Ringworm spreads fast, but it’s treatable. Learn how vets diagnose it, which shampoos, dips, and oral meds help, and how to clean your home to prevent rein...
Article
•
Designer Mixes
How to Tell if Your Dog Has Ringworm

Shari Shidate
Designer Mixes contributor
Ringworm can sound scary, but here is the comforting truth: it is treatable, and the sooner you recognize it, the easier it is to get your dog feeling comfortable again. As a veterinary assistant, I also want you to know one key fact up front: ringworm is not a worm at all. It is a fungal infection of the skin, hair, and sometimes nails.
Because it can spread to other pets and to people, knowing what to look for and what to do next matters. Many skin issues look alike, so getting the right diagnosis helps you treat the right problem and avoid wasting time on products that can make things worse.
This guide will walk you through the signs, what ringworm can look like on different coats and skin tones, how vets diagnose it, and how to protect your home while your dog heals.
What ringworm is and how dogs catch it
Ringworm is caused by dermatophyte fungi. In dogs and cats, the most common species include Microsporum canis, Microsporum gypseum, and Trichophyton mentagrophytes. These fungi produce spores that can live in the environment, especially in places with hair and dust (bedding, carpets, grooming tools, crate pads).
Common ways dogs are exposed
- Direct contact with an infected animal (dog, cat, rabbit, or even wildlife).
- Contact with spores in the environment (shared bedding, grooming clippers, collars, floors).
- Higher-risk settings like shelters, grooming facilities, boarding, and daycare. Dog parks can be a risk too, especially if there are infected animals or contaminated shared surfaces.
Dogs most at risk
- Puppies and seniors
- Dogs with allergies or irritated skin
- Dogs with weakened immune systems
- Dogs living in crowded environments
- Long-coated dogs where early lesions are harder to notice
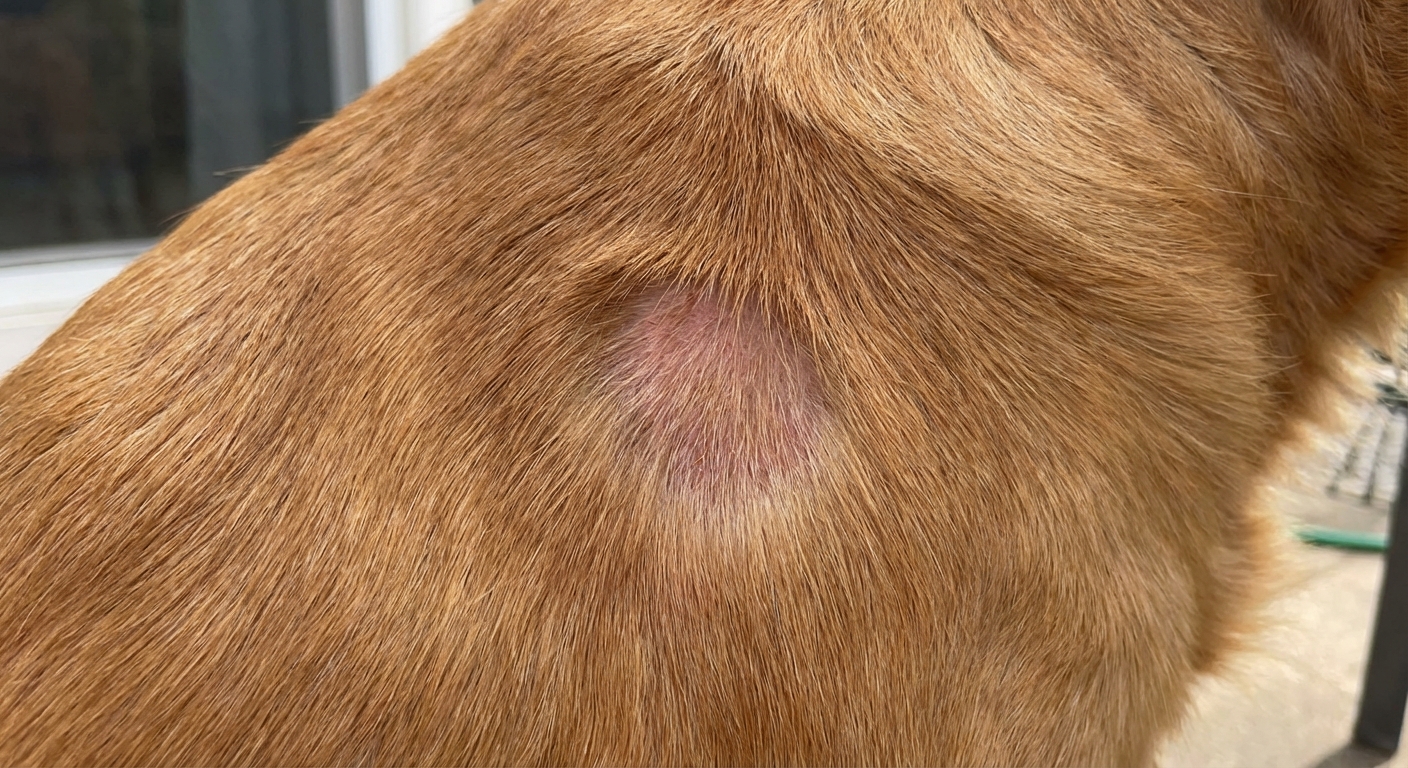
Signs your dog may have ringworm
