Learn liver-friendly homemade dog food strategies: when to restrict copper, pick digestible proteins and gentle carbs, what ingredients to avoid, and simple ...
Article
•
Designer Mixes
Dog Liver Problems Quick Guide

Shari Shidate
Designer Mixes contributor
As a veterinary assistant in Frisco, Texas, I have learned that “liver problems” in dogs can mean a lot of different things. Sometimes it is a mild, temporary irritation. Other times, it is a true emergency. The good news is that when pet parents know what to watch for and act quickly, many dogs do very well.
This guide will help you recognize common signs, understand what your vet is looking for, and support your dog safely at home while you get proper medical care.
Quick note about my role: I am not a veterinarian, but I work alongside veterinarians every day. I will share what we commonly see in clinic and what is generally recommended, but your vet is the one who diagnoses and prescribes.

What the liver does (and why it matters)
Your dog’s liver is a powerhouse organ. It processes nutrients, helps with digestion, stores energy, supports blood clotting, and filters toxins and medications. Because it does so many jobs, liver disease can look like many other health problems at first.
One important detail: the liver has a lot of “reserve capacity.” A dog can have significant liver changes before obvious symptoms show up. That is why routine lab work can catch issues early.
Fast symptom check
Many of these signs are common and can happen with lots of illnesses, not just liver disease. The pattern, severity, and how quickly things change are what help your vet narrow it down.
Common signs you might notice at home
- Low appetite or suddenly becoming picky
- Vomiting and/or diarrhea
- Lethargy, weakness, less interest in walks or play
- Weight loss over weeks to months
- Increased thirst and urination
- Abdominal swelling or a “pot-bellied” look
- Yellow tint to the eyes, gums, or skin (jaundice)
- Behavior changes such as disorientation, staring, stumbling, or seeming “not themselves”
- Bruising, nosebleeds, or bleeding gums (can relate to clotting problems)
- Color clues: dark orange-brown urine, or pale/gray stool (can be seen with bile flow problems)
Red flags: go to an ER now
- Yellow gums or eyes with vomiting, weakness, or collapse
- Repeated vomiting and inability to keep water down
- Swollen belly plus trouble breathing
- Seizures, severe wobbliness, or extreme confusion
- Suspected toxin exposure (xylitol, rodenticide, sago palm, blue-green algae, human medications like acetaminophen, mushrooms, moldy foods)
If you think your dog ate something toxic, bring the package or a photo of the label if you can. That can save valuable time.
Same-day call to your vet (do not wait)
- Vomiting or diarrhea lasting more than 24 hours, or any blood in vomit or stool
- Not eating for a full day (especially in small dogs, seniors, or dogs with other medical conditions)
- New jaundice, even if your dog otherwise seems “okay”
- Noticeably increased drinking and urination that is new for your dog
- Newly dark urine or very pale stools
What causes liver problems in dogs?
“Liver problems” is a broad umbrella. Here are common categories your veterinarian may consider.
1) Toxins and medications
Some toxins directly injure liver cells. Certain medications can also stress the liver, especially if the dose is too high, the dog has a sensitivity, or multiple drugs are combined. Never give human medications unless your veterinarian specifically instructs you to.
2) Infection and inflammation
Viral, bacterial, and parasitic infections can affect the liver. In some cases, inflammation is immune-mediated, meaning the immune system attacks liver tissue.
3) Gallbladder and bile flow problems
The liver produces bile to help digest fats. If bile flow is blocked or sluggish, dogs can become very sick. Gallbladder mucoceles, for example, can be serious and sometimes require surgery.
4) Chronic hepatitis and copper-associated disease
Some dogs develop long-term inflammation (chronic hepatitis). Certain breeds are more prone to copper accumulation, which can damage liver tissue over time. Diet and medication plans can be tailored once your vet identifies the cause.
5) Congenital issues like portosystemic shunts
A shunt is an abnormal blood vessel that bypasses the liver. Dogs can show slow growth, picky appetite, digestive upset, and neurologic signs, especially after meals. Shunts are often diagnosed in younger dogs and may be managed with diet and medications or corrected surgically depending on type.
6) Cancer or benign liver masses
Not every liver mass is cancerous, but any suspected mass deserves prompt imaging and a plan. Many dogs with liver masses have no signs at first.
