Splenic masses in dogs can be silent until they bleed. Learn subtle warning signs, rupture emergencies, how vets diagnose, what to expect at the ER, treatmen...
Article
•
Designer Mixes
Hemangiosarcoma in Dogs: Symptoms, Stages, and What to Expect

Shari Shidate
Designer Mixes contributor
Hemangiosarcoma is one of the most heartbreaking cancers we see in dogs because it often grows silently and is discovered during an emergency. As a veterinary assistant, I have watched families go from “He was fine yesterday” to facing big decisions in a single afternoon. The good news is that understanding the early warning signs, the diagnostic process, and what treatment can realistically do helps you act faster and feel more grounded, even in a scary moment.
This article covers the most common types of hemangiosarcoma (splenic, cardiac, dermal, and liver), symptoms owners often miss, how vets diagnose and stage it, treatment options (including surgery and chemotherapy), prognosis by stage, and quality of life considerations. I will also clearly outline emergency signs of a splenic rupture and what typically happens at the ER, because those minutes matter.

What is hemangiosarcoma?
Hemangiosarcoma (often shortened to HSA) is an aggressive cancer that starts in cells that line blood vessels. Because it is a “blood vessel tumor,” it tends to form fragile, blood-filled masses that can bleed internally. It can also spread (metastasize) early, often before a dog shows obvious symptoms.
Hemangiosarcoma can develop in multiple areas of the body, but there are a few types owners hear about most:
- Splenic hemangiosarcoma: One of the most common visceral (internal) forms. A mass forms on the spleen and may rupture, causing internal bleeding.
- Cardiac hemangiosarcoma: Often arises on the right side of the heart (commonly the right atrium) and can cause fluid or blood to accumulate around the heart.
- Hepatic (liver) hemangiosarcoma: Another common visceral site. Liver masses can also bleed, sometimes suddenly.
