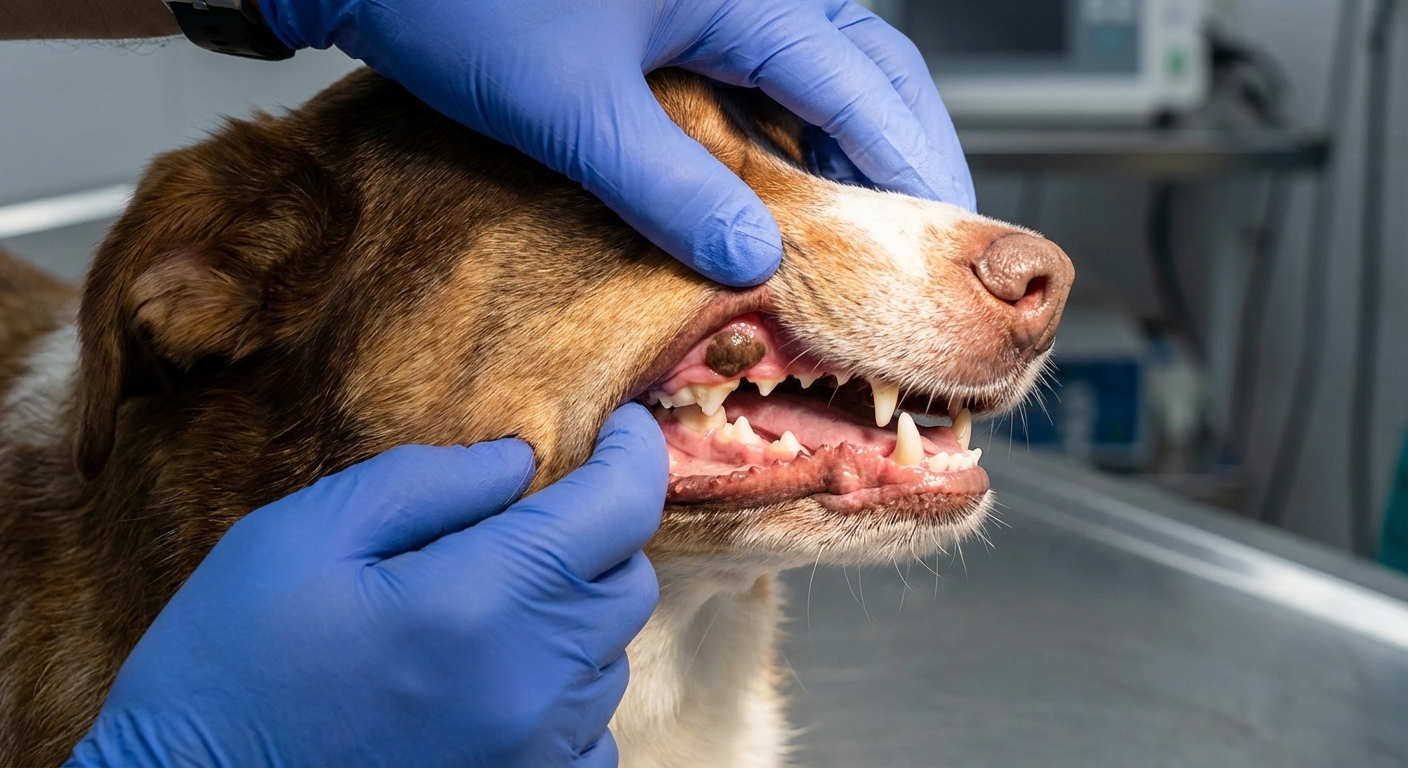
What is canine melanoma?
Melanoma is a cancer that starts in melanocytes, the cells that produce pigment (melanin). In dogs, melanomas can be pigmented (black or brown) or non-pigmented (pink or red, also called amelanotic). That matters because a pink mass can be mistaken for a benign growth or irritation.
