Lymphoma in Cats: Stages, Prognosis, and What to Expect

If your cat has just been diagnosed with lymphoma, you are likely juggling a lot at once: scary new terms, a whirlwind of tests, and the big question everyone asks first, “How much time do we have?” As a veterinary assistant, I want you to know two things right away. First, feline lymphoma is common, and we have real treatment options. Second, the stage helps guide treatment planning, but it is not the only factor that affects prognosis.
In this guide, we will break down feline lymphoma staging (Stages I through V), how different lymphoma types behave (intestinal, mediastinal, nasal, renal, and more), and what you can do at home to support your cat through treatment.

What is lymphoma in cats?
Lymphoma is a cancer of lymphocytes, a type of white blood cell. Because lymphocytes travel throughout the body, lymphoma can show up in many places. Some forms are multicentric (in lymph nodes), and others are extranodal (in organs like the intestines, nose, kidneys, skin, or chest).
Many cats with lymphoma can feel “off” for weeks or months before a diagnosis. The most common signs include:
- Weight loss
- Decreased appetite or picky eating
- Vomiting or diarrhea (especially with intestinal lymphoma)
- Lethargy and hiding
- Increased thirst and urination (often with kidney involvement)
- Breathing changes (especially with mediastinal lymphoma)
Important: These signs also happen with many non-cancer conditions. That is why diagnostics and staging matter.
Why staging matters
Staging is the process of mapping where the cancer is in the body. In cats, staging helps your veterinary team:
- Choose the most appropriate treatment approach (chemotherapy, surgery, steroids, radiation, or combinations)
- Estimate prognosis and likely response
- Set a baseline so you can track response to treatment
- Identify organ involvement that changes safety or dosing for medications