- Dermal (skin) hemangiosarcoma: Can appear as a skin mass. Some are more superficial and may behave less aggressively than internal forms, but others can still be serious.
Hemangiosarcoma is seen more often in middle-aged to older dogs. Certain breeds are overrepresented (like German Shepherds, Golden Retrievers, and Labradors), but any dog can be affected.
Types and what they look like
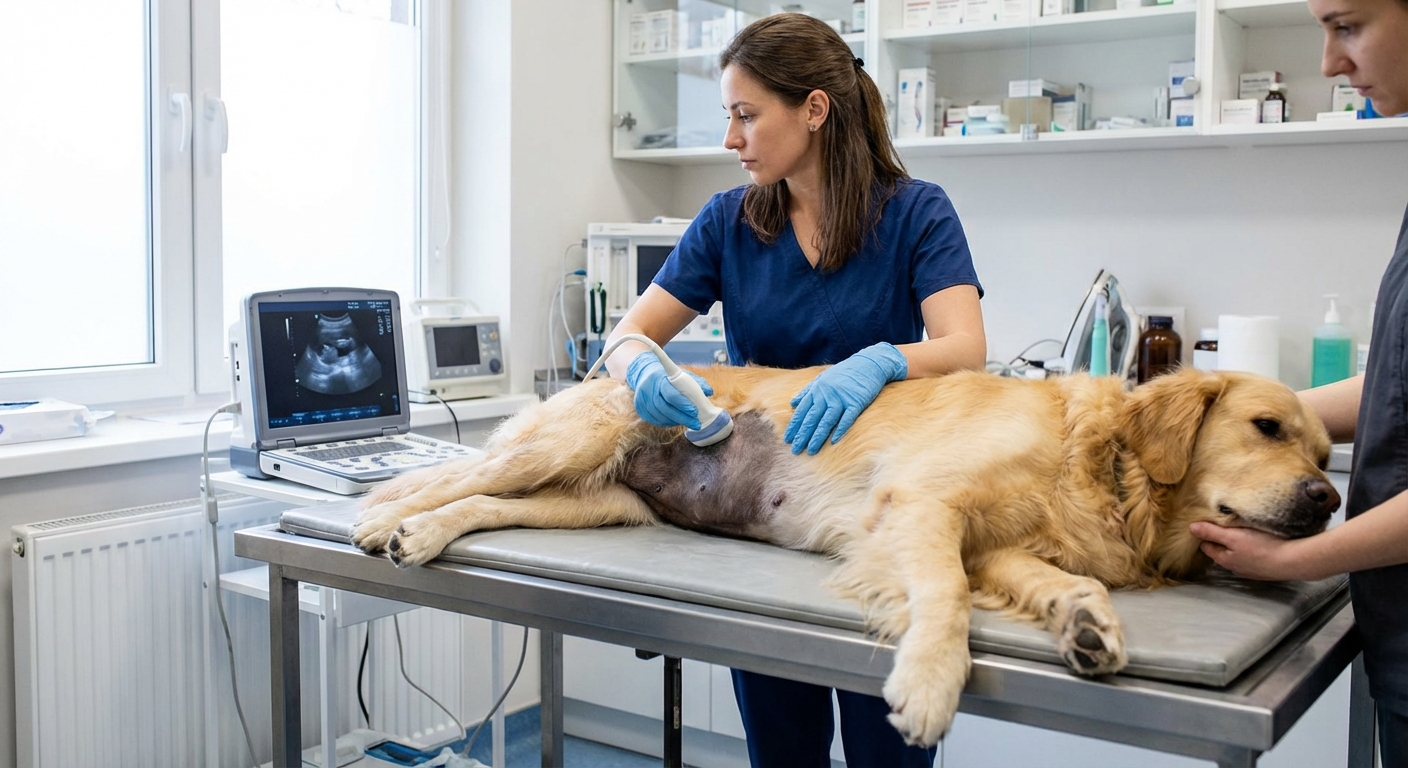
Splenic hemangiosarcoma
The spleen is an organ involved in filtering blood and supporting immune function. HSA tumors in the spleen can grow large without being noticed. Many dogs do not show clear signs until the tumor leaks or ruptures.
Important note: not every splenic mass is hemangiosarcoma. Benign causes (like hematomas or nodular hyperplasia) can also bleed and look similar on ultrasound. The only way to know for sure is usually lab testing of tissue, often after the spleen is removed.
What owners might notice: a sudden low-energy day, weakness after exercise, pale gums, a swollen-looking belly, or collapse that seems to come out of nowhere.
Cardiac hemangiosarcoma
When HSA affects the heart, it can lead to pericardial effusion (fluid or blood around the heart). This can prevent the heart from filling properly, which reduces blood flow to the body. In some cases, abdominal distension can occur secondary to fluid buildup, but it is not as direct or as common a hallmark as internal abdominal bleeding.
What owners might notice: fainting episodes, sudden weakness, labored breathing, restlessness, or a dog who cannot get comfortable lying down.
Hepatic (liver) hemangiosarcoma
Hepatic HSA can develop as one or more masses in the liver. Like splenic tumors, these can be very fragile and can bleed into the abdomen. Signs can overlap heavily with splenic disease, which is why ultrasound is so valuable in an emergency workup.
What owners might notice: weakness, pale gums, belly distension, decreased appetite, or collapse that improves briefly and then returns.
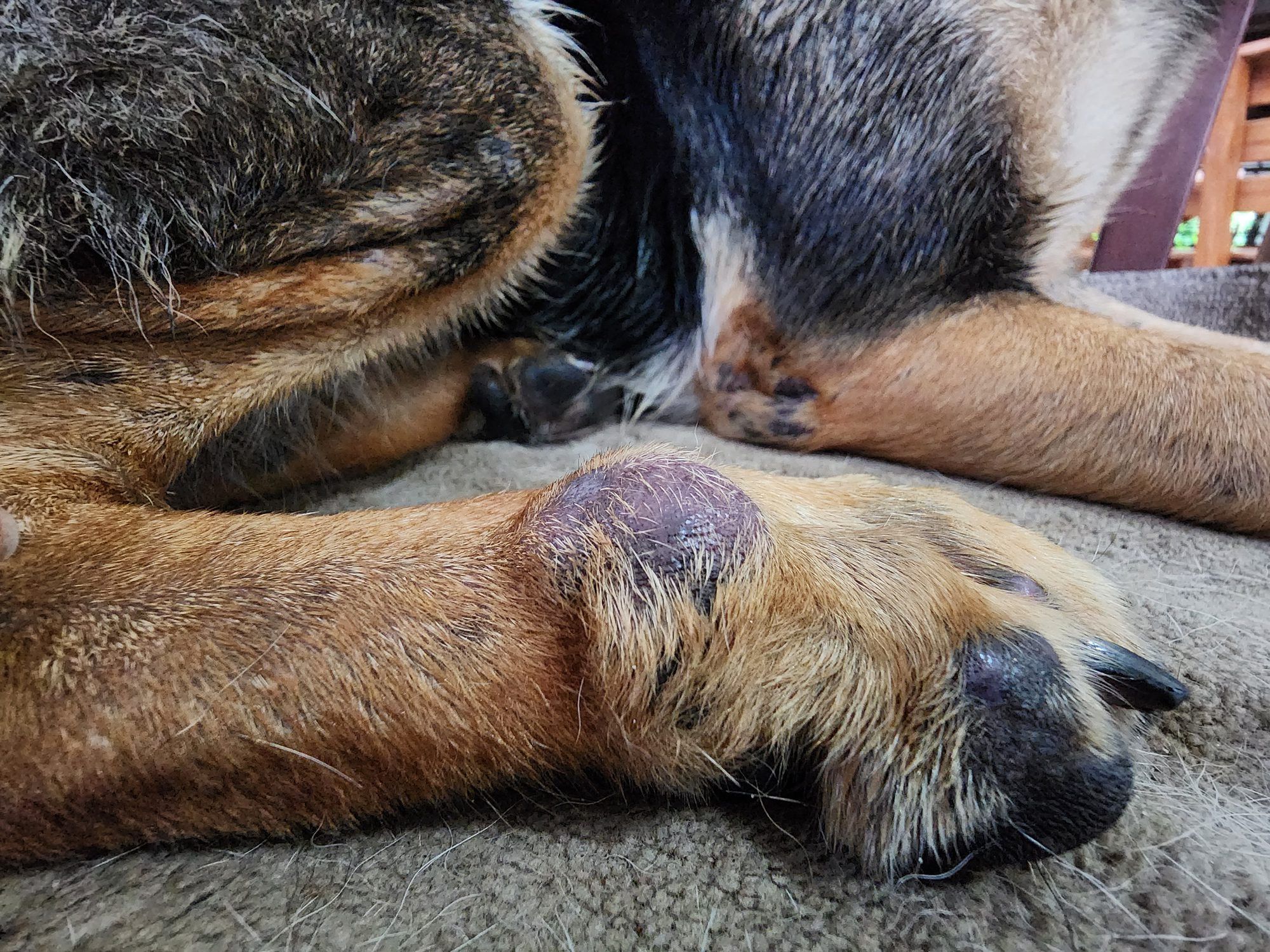
Dermal (skin) hemangiosarcoma