Ringworm is famous for a “ring” shape, but in real life it can be subtle or look like many other skin conditions. You may see one lesion or multiple patches, and some dogs itch while others do not.
Most common symptoms
- Circular hair loss (often with a scaly edge)
- Broken hairs or “stubbly” hair in a patch
- Flaky, crusty skin (dandruff-like scaling)
- Redness or mild inflammation
- Itching (sometimes mild, sometimes more noticeable)
- Darkened skin or changes in pigmentation as it heals
- Nail involvement (less common): brittle, rough, or misshapen nails
Lesions are commonly found on the face, ears, paws, and forelimbs, but they can occur anywhere.

What it looks like on different dogs
Ringworm does not present the same way on every dog. Coat type, grooming, skin tone, and underlying allergies can change the look dramatically.
Short-haired dogs
You may notice clean, round patches of hair loss quickly. Scaling at the edges is common.
Long-haired or curly-coated dogs
Patches can be hidden. Sometimes you see breakage or a “moth-eaten” look rather than a perfect circle.
Light skin vs. dark skin
On lighter skin, redness can be obvious. On darker skin, you may see more grayish scaling, hyperpigmentation (darkening), or a subtle change in coat density.
Dogs with allergies
If your dog already struggles with itchy skin, ringworm can blend in with allergy flares. In these cases, diagnosis is especially important before you assume it is “just allergies again.”
Ringworm or something else?
Many conditions mimic ringworm. That is why I always encourage pet parents not to self-diagnose based on photos alone.
- Hot spots (moist, painful, often very itchy)
- Mange (Demodex or Sarcoptes mites)
- Allergies (food or environmental)
- Bacterial folliculitis (pimples, crusts, patchy hair loss)
- Yeast dermatitis (often greasy, smelly, itchy)
- Pressure sores (on elbows and bony areas)
- Ring-like lesions from immune conditions (less common, but important)
If you see circular hair loss, do not panic. Just treat it as “possibly contagious” until your veterinarian confirms what it is.
