Bloodshot eyes in dogs can signal allergies, conjunctivitis, dry eye, corneal ulcers, foreign bodies, glaucoma, or uveitis. Learn urgent warning signs and sa...
Article
•
Designer Mixes
Glaucoma in Dogs

Shari Shidate
Designer Mixes contributor
Glaucoma in dogs is one of those conditions I never want pet parents to “wait and see” on. It happens when pressure inside the eye (intraocular pressure, or IOP) rises high enough to damage the optic nerve and retina. That damage can become permanent very quickly, sometimes within hours, especially with very high pressures. Exact timelines vary, but the takeaway is the same: this is a true emergency. The good news is that rapid treatment can reduce pain and may save vision, especially if you act quickly.

If your dog has a suddenly red, painful, cloudy-looking eye or is squinting and acting unwell, treat it like an emergency and contact an emergency vet or veterinary ophthalmologist right away.
Glaucoma symptoms in dogs
Glaucoma can look like “just an irritated eye” at first, but there are a few classic signs that should immediately raise concern.
Common warning signs
- Red eye, especially if it appeared quickly
- Cloudy or blue-gray cornea (the clear surface of the eye looks hazy)
- Dilated pupil (the black center looks larger than normal) or pupils that are different sizes
- Squinting or blinking more than usual
- Excess tearing or watery discharge
- Eye rubbing or pawing at the face
- Light sensitivity
- Vision changes like bumping into objects, hesitating on stairs, or acting “spooky” in familiar rooms
Signs your dog is in pain
Increased eye pressure is painful. Some dogs show obvious discomfort, and others get quiet and withdrawn.
- Holding the eye closed
- Head-shyness (not wanting you to touch the face)
- Restlessness or trouble settling
- Lethargy
- Decreased appetite
Later or severe signs
- Bulging or enlarged-looking eye (buphthalmos, meaning an enlarged globe), especially if it develops over time
- Visible corneal swelling that makes the eye look blue-white
- Sudden blindness in one eye
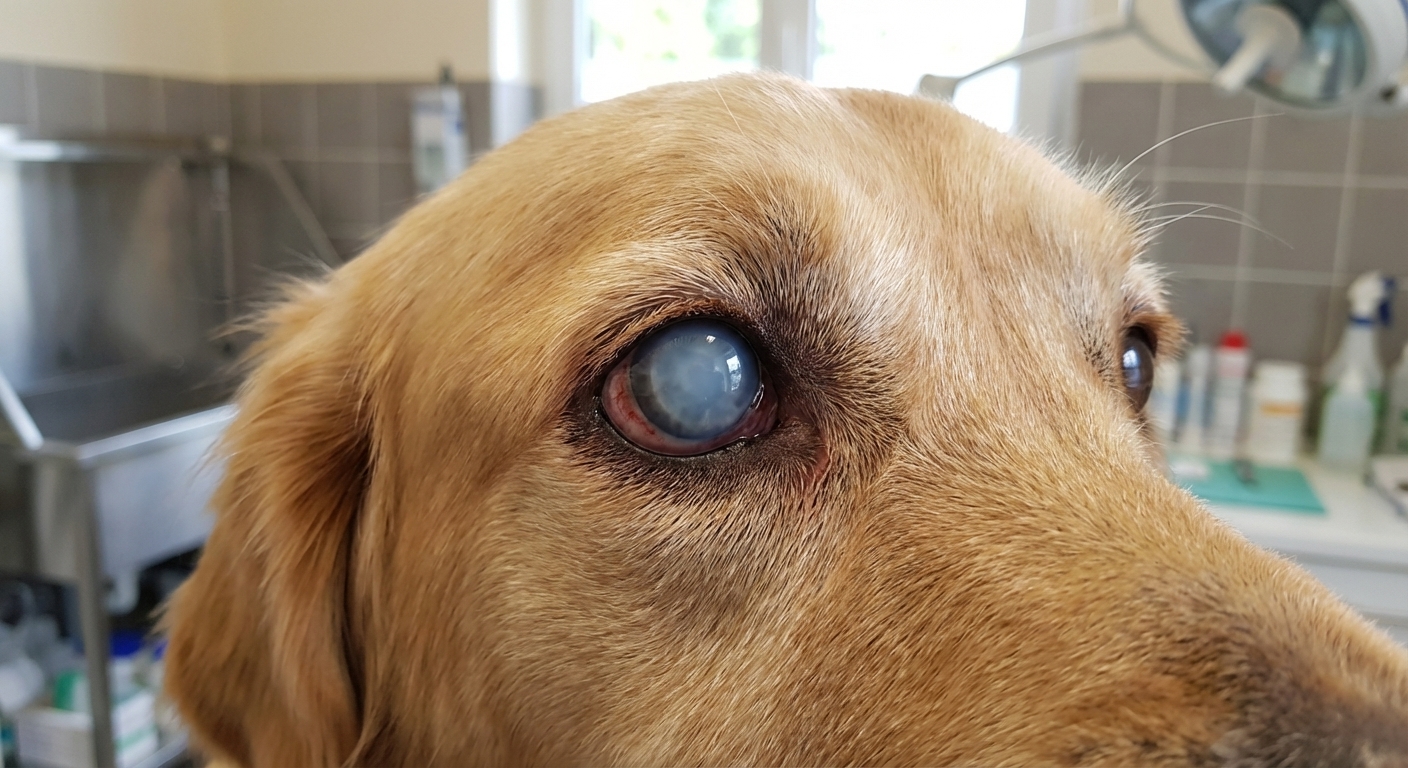
Why glaucoma is an emergency
Glaucoma is not just “high pressure.” That pressure can damage delicate eye structures and injure the optic nerve. Once the optic nerve is harmed, vision may not return even if pressure is later controlled.