Dermal HSA may look like a bruised, red, purple, or black growth on the skin. Sometimes it resembles a “blood blister” or scab that will not heal. A veterinarian needs to sample or test it, because many harmless skin growths can look similar.
Early warning signs
Hemangiosarcoma is infamous for vague symptoms early on. Many families tell us they assumed it was normal aging or an upset stomach. Here are signs worth taking seriously, especially if they come and go:
- Intermittent weakness or “off days”
- Reduced stamina on walks or during play
- Decreased appetite or picky eating that is new
- Panting or restlessness without heat or exercise
- Abdominal distension or seeming “bloated”
- Pale gums or gums that look less pink than usual
- Rapid breathing or increased effort to breathe
- Episodes of collapse or near-fainting, then “back to normal”
- Unexplained bruising or a dark skin mass that changes quickly
If your dog has repeated “mystery” episodes that resolve, do not let that reassure you too much. With hemangiosarcoma, intermittent bleeding can temporarily stabilize, then worsen later.
Next, I want to be very clear about the signs that mean you should skip the “wait and see” approach and go in immediately.
Emergency signs (go to an ER now)
A ruptured splenic or liver mass can cause life-threatening internal bleeding. If you see the signs below, treat it like an emergency and go to the nearest veterinary ER immediately.
- Collapse or inability to stand
- Very pale or white gums
- Distended abdomen that appears to enlarge quickly
- Weakness, wobbliness, or disorientation
- Cold legs or ears or a body that feels unusually cool
- Rapid heart rate (you may feel pounding through the chest)
- Rapid breathing or breathing that looks strained
What to do while you are leaving: keep your dog warm, carry them if you can safely, and call the ER on the way so they can prepare. Do not give human pain medications.
If your dog collapses and then “perks back up,” you still need to be seen urgently. That pattern can happen with internal bleeding that temporarily slows.