That said, two cats with the same stage can have very different outcomes depending on factors like lymphoma type (small-cell versus large-cell), exact location, overall health, and how well the cancer responds to therapy.
Common staging tests
Your vet or veterinary oncologist may recommend some combination of the following:
- Physical exam and lymph node palpation
- Bloodwork: CBC, chemistry panel, and sometimes FeLV and FIV testing
- Urinalysis: especially important when kidney involvement is suspected
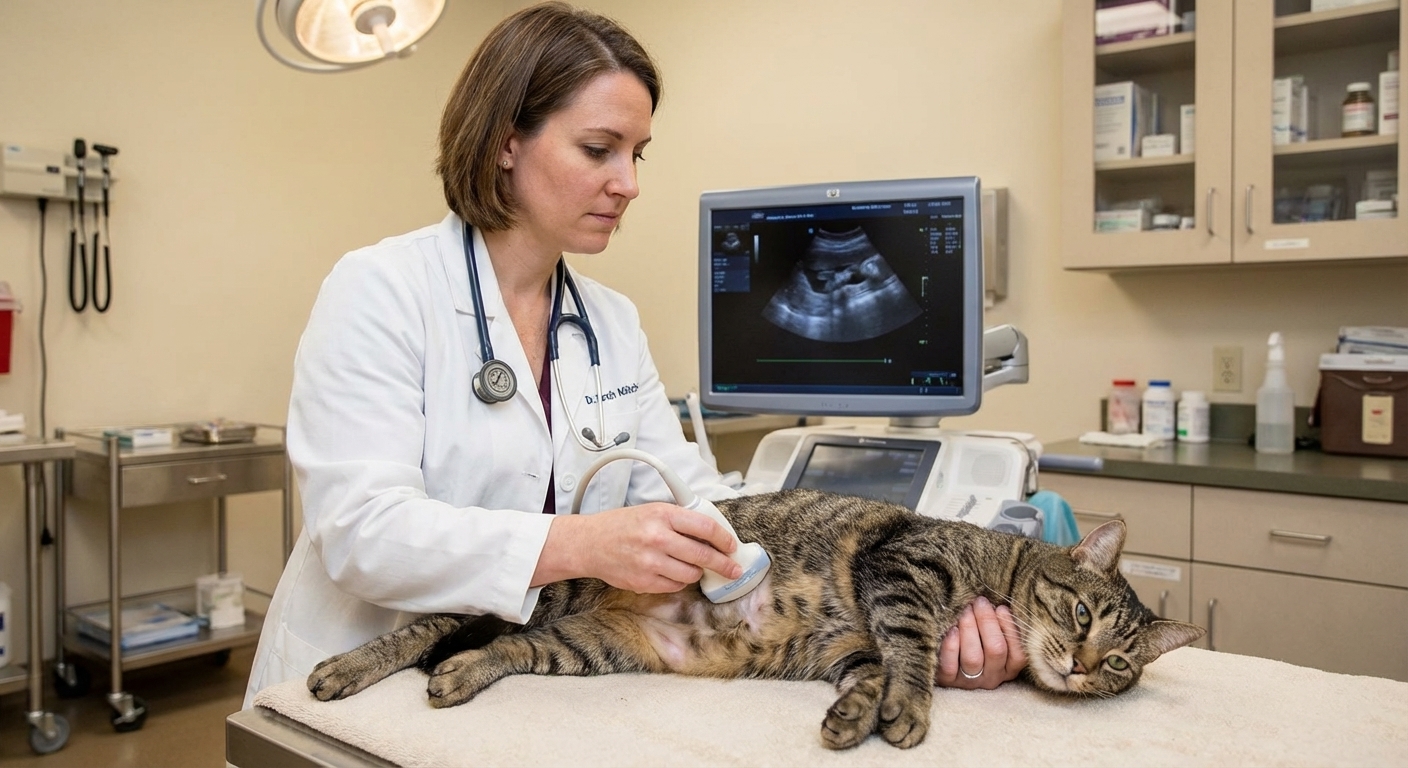
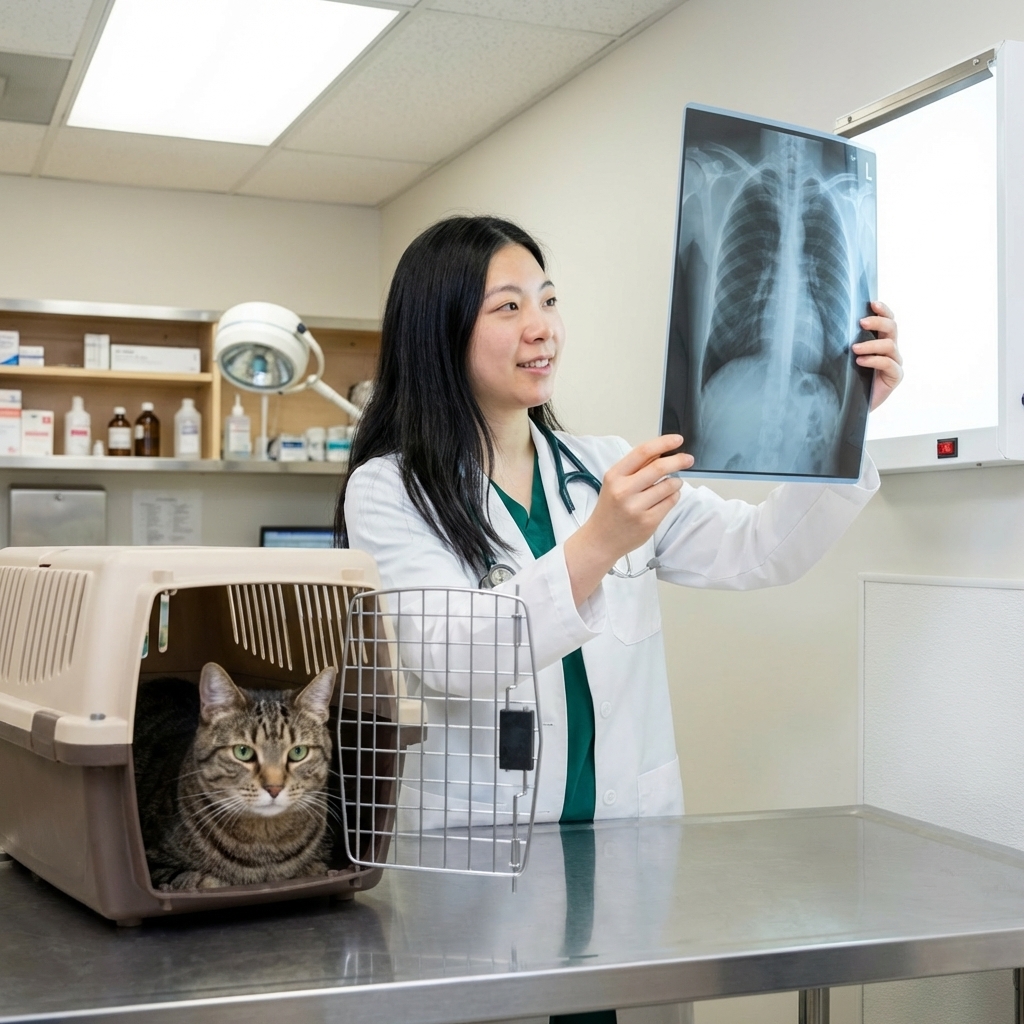
- Imaging: chest radiographs, abdominal ultrasound, sometimes CT
- Cytology or biopsy: aspirate of a lymph node or mass, intestinal biopsies (endoscopic or surgical) if needed
- Flow cytometry or PARR testing: specialized tests that can help confirm lymphoma, identify lineage, and support subtyping in certain cases
Stages and substages
Veterinarians often use a stage system adapted from the World Health Organization (WHO) approach for lymphoma. You may also hear about a “substage,” which describes how your cat feels overall:
- Substage a: feels relatively well, no obvious systemic illness
- Substage b: has systemic signs such as fever, significant weight loss, marked lethargy, or a noticeable drop in appetite
Substage matters. Cats that are bright and eating generally tolerate treatment better.
Stage I
What it means: Lymphoma is in a single location, typically one lymph node, one organ, or one localized extranodal mass.
What it can look like:
- A single enlarged lymph node (for example, under the jaw)
- A solitary nasal mass causing sneezing or one-sided discharge
- A single intestinal mass segment
Treatment options: Depending on location and type, this may include chemotherapy, localized radiation (commonly for nasal cases), or surgery to remove a solitary mass followed by chemotherapy.