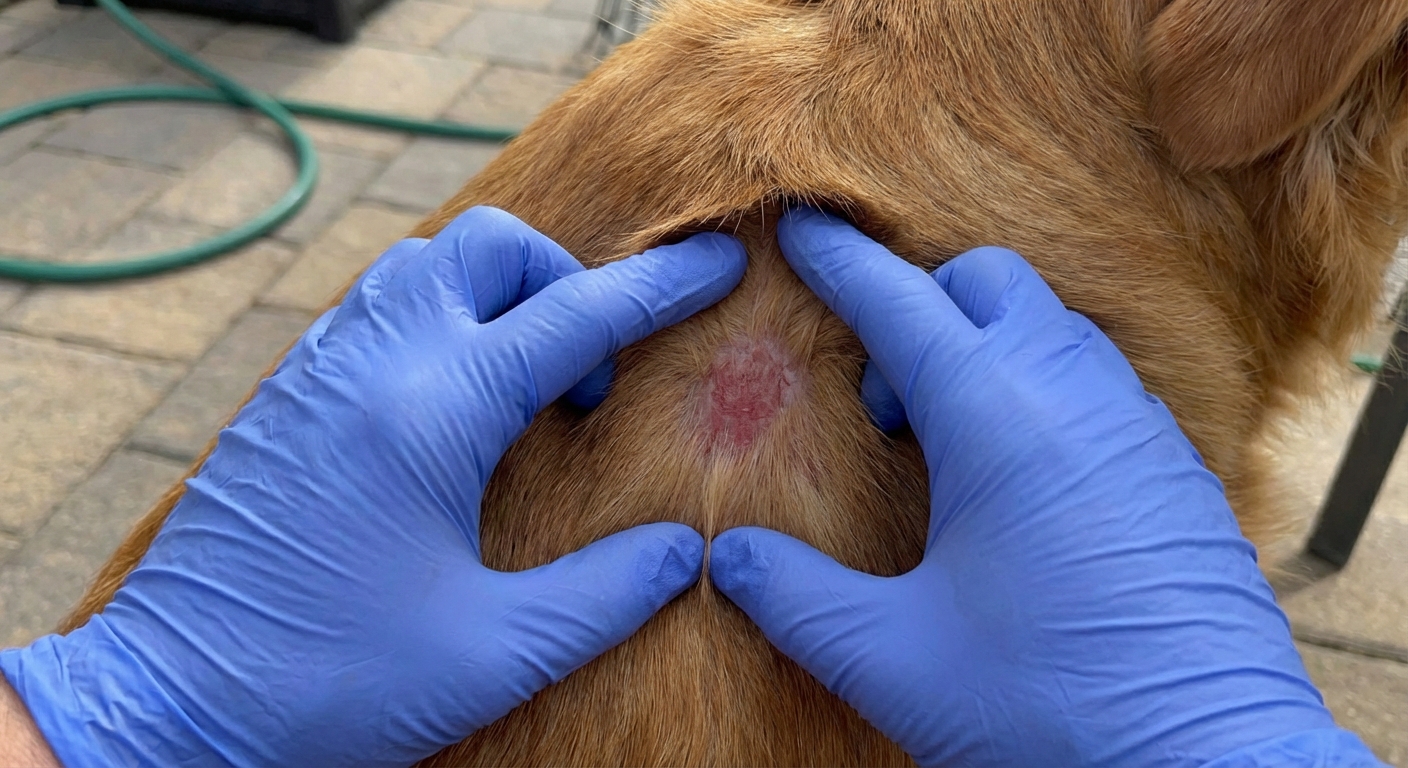
How vets diagnose ringworm
Because ringworm can imitate other skin problems, your veterinarian will usually combine history, exam findings, and targeted testing.
1) Wood’s lamp exam
Some ringworm species fluoresce an apple-green color under a Wood’s lamp. Microsporum canis is the classic one that may glow, while other species often do not. This is quick and helpful, but it is not perfect. Many true ringworm cases do not glow, and some debris can create false positives.
2) Microscopic exam (trichogram)
Your vet may examine plucked hairs or skin debris to look for fungal elements. This can provide quick clues but may miss early or mild infections.
3) Fungal culture
A culture can confirm ringworm and identify the organism. This test takes time because fungi grow slowly, but it is one of the most reliable options.
4) PCR testing
Some clinics use PCR for faster detection of fungal DNA. It can be a great tool, especially when timing matters, though your veterinarian will interpret results in the context of symptoms and exposure.
Is it contagious?
Yes. Ringworm is zoonotic, meaning it can spread between animals and people. Cats are especially common carriers, and some pets can carry spores with minimal symptoms.
People at higher risk
- Children
- Older adults
- Anyone immunocompromised
- Anyone with frequent close contact (cuddling, sleeping with pets, grooming)
If anyone in the household develops an itchy, circular rash, contact your human healthcare provider and mention a possible ringworm exposure.