What usually happens at the ER
Every hospital is a little different, but many emergency teams follow a similar flow:
- Triage and quick exam: gum color, heart rate, breathing effort, temperature, and blood pressure.
- IV access and stabilization: IV fluids, oxygen, pain control, and anti-nausea medications as needed.
- Rapid imaging: a FAST scan (a focused ultrasound) may be done quickly to check for free fluid in the abdomen or around the heart.
- Bloodwork: to assess anemia, platelet count, and organ function, and to help guide transfusion decisions.
- Transfusion planning: if bleeding is significant, a blood transfusion may be recommended before or during surgery.
- Big decision point: if a bleeding splenic mass is suspected and your dog is a surgical candidate, the team may recommend emergency splenectomy. If cardiac tamponade is present, they may recommend pericardiocentesis to remove fluid around the heart.
How it is diagnosed
Diagnosis usually happens in one of two ways: during an emergency visit for collapse or weakness, or during a workup for vague symptoms or a newly found mass.
Common tests your vet may recommend
- Physical exam: gum color, heart rate, belly palpation, signs of fluid, and overall stability.
- Bloodwork (CBC and chemistry): looks for anemia, low platelets, organ function changes, and evidence consistent with bleeding.
- Clotting tests: sometimes used if there is concern for bleeding disorders or surgical risk.
- Abdominal ultrasound: one of the most helpful tools for identifying a splenic or liver mass and checking other organs.
- Chest X-rays: checks the lungs for visible spread and evaluates the heart silhouette.
- Echocardiogram (heart ultrasound): especially important if cardiac HSA is suspected or if fluid around the heart is present.
- Abdominocentesis: if there is abdominal fluid, your vet may sample it to determine if it is blood and whether it clots.
Why sampling a splenic mass is tricky
Because these tumors can be very vascular, sticking a needle into a splenic mass can sometimes increase bleeding risk. Fine needle aspirates (FNA) can also be non-diagnostic because the sample may contain mostly blood. Whether to attempt sampling varies by clinician, your dog’s stability, and the hospital’s comfort level. Many dogs ultimately get a diagnosis after spleen removal (splenectomy) and lab testing of the mass.

Staging
“Staging” is the process of evaluating how advanced the cancer is. It helps guide treatment decisions and gives you a more realistic outlook.
Typical staging workup
- Imaging: chest X-rays and abdominal ultrasound, sometimes CT depending on availability and goals.
- Heart evaluation: echocardiogram if indicated.
- Sampling suspicious lesions: if there are enlarged lymph nodes or liver changes.
Common staging categories (general)
Staging systems can vary a bit by hospital, but many vets describe hemangiosarcoma in these broad terms:
- Stage I: primary tumor is present, no evidence of spread, and no rupture or major bleeding event.
- Stage II: rupture or bleeding and/or regional lymph node involvement (local spread).
- Stage III: metastatic disease is detected (spread to organs such as liver, lungs, omentum, or elsewhere).
Even with good imaging, microscopic spread can be present but not yet visible. That is one reason hemangiosarcoma is so challenging.
Treatment options
Treatment depends on tumor location, whether your dog is stable, overall health, and your goals. In many cases, the plan includes emergency stabilization, surgery, and then discussion of chemotherapy.
Emergency stabilization
- IV fluids to support circulation
- Blood transfusion if anemia or shock is severe
- Oxygen support when needed
- Pain control and anti-nausea medications
Surgery
Splenic HSA: Splenectomy (removing the spleen) is the standard approach when a splenic mass is bleeding and your dog is a surgical candidate. Surgery can be lifesaving in the short term by stopping internal bleeding. The removed tissue is sent to a pathologist for diagnosis.
Hepatic HSA: Surgery may be an option in select cases depending on the location and extent of the mass (for example, if a portion of the liver can be removed safely). Your vet may recommend referral to a specialty surgeon.
Cardiac HSA: Surgery is more complex and often not curative. Management may involve removing fluid around the heart (pericardiocentesis). Because effusion can recur, some dogs are referred to a cardiologist to discuss options like a pericardiectomy (surgically creating a window in the sac around the heart) and how that fits into an overall oncology plan.
Dermal HSA: Surgical removal with clean margins is often recommended. Superficial tumors that are fully removed may have a better outcome than internal forms, but staging is still important.