Prognosis notes: Localized disease can sometimes have a better outlook, but lymphoma can be microscopic elsewhere even when it appears localized. Your oncologist will focus on control and quality of life.
Stage II
What it means: Multiple lymph nodes are affected in one general region of the body, or a single organ tumor with involvement of nearby lymph nodes.
What it can look like:
- Several enlarged lymph nodes in the head and neck region
- An intestinal tumor with local abdominal lymph node involvement
Treatment options: Chemotherapy is typically recommended. In selected cases, surgery may be part of the plan (especially for obstructive intestinal masses), but lymphoma is usually treated as a whole-body disease.
Prognosis notes: Many cats can still do well, especially if they feel good overall and the lymphoma is a slower-growing subtype.
Stage III
What it means: Lymphoma is generalized in lymph nodes throughout the body.
What it can look like:
- Enlarged lymph nodes in multiple areas (neck, shoulders, popliteal nodes behind the knees)
- Weight loss, reduced appetite, lower energy
Treatment options: Multi-agent chemotherapy protocols are commonly recommended. Steroids may be used as part of therapy or palliative care, but timing matters (more on that below).
Prognosis notes: Stage III is considered widespread, but response to treatment is still one of the biggest drivers of outcome.
Stage IV
What it means: The liver and or spleen are involved, often along with stage III lymph node disease.
What it can look like:
- Enlarged liver or spleen on ultrasound
- Changes in liver enzymes on bloodwork
- Abdominal distension in some cases
Treatment options: Chemotherapy is usually the primary treatment. Supportive medications to protect appetite, reduce nausea, and support hydration can make a big difference.
Prognosis notes: Organ involvement can complicate care, but many cats still achieve good quality-of-life time if the lymphoma responds.