From a practical standpoint, glaucoma is an emergency for two reasons:
- Vision can be lost quickly, sometimes within hours to a day in severe cases.
- It is extremely painful, even when your dog is trying to be brave about it.
If your regular vet is not open, an emergency hospital can provide pain control and pressure-lowering medications and can help you reach a veterinary ophthalmologist for urgent follow-up.
Primary vs. secondary glaucoma
Understanding which type of glaucoma your dog has helps explain why it happened and what the long-term plan looks like.
Primary glaucoma
Primary glaucoma is usually inherited. It is caused by abnormal drainage anatomy inside the eye, so fluid cannot exit normally and pressure rises.
- Often affects both eyes eventually, even if it starts in one.
- May come on suddenly (acute) or progress more slowly (chronic).
- Long-term management often includes lifelong medications and close monitoring.
If your dog is diagnosed with primary glaucoma in one eye, your vet or ophthalmologist will usually talk to you about monitoring (and sometimes treating) the other eye. Preventative drops may help delay onset in the second eye, but they do not guarantee it will never happen.
Secondary glaucoma
Secondary glaucoma happens because something else in the eye disrupts normal drainage or eye function.
Common causes include:
- Uveitis (inflammation inside the eye)
- Lens luxation (the lens shifts out of place)
- Advanced cataracts and lens-related inflammation
- Eye tumors
- Trauma
- Bleeding inside the eye (hyphema) or significant internal inflammation that interferes with drainage
With secondary glaucoma, treating the underlying cause is just as important as lowering the pressure.
Breeds at higher risk
Any dog can develop glaucoma, but primary (inherited) glaucoma is more common in certain breeds. If you have a breed on this list, it is worth being extra alert to any eye changes and asking your vet about routine eye exams.
- American Cocker Spaniel
- Basset Hound
- Beagle
- Chow Chow
- Shar-Pei
- Siberian Husky
- Shih Tzu
- Poodle (especially Miniature)
- Jack Russell Terrier
- Boston Terrier
- Samoyed
This list is not exhaustive, and breed risk varies by family lines and region. Breed risk does not mean it is inevitable. It simply means the threshold for acting fast should be very low if symptoms appear.

Emergency signs that need same-day care
If you notice any of the signs below, seek veterinary care immediately. These are “drop what you are doing” symptoms.
- Sudden cloudy or blue-white eye
- Red eye with squinting, especially if it came on fast
- One pupil suddenly much larger than the other
- Eye looks enlarged or bulging
- Severe tearing and obvious pain
- Sudden vision loss, bumping into objects, or disorientation
- Vomiting, extreme lethargy, or hiding along with an abnormal eye (pain can make dogs feel very sick)
Important: Avoid using leftover eye medications from another pet or an old prescription. Some drops are unsafe depending on the cause, especially if there is an ulcer or certain types of inflammation. A vet needs to examine the eye and measure pressure first.
How vets diagnose glaucoma
Diagnosis is based on a combination of exam findings and pressure testing.
- Tonometry: measures intraocular pressure quickly and comfortably. Normal canine IOP is often roughly 10 to 25 mmHg (ranges vary by device and clinic). Glaucoma is commonly suspected when pressures rise above the mid-20s to 30s, but the diagnosis is still clinical, not just one number.
- Fluorescein stain: checks for corneal ulcers, which can change what medications are safe.
- Full eye exam: evaluates the lens, retina, and internal eye structures.
- Gonioscopy (often by an ophthalmologist): evaluates the eye’s drainage angle, helpful for diagnosing primary glaucoma and assessing the “at risk” eye.
Treatment options
Glaucoma treatment has two urgent goals: lower the eye pressure and control pain. The longer-term goal depends on whether vision is still present and whether the glaucoma is primary or secondary.
1) Eye drops to lower pressure
Medications are tailored to the case, but commonly include:
- Prostaglandin analogs (often used for acute pressure spikes). These are not appropriate for every case and may be used cautiously or avoided with certain conditions like some lens luxations or significant uveitis.