In general, veterinarians group canine melanoma into three common types based on location:
- Oral melanoma: mouth, gums, lips, tongue, or hard palate
- Cutaneous melanoma: skin (anywhere on the body)
- Digital melanoma: toes and nail beds
Why oral melanoma is more aggressive
Location is not just about convenience. It is often associated with how the tumor behaves.
Oral environment and early spread
Oral melanomas tend to invade surrounding tissues early and can spread (metastasize) to nearby lymph nodes and the lungs. The mouth has a rich blood supply and lots of lymphatic drainage, which may help tumor cells travel sooner. Less commonly, melanoma can also spread to other organs (like the liver).
Different behavior on skin
Many haired-skin melanomas in dogs are benign or less aggressive, especially when they appear as small, slow-growing bumps. In contrast, oral melanomas are more likely to be malignant, locally invasive, and metastatic. Still, some skin locations (mucocutaneous junctions, footpads) and some biopsy findings can signal a higher-risk tumor even on the skin.
Harder to catch early
Dogs do not show obvious mouth symptoms at first. By the time owners notice bad breath, drooling, or bleeding, the tumor can already be advanced.
Oral melanoma (mouth)
What you might see at home can be surprisingly subtle at first:
- Bad breath that seems to come on quickly
- Bleeding from the mouth, or blood on chew toys