Stage V
What it means: Lymphoma involves the blood and or bone marrow, and or the central nervous system. Depending on the reference and the clinical situation, stage V may also be used when there is widely disseminated extranodal organ involvement (for example, extensive kidney involvement alongside other systemic sites).
How extranodal sites fit in: Extranodal lymphoma can occur at several stages. A solitary extranodal lesion (such as a localized nasal mass) is often staged as localized disease, while widespread organ involvement is staged higher.
What it can look like:
- Abnormal blood cell counts (anemia, low white cells, low platelets) from bone marrow involvement
- Neurologic signs such as weakness, seizures, or behavior changes if CNS is involved
- Severe lethargy, decreased appetite, and overall decline
Treatment options: Chemotherapy may still be offered, but plans are individualized based on organ function and comfort. Palliative care is a valid, compassionate path when treatment would not be tolerated or would not help.
Prognosis notes: Stage V typically carries a more guarded prognosis, but some cats respond surprisingly well. Your oncology team will help you weigh potential benefits versus stress.
Types by location
Location is a big part of what makes feline lymphoma feel so different from one cat to another. Below are the most common patterns and what they often mean in real life.
Intestinal lymphoma
Where it occurs: stomach, small intestine, large intestine, and associated abdominal lymph nodes.
Common signs:
- Chronic vomiting or diarrhea
- Weight loss and muscle wasting
- Reduced appetite or food aversion
- Sometimes constipation if the colon is involved
Small-cell vs large-cell:
- Small-cell intestinal lymphoma is often slower-growing. Many cats do well for long periods with oral chemotherapy (commonly chlorambucil) plus prednisolone, along with B12 support if needed.
- Large-cell intestinal lymphoma is more aggressive and often treated with multi-agent injectable chemotherapy. Prognosis is usually more guarded than small-cell, but remission is possible.
What staging looks like here: Staging evaluates intestinal involvement, regional lymph nodes, and spread to organs such as the liver and spleen, and sometimes kidneys or bone marrow.

GI diagnosis can be tricky
One common frustration for families is the overlap between inflammatory bowel disease (IBD) and small-cell intestinal lymphoma. Ultrasound can suggest patterns, but it cannot always definitively separate IBD from lymphoma.
If the diagnosis feels uncertain, your veterinarian may discuss:
- Endoscopic biopsies versus full-thickness surgical biopsies
- Whether sampling lymph nodes (and not only the intestine) would improve clarity
- Specialized testing such as PARR, which can help support a lymphoma diagnosis in some cases, especially when standard biopsy results are borderline
If you feel stuck, asking “What diagnosis are we most confident in, and what test would change the plan?” can be a helpful way forward.
Mediastinal lymphoma
Where it occurs: the mediastinum, which is the area in the chest between the lungs. This can involve the thymus and nearby lymph nodes.
Common signs:
- Rapid or labored breathing
- Open-mouth breathing or panting
- Reduced activity, hiding
- Sometimes loss of appetite due to discomfort
Why it can feel urgent: A mass or fluid in the chest can affect breathing. Cats with respiratory distress should be treated as an emergency.
FeLV connection: Historically, mediastinal lymphoma has been associated with feline leukemia virus (FeLV), especially in younger cats, although it can occur in FeLV-negative cats as well. Testing status helps guide the conversation about prognosis and overall health planning.
Treatment options: Chemotherapy is the mainstay. If there is pleural effusion (fluid around the lungs), your vet may recommend thoracocentesis (draining the fluid) to help your cat breathe before additional treatment starts.
Nasal lymphoma
Where it occurs: the nasal passages and surrounding tissues. This is a relatively common extranodal form in cats.
Common signs:
- Sneezing and noisy breathing
- One-sided nasal discharge (sometimes bloody)
- Facial discomfort or pawing at the nose
What makes it unique: Nasal lymphoma is often discussed separately because it can respond very well to localized radiation therapy, especially when it is truly confined to the nasal area. Chemotherapy may still be part of the plan depending on staging and subtype.