What your vet will test (and what it means)
When liver disease is suspected, your veterinarian typically builds a “big picture” using multiple tests. One elevated value rarely tells the whole story.
Liver enzymes vs liver function
This is one of the most confusing parts for pet parents. Elevated enzymes often suggest liver or bile duct irritation, inflammation, or “stress,” but they do not automatically mean liver failure. Liver function looks at whether the liver is still doing its jobs, like processing waste products and making key proteins.
Common diagnostics
- Blood chemistry: looks at enzymes (often ALT, AST, ALP, GGT) and function-related markers like bilirubin, albumin, glucose, and cholesterol.
- CBC (complete blood count): checks for anemia, infection patterns, and platelet counts.
- Urinalysis: can show bilirubin, concentration issues, and clues that guide next steps.
- Bile acids test: evaluates liver function and blood flow through the liver, often used when a shunt is suspected.
- Coagulation testing: checks clotting ability, important before procedures and in more severe disease.
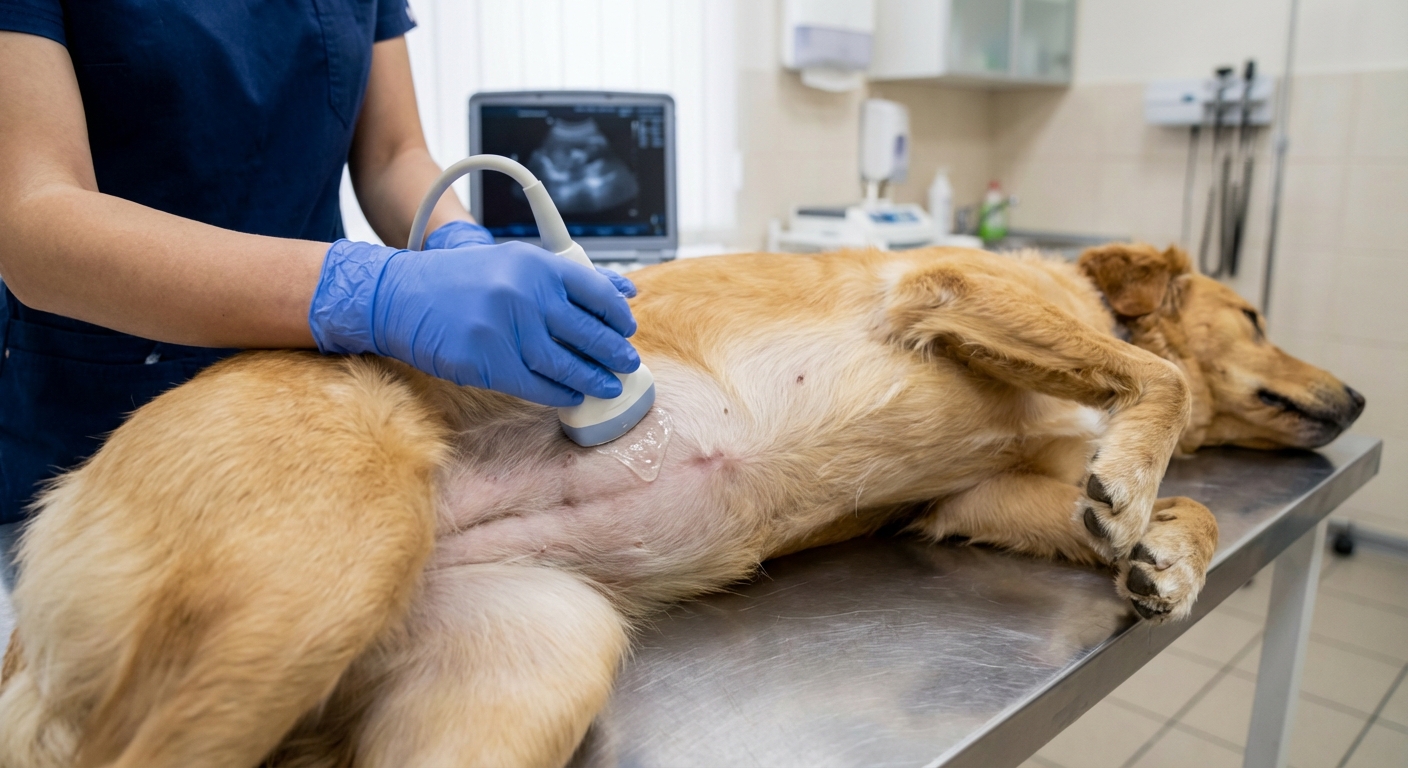
- Ultrasound: evaluates liver texture, bile ducts, gallbladder, and blood flow patterns.