- Drooling, pawing at the mouth, or facial swelling
- Loose teeth not explained by dental disease alone
- Difficulty eating, dropping food, chewing on one side
- A dark or pink mass on the gums, lips, tongue, or palate
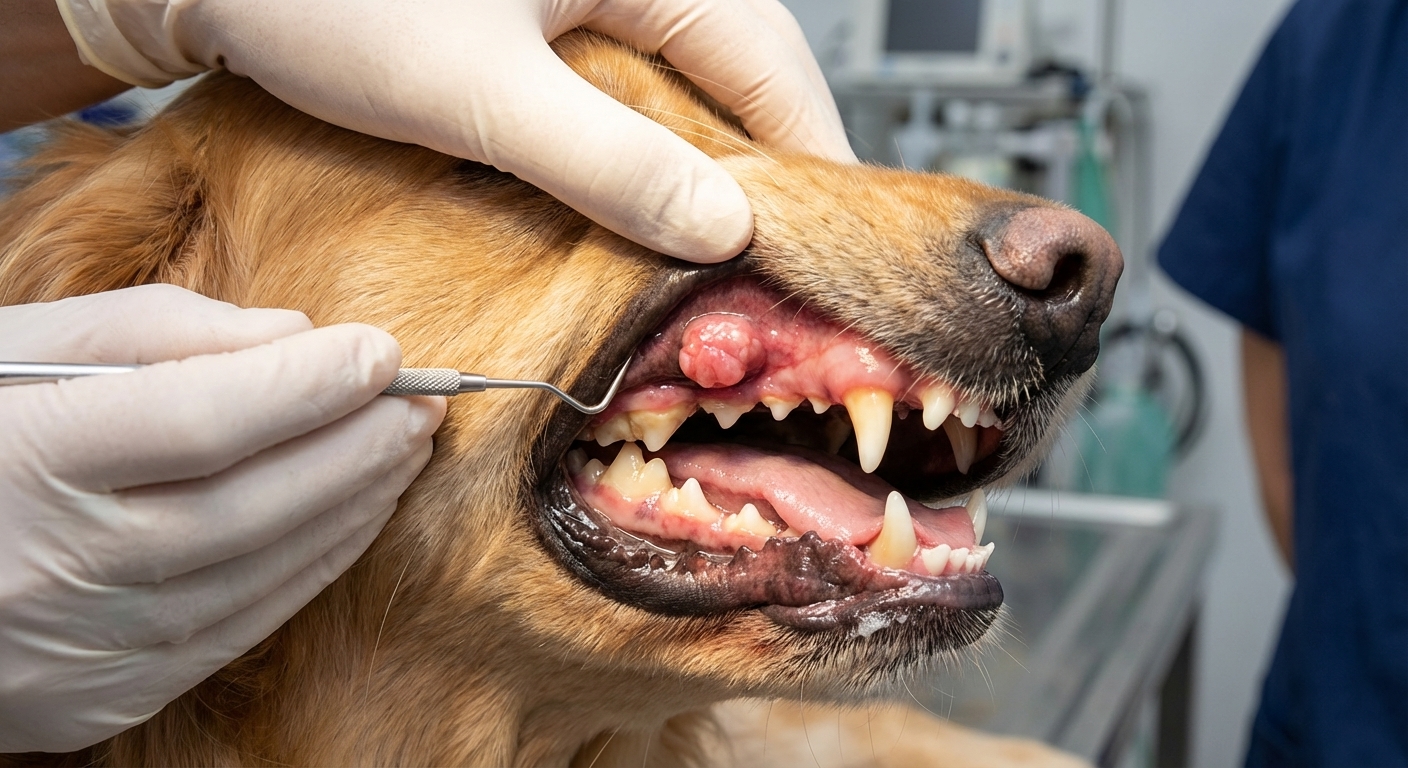
Important nuance: not every dark or pink oral mass is melanoma. Oral pigment can also come from benign growths (including melanocytomas) and other tumor types. That is why vets lean on sampling and biopsy for a real answer.
Prognosis: Oral melanoma is often considered aggressive. Prognosis varies widely depending on stage, whether the tumor can be removed completely, and whether there is metastasis.
Common spread sites: local lymph nodes (under the jaw and in the neck) and lungs.
Cutaneous melanoma (skin)
Skin melanomas can appear as:
- A raised dark bump
- A firm nodule under the skin
- A pink or red mass (amelanotic melanoma)
- A lesion that ulcerates or bleeds
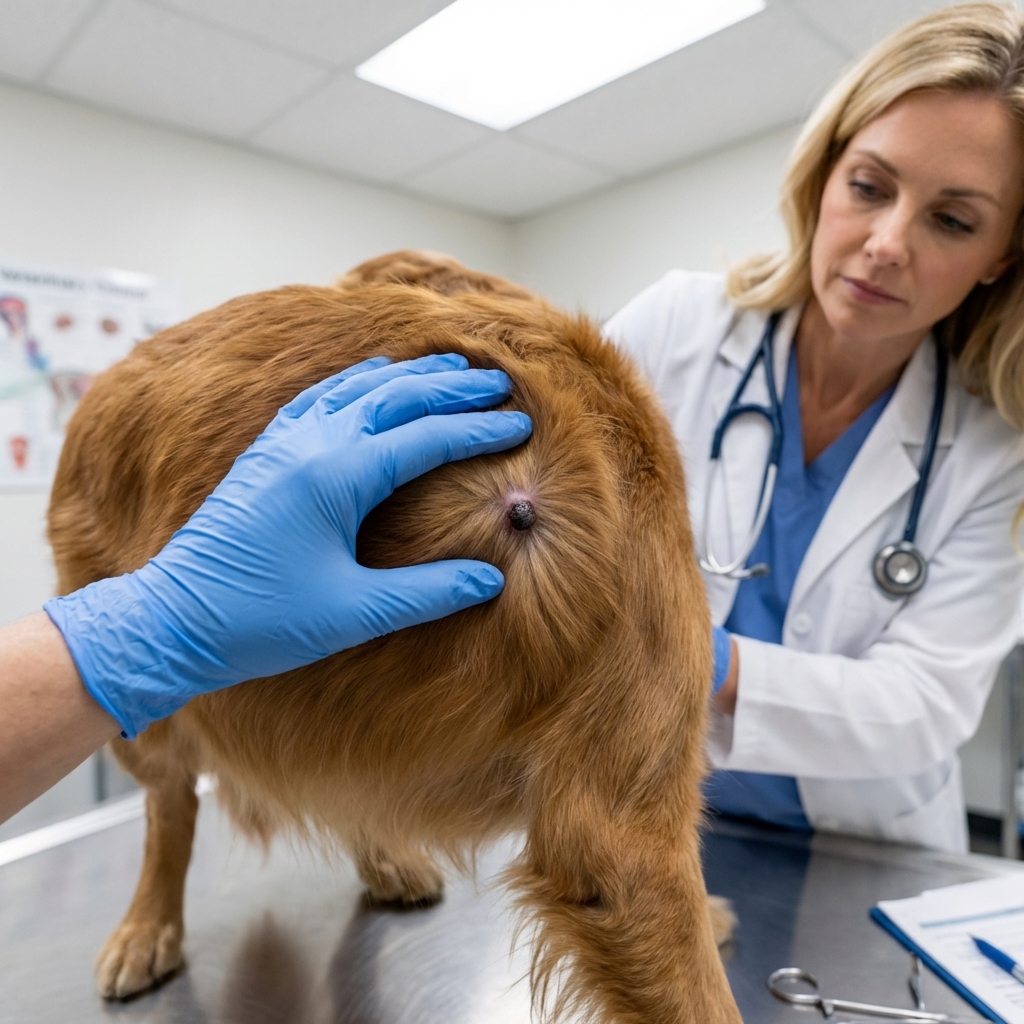
Prognosis: Many cutaneous melanomas on haired skin are benign, but not all. Melanomas on mucocutaneous junctions (like lip margins), on footpads, or those with concerning pathology features may act more aggressively. The only way to know what you are dealing with is diagnostic testing.
Key point: If a skin lump is changing, bleeding, itching, growing quickly, or looks unusual in any way, it is worth sampling.
Digital melanoma (toe and nail bed)