Staging focus: Imaging of the nose and head (often CT), checking nearby lymph nodes, and screening for spread elsewhere.
Renal lymphoma
Where it occurs: one or both kidneys, sometimes with spread to nearby lymph nodes, liver, spleen, or brain and spinal cord.
Common signs:
- Increased thirst and urination
- Weight loss, poor appetite
- Vomiting and dehydration
- Kidney pain or discomfort in some cats
Why kidney lymphoma is unique: Kidney involvement can affect how safely we can use certain medications and can change supportive care needs. An increased risk of central nervous system spread has been reported in some cats, so your oncologist may watch closely for neurologic changes.
Treatment options: Chemotherapy plus strong supportive care. In some cats, managing kidney values, hydration, nausea, and appetite becomes just as important as treating the cancer itself.
Subtype matters
You may hear your oncology team talk about grade (small-cell versus large-cell) and immunophenotype (B-cell versus T-cell). This is not just academic.
- Grade often predicts how fast the lymphoma grows and which chemotherapy approach is most effective.
- Immunophenotype can help refine prognosis and guide expectations, since some patterns behave differently depending on B-cell versus T-cell origin.
Prognosis and life expectancy
I wish there were one simple number I could give you. The truth is that prognosis in feline lymphoma depends on a combination of:
- Lymphoma grade and type (small-cell versus large-cell is often more predictive than stage alone)
- Location (intestinal, mediastinal, renal, nasal, etc.)
- Substage (how sick your cat feels)
- Response to treatment (remission duration varies widely)
- Underlying viruses (FeLV status in some cases)
- Organ function (especially kidneys and liver)
General patterns you may hear from your oncology team:
- Many small-cell intestinal lymphoma cats can do well for extended periods with oral therapy and careful monitoring.
- Large-cell lymphoma often needs more intensive chemotherapy. Some cats achieve remission, but relapse is more common and can happen sooner.
- Mediastinal and renal cases can be more complex because of breathing or kidney function issues, but supportive care can meaningfully improve comfort and outcomes.
- Nasal lymphoma can have a particularly encouraging response when localized radiation is an option and staging supports a confined disease process.
Your veterinarian or oncologist can give you the most realistic expectation after staging, subtype confirmation, and the first few weeks of treatment response.
Treatment by stage
Here is the big-picture idea many oncology teams follow. Exact protocols vary and should always be individualized by your veterinarian or veterinary oncologist based on your cat’s subtype, organ function, and comfort.
Stages I to II
- Chemotherapy is commonly recommended, even if the disease appears localized.
- Surgery may be used if a mass is obstructing the intestine or if there is a solitary, accessible tumor.
- Radiation is sometimes used for certain localized forms (for example, some nasal lymphomas).
Stage III
- Multi-agent chemotherapy is common.
- Supportive medications for appetite and nausea are frequently added early.
Stages IV to V
- Chemotherapy can still be helpful, but organ function and comfort guide decisions.
- More frequent monitoring is often needed (bloodwork, urinalysis, rechecks).
- Palliative care may be chosen sooner if quality of life cannot be protected.
A note about steroids: Prednisolone is often part of lymphoma care, but do not start it at home without veterinary guidance. If steroids are started before cytology or biopsy sampling, they can temporarily shrink lymphoma and reduce diagnostic yield. In some cases, starting prednisolone before chemotherapy may also reduce the chance of a strong chemotherapy response later. If you already started steroids, tell your vet, since it affects next steps.
How to support your cat
This is the part that tends to make the biggest day-to-day difference for families. Treatment is not only about chemotherapy. It is also about keeping your cat comfortable, eating, hydrated, and calm.
At-home care that helps
- Track appetite and weight weekly. A baby scale can be very helpful for small cats.
- Use nausea control early. If your cat is nauseated, they may act “picky” when they are actually queasy. Ask your vet about anti-nausea meds if vomiting, lip smacking, drooling, or food avoidance show up.
- Hydration support. Add water to food, offer a fountain, and ask about subcutaneous fluids if kidney values are a concern.