- Carbonic anhydrase inhibitors (reduce fluid production). Common examples include dorzolamide.
- Beta blockers (reduce fluid production, often combined with other drops). A common example is timolol (often paired with dorzolamide).
Your vet will tell you exactly how often to dose. In an emergency, drops may be needed very frequently at first.
2) Oral and hospital medications
Some dogs need oral medications to help reduce pressure systemically, especially during acute episodes. In severe cases, hospitals may use additional medications such as IV osmotic agents (for example, mannitol) when appropriate. These can be very effective but must be prescribed and monitored by a veterinarian.
3) Treating the underlying cause (secondary glaucoma)
If glaucoma is secondary, additional treatments may include anti-inflammatory medications for uveitis, addressing lens luxation, managing advanced cataract complications, or investigating a mass.
4) Surgery and advanced procedures
When medications are not enough, or if the goal is to preserve remaining vision, your vet may refer you to a veterinary ophthalmologist for procedures such as:
- Cyclophotocoagulation (laser treatment to reduce fluid production)
- Cyclocryotherapy (freezing treatment to reduce fluid production)
- Drainage implants to help fluid exit the eye
- Lens surgery if lens luxation is contributing
5) When the eye is blind and painful
If vision is permanently lost and the eye remains painful, the kindest goal becomes long-term comfort. Options may include:
- Enucleation (surgical removal of the eye), which often provides the fastest, most reliable pain relief
- Prosthetic options in select cases
- Ciliary body ablation (a procedure intended to reduce pressure and pain in a non-seeing eye). This is very case-dependent and can be done using different techniques. Your ophthalmologist will walk you through risks, benefits, and whether it is a good fit for your dog.
I know the idea of eye removal can feel overwhelming. Many dogs bounce back quickly and feel noticeably better once the pain source is gone. Dogs adapt incredibly well to vision changes, especially when pain is controlled.

Prognosis: can my dog keep their vision?
Prognosis depends on how quickly treatment starts, how high the pressure is, and what caused the glaucoma.
- If treated early and aggressively, some dogs keep useful vision, especially in acute cases caught quickly.
- If pressure has been high for too long, vision loss can be permanent even if the eye looks better later.
- Primary glaucoma often requires long-term management and the second eye is frequently at risk.
- Secondary glaucoma may improve if the underlying cause can be corrected, but outcomes vary widely.
Your veterinarian or ophthalmologist may recommend monitoring the “other” eye closely, and in some high-risk cases, using preventative medication. The goal is to buy time and catch changes before a crisis happens.
What you can do at home right now
If you suspect glaucoma, the most helpful thing you can do is move quickly and keep your dog as comfortable as possible while you get to care.
- Call ahead to your ER vet and tell them you suspect glaucoma, so they can prepare.
- Prevent rubbing by using an e-collar if you have one.
- Keep lighting soft if your dog seems light-sensitive.
- Do not use human eye drops unless a veterinarian specifically instructed you to.
- Do not give human pain medications unless your veterinarian prescribed them. Some are dangerous for dogs.
- Bring medications your dog is currently on, including any eye meds.
If your dog has had glaucoma in one eye, ask your vet what to watch for in the other eye and how often pressure checks should be done. Having a plan in place can save precious time later.
When to see a veterinary ophthalmologist
Many general practice veterinarians can start emergency treatment, but glaucoma management often benefits from an ophthalmologist, especially when surgery is on the table or if the diagnosis is unclear.
Consider urgent referral if:
- Pressure is not controlled within hours to a day
- Vision is changing
- Your dog has a high-risk breed history or suspected primary glaucoma
- Secondary causes like lens luxation or severe uveitis are suspected
Quick FAQ
Can glaucoma look like pink eye?
Yes. Both can cause redness and discharge. The difference is that glaucoma typically involves pain, often a cloudy cornea, and sometimes a dilated pupil or vision changes. Because they can look similar at first, a same-day exam is the safest approach.
Is glaucoma contagious?
No. Glaucoma is not contagious. But some causes of secondary eye inflammation may be related to underlying disease, so your veterinarian will look at the whole picture.
Will my dog be okay if they lose vision in one eye?
Many dogs do very well with vision loss in one eye, and even with complete blindness, as long as pain is controlled and the home environment is kept consistent. Dogs rely heavily on smell and hearing, and they adapt better than most people expect.
A final word from a vet assistant perspective
If there is one takeaway, it is this: glaucoma is a pain emergency and a vision emergency. You are not overreacting by going in right away. Fast care can make a real difference in comfort, and sometimes in whether vision can be saved.
Medical note: This article is for education and is not a substitute for veterinary diagnosis or treatment. If your dog has sudden eye changes, contact a veterinarian immediately.