- Sampling: fine needle aspirate or biopsy may be recommended to confirm diagnosis and guide treatment.
Quick note: elevated liver enzymes can happen for reasons that are not primary liver disease, including pancreatitis, endocrine disease (like Cushing’s), diabetes, and steroid medications. That is why follow-up testing and context matter.
Treatment basics you may hear about
Treatment depends on the cause. Your vet’s plan might include a combination of the following.
Medications and supportive care
- Fluids to correct dehydration and support circulation
- Anti-nausea medications and GI protectants
- Antibiotics if infection is suspected or confirmed
- Lactulose and sometimes antibiotics to reduce ammonia in dogs with hepatic encephalopathy (brain effects)
- Ursodiol to support bile flow in appropriate cases, typically after imaging confirms it is safe. It is generally avoided if complete biliary obstruction is suspected.
- SAMe and silybin (milk thistle extract) are commonly used liver-support supplements. Evidence is moderate and varies by condition and product, so ask your veterinarian about whether they fit your dog’s case and which brands to trust.
- Vitamin K may be used in specific situations, such as certain toxin exposures (like anticoagulant rodenticides) or when testing suggests it will help. It is not a universal fix for every liver-related clotting problem.
Diet changes
Nutrition is one of the most powerful tools for liver support. Many dogs do better with:
- Highly digestible diets that are gentle on the GI tract
- Appropriate protein: not always “low protein,” but the right type and amount for that specific dog
- Controlled copper if copper accumulation is a concern
- Omega-3 fats in vet-approved amounts for inflammation support
If you love the idea of fresh food, that can be a great option, but liver patients are not the place for guessing. Work with your veterinarian or a board-certified veterinary nutritionist so the diet is balanced and targeted to your dog’s diagnosis.
What you can do at home right now
If your dog is stable and you are waiting for an appointment or test results, these steps can help you stay focused and avoid common missteps.
Safe, helpful steps
- Write down symptoms: when they started, what changed, and whether it relates to meals.
- Track food, water, and bathroom habits: appetite, thirst, vomiting episodes, stool color, urine color, and frequency.
- Bring a full medication list: include supplements, flea and tick products, and any people meds your dog could access.
- Offer small, frequent meals if your dog is nauseated, only if your vet has not instructed fasting.
- Prevent access to toxins: secure trash, gum, grapes and raisins, rodenticides, and backyard hazards.
Please avoid these common mistakes
- Do not give acetaminophen, ibuprofen, naproxen, or aspirin unless a veterinarian directs you. Many are toxic to dogs.
- Do not start “detox” products or essential oils. Some can worsen liver stress.
- Do not switch to an extreme homemade diet without guidance. Imbalances can hurt recovery.
- Do not wait on jaundice, belly swelling, or neurologic signs.

How to talk to your vet
When you are worried, it is easy to forget what you wanted to ask. Here are a few high-value questions that keep the appointment productive:
- Which liver values are abnormal, and do they suggest liver injury, bile flow issues, or decreased liver function?
- Do we need a bile acids test or clotting test?
- Is ultrasound recommended, and how soon?
- Could any current medications or supplements be contributing?
- What symptoms mean my dog should go to the ER?
- What diet do you recommend right now, and should we consult a veterinary nutritionist?
Prognosis and hope
I want to leave you with something encouraging: many liver conditions are treatable, and the liver can regenerate remarkably well when the underlying cause is addressed. The most important thing you can do is act early, follow your veterinarian’s plan closely, and keep communication open if symptoms change.
This guide is educational and not a substitute for veterinary care. If your dog has jaundice, repeated vomiting, abdominal swelling, or neurologic signs, seek urgent veterinary attention.