Nail bed melanoma is a big one for families to miss, because it often looks like an injury or infection.
Warning signs owners often notice first:
- A swollen toe or “puffy” nail bed
- A nail that breaks repeatedly or falls off
- Licking at one foot constantly
- Bleeding around the nail
- Lameness that comes and goes
- A draining sore that does not heal
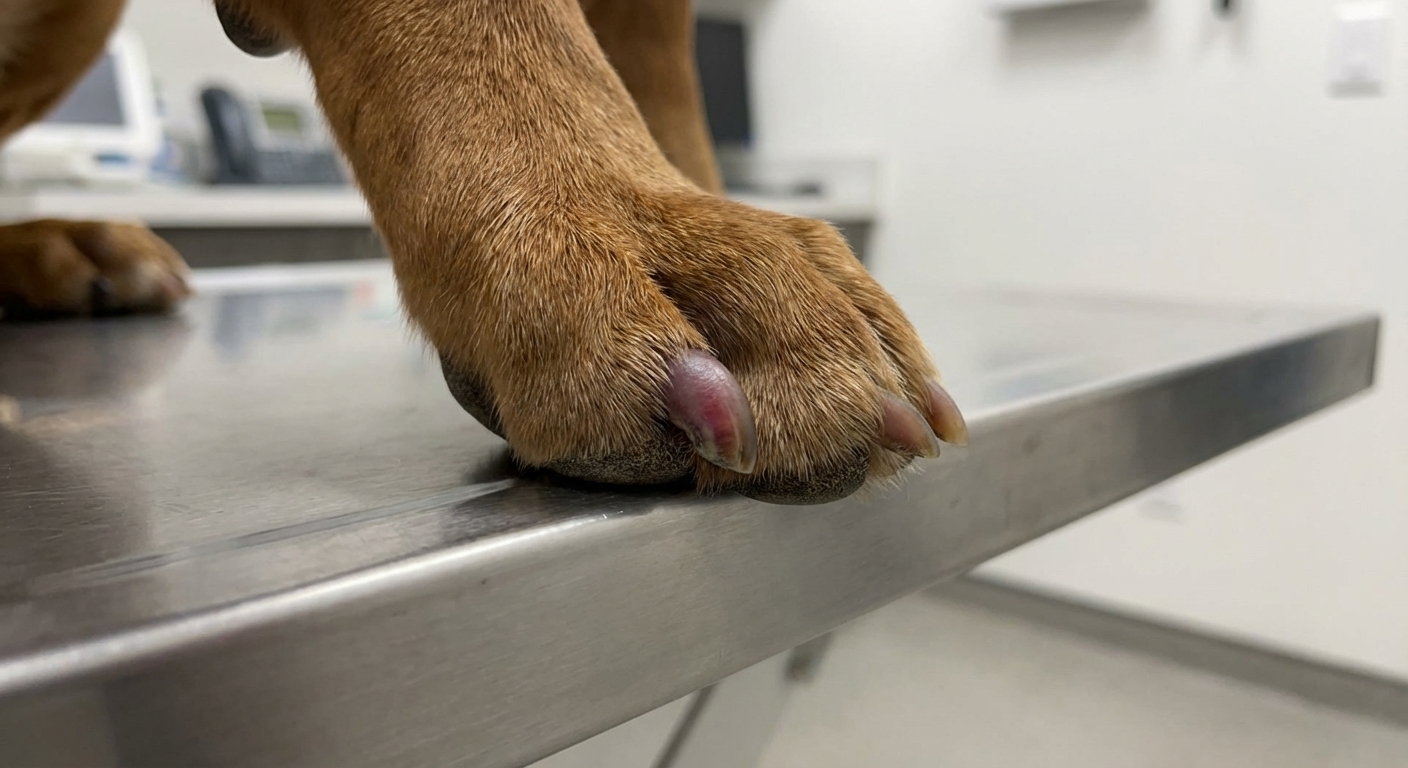
Important note: not every nail bed tumor is melanoma. Another common culprit is squamous cell carcinoma, and infections or trauma can mimic cancer too. Either way, a persistent nail bed problem deserves a vet visit and usually a sample.
Prognosis: Digital melanoma is often malignant and can metastasize, which is why vets tend to take toe tumors very seriously. Early diagnosis and treatment can make a meaningful difference.
How vets diagnose melanoma
If your vet suspects melanoma, you may hear about a few different steps. Not every dog needs every test, but these are common:
- Fine needle aspirate (FNA): a needle sample from the mass or a nearby lymph node
- Biopsy: a tissue sample to confirm the diagnosis and assess tumor features
- Oral exam under anesthesia: often needed for oral masses to see the full extent
- Imaging: chest X-rays or CT to look for spread to the lungs, and CT of the head for oral tumors to evaluate bone invasion
- Lymph node evaluation: sampling nodes can help staging even if they feel normal