Chemotherapy
Chemotherapy is commonly recommended after splenectomy when hemangiosarcoma is confirmed, because the risk of microscopic spread is high. Your oncology team will tailor the protocol, but many plans involve several treatments over a few months, with monitoring visits in between.
One thing I like owners to know up front: veterinary chemo is usually aimed at quality of life. Many dogs tolerate it better than people expect, though side effects can still happen.
Palliative care (comfort-focused care)
Some families choose comfort care only, especially if cancer is advanced, the dog has other serious health issues, or the stress of aggressive treatment does not fit their goals. Palliative care can include:
- Pain management
- Anti-nausea and appetite support
- Activity adjustments and mobility help
- Short, calm routines that prioritize comfort
Your vet can help you plan what to do if another bleeding episode occurs, so you are not making decisions in a panic.
Prognosis by stage
It is completely fair to ask, “How much time do we have?” Prognosis varies based on location, stage, whether rupture occurred, and whether chemo is pursued. Your veterinarian or veterinary oncologist can give the most accurate expectations for your specific dog.
General expectations
- Surgery alone (splenic HSA): often provides a shorter survival time than surgery plus chemotherapy, because metastasis is common.
- Surgery plus chemotherapy: often extends survival compared with surgery alone, and may provide more good-quality time.
- Stage III disease: prognosis is typically poorer due to confirmed spread.
- Dermal HSA: can have a better outlook if it is superficial and fully removed early, but deeper or subcutaneous forms behave more aggressively.
Ballpark timelines (with big caveats)
Families often want approximate ranges. These numbers can vary a lot based on stage, overall health, and treatment choices, so use them as a general orientation and not a promise:
- Splenectomy alone for splenic HSA: commonly measured in weeks to a few months in many published reports.
- Splenectomy plus a doxorubicin-based chemotherapy protocol: often measured in a few months, with some dogs doing longer.
- Advanced metastatic disease: often shorter, especially if recurrent bleeding episodes occur.
Even when we cannot cure hemangiosarcoma, treatment can sometimes give families meaningful extra time, especially when the dog feels good after recovering from surgery and is enjoying normal routines again.
Quality of life
Quality of life is the center of decision-making with hemangiosarcoma. A plan that looks good on paper is not helpful if your dog is uncomfortable or anxious all the time.
Signs your dog is doing well
- Comfortable breathing and normal gum color
- Interest in food and hydration
- Enjoyment of short walks and favorite activities
- Resting comfortably and sleeping well
- Good engagement with family
Signs you should call your vet promptly
- Weakness, wobbliness, or new exercise intolerance
- Pale gums, sudden panting, or restlessness
- Swollen belly or signs of pain
- Refusing food for more than a day, especially with lethargy
- Collapse, even if brief
Practical ways to support your dog
- Keep routines simple: predictable meals, short walks, and calm rest time.
- Prevent slips and falls: add rugs or traction where your dog gets up and down.
- Track the basics: appetite, energy, breathing rate at rest, gum color, and any collapse episodes.
- Ask about a “crisis plan”: what ER to use, when to go, and whether transfusion or surgery would be considered if bleeding happens again.
If you are also thinking about nutrition support, talk with your veterinarian or a board-certified veterinary nutritionist, especially if your dog is in treatment. There is no one “anti-cancer diet” that fits every dog, but there are safe ways to keep meals enticing, maintain weight, and avoid risky supplements that can interfere with medications.

Questions to ask
- Based on imaging, what stage do you suspect and what findings make you think that?
- Is my dog stable enough for surgery, and what are the most likely risks?
- If the spleen is removed, what will you send to the lab and how long do results take?
- Do you think this could be a benign splenic mass, and how does that affect decision-making?
- Would you recommend chemotherapy, and what benefits are realistic for my dog?
- How will we monitor for metastasis or recurrence?
- What symptoms mean I should go to the ER right away?
- Can you help me set a quality of life checklist for my dog at home?
Final thoughts
Hemangiosarcoma moves fast, but you are not powerless. Knowing the subtle signs, seeking diagnostics early, and having an emergency plan can make a real difference in how supported you feel and how quickly your dog gets care. If you are in the middle of a diagnosis right now, please be gentle with yourself. You do not have to make every decision perfectly. You just have to keep coming back to the same question: what gives my dog the best comfort and the best day today?