- Keep stress low. A quiet recovery area, familiar bedding, and predictable routines help. Many cats do better with separate feeding spaces away from other pets.
- Litter box monitoring. Note stool consistency and frequency. Report straining, black stools, or blood.
Feeding tips
Nutrition matters because lymphoma and treatment can reduce appetite and cause weight and muscle loss. Practical strategies:
- Warm wet food slightly to enhance aroma.
- Offer smaller meals more frequently.
- Ask your vet about appetite stimulants if intake drops.
- If your cat has intestinal lymphoma, follow your vet’s guidance on diet trials, novel proteins, or hydrolyzed diets if food sensitivity is suspected.
Chemotherapy safety at home
If your cat is receiving chemotherapy, your veterinary team will give you specific handling instructions. General precautions often include:
- Wash hands after giving oral meds.
- Use gloves if instructed, especially for chemotherapy tablets.
- Be extra careful with litter box waste for a period after treatments, as drugs can be present in urine and feces.

Quality of life check
It is normal to wonder, “How will I know if my cat is doing okay?” A simple weekly check-in can help you catch problems early and also feel more confident about decisions.
- Eating: Are they eating enough to maintain weight?
- Comfort: Are they resting comfortably, grooming some, and moving without obvious pain?
- Energy: Are they still seeking favorite spots and responding to you?
- Breathing: Is breathing calm and easy at rest?
- Bathroom: Are urine and stools happening regularly and without straining?
If more “no” answers are stacking up week to week, it is a kind and responsible choice to ask your veterinary team about adjusting the plan, adding hospice support, or discussing euthanasia timing. Those conversations can be part of good care, not a failure.
What to expect at rechecks
Most cats in active treatment have regular rechecks. What your vet monitors commonly includes:
- Body weight, muscle condition, hydration
- Bloodwork to watch white blood cells, red blood cells, platelets, kidney and liver values
- Response of lymph nodes or masses on exam
- Repeat ultrasound or chest radiographs when needed
Side effects are possible, but cats often tolerate chemotherapy better than people expect. Many protocols are designed with quality of life as the priority.
When to call urgently
Contact your veterinarian or an emergency clinic right away if you notice:
- Open-mouth breathing, severe panting, or breathing effort
- Repeated vomiting or inability to keep water down
- Profound lethargy or collapse
- No appetite for more than 24 hours, especially in cats prone to hepatic lipidosis
- Not urinating, straining, or signs of pain
- Bleeding, bruising, or very pale gums
Questions to ask
- What type of lymphoma is this (small-cell vs large-cell, B-cell vs T-cell if known)?
- What stage and substage is my cat, and what does that change in the plan?
- What is the goal: remission, control, or comfort?
- What side effects should I watch for at home and when should I call?
- How often will rechecks and bloodwork be needed?
- What costs should I expect over the first 4 to 8 weeks?
- If treatment stops working, what are the next best options?
The bottom line
Lymphoma in cats is not one single disease. Stage helps your veterinary team understand how far it has spread, but location and lymphoma subtype often explain even more about what to expect. With the right plan, many cats maintain a good quality of life during treatment, and supportive care at home can be just as powerful as the medications themselves.
If you are in the early days of diagnosis, take it one step at a time. Ask for the staging plan in writing, keep a simple daily log of appetite and energy, and lean on your veterinary team. You do not have to carry this alone.
References
- Vail DM, Thamm DH, Liptak JM. Withrow and MacEwen’s Small Animal Clinical Oncology. (Lymphoma chapters, clinical staging concepts, and treatment principles.)
- Merck Veterinary Manual. Lymphoma in cats (overview of presentation, diagnostics, and treatment principles).
- Veterinary partner resources from specialty hospitals and oncology services that outline feline lymphoma staging workups, chemotherapy monitoring, and home safety precautions.
- Peer-reviewed review literature on feline alimentary lymphoma and chlorambucil plus prednisolone protocols (consult your oncologist for the most relevant, up-to-date citations for your cat’s specific subtype).