Melanoma can be tricky on cytology (FNA) when it is non-pigmented. If the result is unclear, biopsy is usually the next step.
Staging: how advanced is it?
Staging helps guide treatment and prognosis. For oral melanoma in dogs, staging commonly considers:
- Tumor size (how large it is)
- Lymph node involvement (has it spread locally?)
- Distant metastasis (especially lungs)
You may hear your veterinarian or oncologist refer to stages such as:
- Stage I: smaller tumor, no evidence of spread
- Stage II: larger tumor, no evidence of spread
- Stage III: lymph node involvement (and often larger tumors)
- Stage IV: distant spread (often lungs)
About size cutoffs: systems vary, but a commonly used guide for oral melanoma is <2 cm (Stage I), 2 to 4 cm (Stage II), and >4 cm and or lymph node involvement (Stage III), with distant metastasis as Stage IV.
For cutaneous and digital melanoma, staging can vary more based on location and pathology findings, but the same big picture applies: size, local invasion, lymph nodes, and distant spread.
Treatment options
Treatment is usually about some combination of: removing the main tumor, controlling local disease, and reducing the risk of metastasis.
Surgery
Surgery is often the first choice when the tumor can be removed with clean margins.
- Oral melanoma: may require more extensive surgery than people expect, sometimes including partial jaw surgery. This can sound frightening, but many dogs recover well and return to eating comfortably.