What to do if you suspect it
The goal is to protect your dog, protect your household, and get a clear diagnosis.
Step-by-step
- Call your veterinarian and ask for guidance on skin testing and next available appointment.
- Limit contact between the suspected pet and other pets until you know what you are dealing with.
- Pause grooming appointments and avoid daycare, boarding, and other close-contact settings for now.
- Wash hands after handling your dog and avoid letting them sleep on pillows or shared bedding until you have a plan.
- Do not apply random creams (especially steroid creams) unless your vet instructs you. Topical or oral steroids can mask or worsen fungal infections and can delay the correct diagnosis.
Treatment overview
Treatment depends on how widespread the infection is, your dog’s coat type, whether other pets are exposed, and your veterinarian’s diagnostic results. Many cases require a combination approach.
Common treatment tools
- Topical therapy: medicated shampoos or rinses to reduce spores on the coat
- Oral antifungal medication: often used for more extensive disease or in multi-pet households
- Clipping: sometimes recommended for long-coated dogs to improve topical contact and reduce contaminated hair
- Environmental cleaning: critical, because spores can re-infect pets
How long it usually takes
Many dogs need several weeks of treatment. A common range is about 4 to 8 weeks, but it can be shorter or longer depending on the case and how well environmental control is going. Your veterinarian may recommend follow-up testing to confirm your dog is truly clear, especially if there are other pets in the home.
What not to do
- Do not stop treatment early just because the skin looks better. Spores can linger.
- Do not use essential oils or home remedies. Some are toxic to pets, and many do not treat the infection.
- Do not rehome out of fear. With a plan, ringworm is very manageable.
Home cleaning and prevention
Ringworm spores are hardy. Medication helps your dog, but cleaning helps stop the cycle. This is where many households struggle, and it is also where you can make the biggest difference.
Practical cleaning checklist
- Vacuum frequently, ideally daily in high-traffic areas. Focus on rugs, couch cushions, and baseboards. Dispose of vacuum contents promptly.
- Wash bedding (pet and human) in hot water and dry on high heat when fabric allows.
- Hard surfaces: clean first, then disinfect. Follow label directions for dilution and contact time, and keep pets away until surfaces are dry.
- Disinfectants your vet may suggest: accelerated hydrogen peroxide products or a properly diluted bleach solution, used carefully and according to instructions. Ask your veterinarian what is safest for your home and surfaces.
- Grooming tools: disinfect brushes, combs, collars, harnesses, and clippers.
- Create a “clean zone”: confine your dog to one easy-to-clean room when possible. If you can, limit access to carpeted rooms and soft furnishings during treatment.
If you have multiple pets, ask your veterinarian whether they should be checked or treated too. Quiet carriers happen, and cats are a common example.
When to seek urgent care
Ringworm itself is rarely an emergency, but some situations should be addressed quickly:
- Rapidly spreading lesions or severe inflammation
- Signs of secondary infection (oozing, strong odor, pain, swelling)
- Facial swelling, significant discomfort, or your dog seems unwell
- Immunocompromised dog (for example, on certain medications or with chronic disease)
FAQ
Can ringworm go away on its own?
Sometimes mild cases can improve over time, but that is not a safe plan in most homes because ringworm is contagious and spores persist in the environment. Treatment also reduces spread and discomfort.
How long is a dog with ringworm contagious?
It varies. Dogs can shed spores while lesions are active and sometimes beyond what you can see. Your veterinarian may recommend rechecks or tests to confirm resolution.
Does ringworm always itch?
No. Some dogs are surprisingly unbothered, which is why you might only notice a patch of hair loss at first.
Can I catch ringworm from my dog?
Yes. Good hygiene, limiting close contact until diagnosis, and environmental cleaning make a huge difference.
A gentle closing note
If you suspect ringworm, you are already doing the most important thing: paying attention. Take a photo of the lesion (so you can track changes), schedule a vet visit, and start simple containment and cleaning. With the right diagnosis and a consistent treatment plan, most dogs recover very well, and families can get back to normal cuddles safely.