- Digital melanoma: amputation of the affected toe is commonly recommended to get full removal and pain relief.
- Skin melanoma: removal of the mass with margins is often curative when the tumor is benign or low grade.
Radiation therapy
Radiation is often used for oral melanoma, especially when complete surgical removal is not possible. It can shrink tumors, improve comfort, and often provides good local control. On its own, it does not reliably prevent metastasis, so it is commonly part of a multi-step plan.
Immunotherapy (the melanoma vaccine)
You may hear about an immunotherapy vaccine for canine melanoma (often called the melanoma vaccine or Oncept), usually discussed after local control with surgery and/or radiation. The goal is to help the immune system recognize and attack melanoma cells.
Important note: study results are mixed and a clear survival benefit has not been consistent across all research. Availability also varies by region and practice. Many oncologists consider it most often for Stage II to Stage III cases after local control, but it is not universally recommended. This is a great “bring your questions” moment so you understand expected benefits, costs, and realistic goals for your dog.
Chemotherapy and newer therapies
Chemotherapy has historically had variable results with melanoma, but it may be considered in certain cases. Some dogs may also be candidates for newer approaches (including targeted or combination therapies) depending on what is available and the oncologist’s assessment.
Pain control and supportive care
Comfort matters. Dogs with oral tumors may have pain, trouble eating, or infections. Your vet may recommend a mix of pain medications, antibiotics if needed, appetite support, and dietary adjustments.
What to watch for at home
If you take only one thing from this article, let it be this: do not wait on mouth, toe, or nail changes. Melanoma and other aggressive tumors can move fast, and early action can open up more treatment options.
- Mouth: new bad breath, drooling, bleeding, swelling, a visible mass, trouble chewing
- Skin: a new lump, rapid growth, color change, ulceration, bleeding, persistent licking
- Nail bed/toe: swelling, recurring broken nail, persistent licking, bleeding, lameness, non-healing sore
If you see a suspicious growth, ask your vet about sampling it sooner rather than later. In veterinary medicine, we often say: “Do not watch lumps, sample lumps.”
What is urgent?
- Trouble breathing, open-mouth breathing, or significant facial swelling
- Profuse or persistent bleeding from the mouth
- Inability to eat or drink, or repeated gagging
- Severe pain that is not settling with prescribed meds
Questions to ask your vet
- Is this mass more likely benign or malignant based on location and appearance?
- Should we do an FNA, biopsy, or both?
- Do you recommend checking local lymph nodes even if they feel normal?
- What imaging do you recommend, and why (X-rays vs CT)?
- What is the goal of treatment for my dog: cure, control, or comfort?
- If surgery is recommended, what function changes should I expect afterward?
- Am I a candidate for radiation or the melanoma vaccine?
- What signs at home would be an emergency?
A hopeful note
A melanoma diagnosis is heavy, especially when it is in the mouth or nail bed. But you are not powerless here. Getting a fast, accurate diagnosis, staging the disease thoughtfully, and working with your veterinarian and a board-certified oncologist can help you choose the best plan for your dog and your family.
If you are unsure whether a spot is “serious enough,” please trust your instinct and schedule the visit. It is always okay to advocate for a sample and clear answers.
References
- Merck Veterinary Manual. Melanocytic Tumors (Dogs). (Accessed online.)
- American College of Veterinary Surgeons (ACVS). Melanoma (Canine). (Client education overview; accessed online.)
- Veterinary Cooperative Oncology Group (VCOG). Response Evaluation Criteria for Solid Tumors (RECIST) in dogs. (Guidance commonly used in oncology assessment; accessed via journal publication.)
- Published veterinary oncology reviews and clinical studies on oral melanoma staging (tumor size, lymph nodes, metastasis) and multimodal therapy, including radiation and immunotherapy vaccine outcomes. (Ask your oncologist which staging system and evidence base they use for your dog’s specific case.)
