Know the most common dog cancer warning signs—new lumps, weight loss, lethargy, vomiting, breathing trouble, bleeding, swollen lymph nodes—and when to se...
Article
•
Designer Mixes
Dog Cancer Signs: Insights & Help

Shari Shidate
Designer Mixes contributor
As a veterinary assistant here in Frisco, Texas, I have sat with many families who felt blindsinded by a cancer diagnosis. What I want you to know is this: sometimes the signs are loud, but often they are quiet and easy to explain away as “just getting older.” This page is here to help you notice what matters, act early, and feel more confident walking into your vet visit.
Quick note from me: I cannot diagnose cancer. This is educational guidance to help you know what to watch for and how to talk with your veterinarian.

Important: Only a veterinarian can diagnose cancer. If you notice a change that persists, worsens, shows up in multiple areas (appetite, energy, weight, breathing, bathroom habits), or feels “not right,” it is time to call your vet. Breathing trouble, collapse, pale gums, or uncontrolled bleeding are always urgent.
Why early detection matters
Cancer is common in dogs, especially as they age, but “common” does not mean “hopeless.” Many cancers can be treated or managed when caught earlier, and even when cure is not possible, earlier care often means better comfort and more good days.
The tricky part is that many cancer signs overlap with other conditions like arthritis, dental disease, allergies, infections, or gastrointestinal upset. That is why trends matter: changes that stick around, progress, or keep returning deserve a closer look.
If your dog is a senior, proactive care helps too. Many vets recommend twice-yearly exams and periodic screening bloodwork and urinalysis to catch problems earlier, cancer and non-cancer alike.
Common dog cancer signs to watch for
Use this as a practical checklist. One sign alone does not prove cancer, but it does justify paying attention and getting guidance.
Quick “7 warning signs” recap (classic veterinary messaging): lumps, non-healing sores, unexplained weight loss, bleeding or discharge, unusual odor, difficulty eating or swallowing, and persistent lameness or stiffness.
1) New lumps, bumps, or swelling
- New lump anywhere on the body, especially if it grows over days to weeks.
- Firm, fixed, irregular masses that feel attached under the skin.
- Swollen lymph nodes (commonly under the jaw, in front of the shoulders, behind the knees).
Many lumps are benign (like lipomas), but you cannot tell by feel alone. A quick fine needle aspirate (FNA) is often a helpful next step. Sometimes an FNA is non-diagnostic, and your vet may recommend a biopsy or removal to get a clear answer.
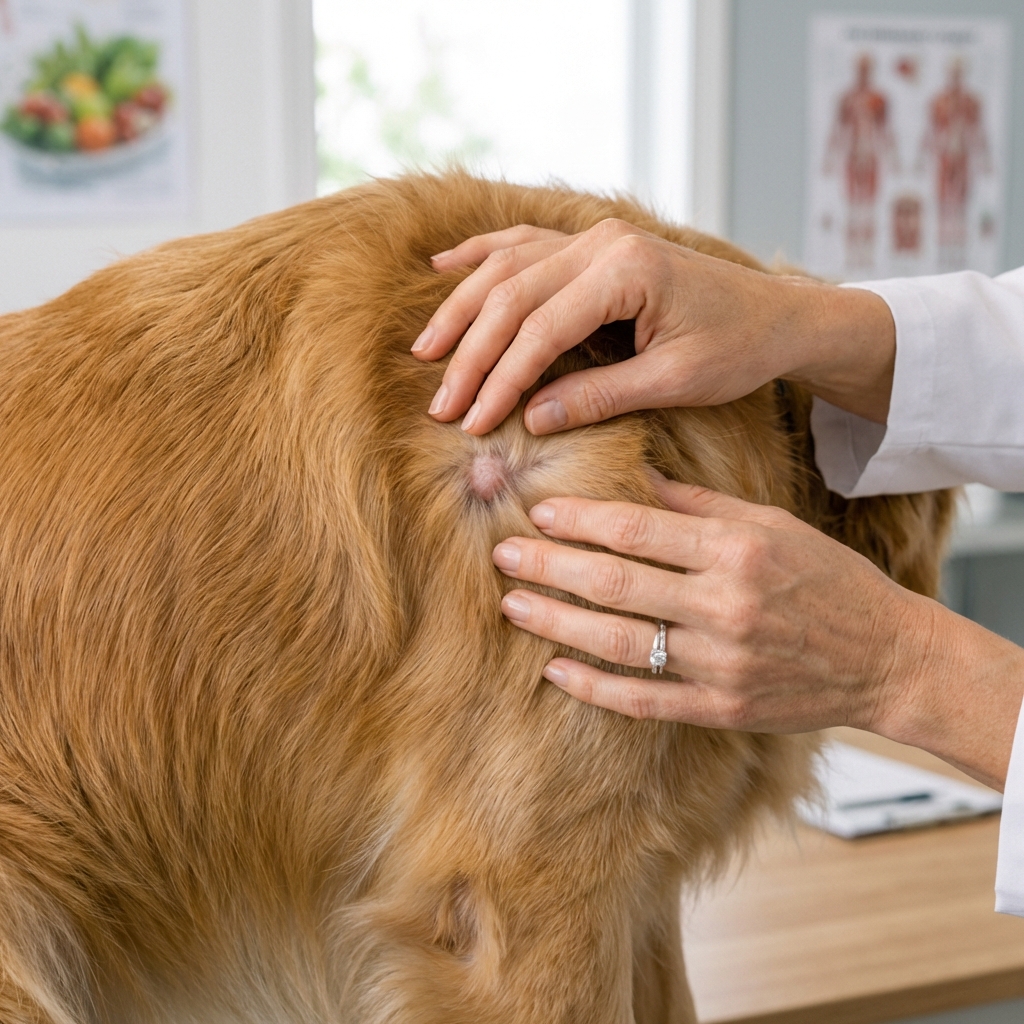
2) Unexplained weight loss or muscle loss
- Noticeable slimming despite normal food intake.
- Back end looking bony or weaker.
- Loss of appetite, especially in a dog who normally loves food.
Cancer can increase calorie needs and change metabolism. Weight loss can also signal many other illnesses, all worth addressing quickly.
3) Changes in eating, drinking, or bathroom habits
- Vomiting or diarrhea that persists, returns often, or includes blood.
- Straining to urinate or defecate.
- Accidents in a previously house-trained dog.
- Increased thirst and urination.
These signs can point to gastrointestinal disease, urinary issues, diabetes, kidney disease, or cancer. Your vet can sort this out with targeted testing.
4) Low energy, weakness, or exercise intolerance
- Fatigue that seems out of proportion to activity.
- Reluctance to walk, jump, or play.
- Collapse or episodes of extreme weakness.
Sometimes this is pain. Sometimes it is anemia, heart issues, internal bleeding, or systemic illness. If your dog seems “not themselves” and it is not improving, trust your instincts and call.
5) Persistent pain, limping, or stiffness
- Limping that does not improve with rest.
- Pain when touched, especially over a specific bone.
- Swelling of a limb.
Bone cancer can look like an injury at first. If your dog is limping and not improving, your vet may recommend X-rays and a pain assessment.
6) Coughing, breathing changes, or trouble swallowing
- Chronic cough, especially in an older dog.
- Fast breathing at rest.
- Gagging, retching, or difficulty swallowing.
These may be respiratory disease, heart disease, or sometimes tumors in the chest, throat, or mouth. Breathing changes should be treated as urgent.
7) Mouth issues: bleeding, odor, drooling, or visible growths
- Bad breath that is new or worsening.
- Drooling, pawing at the mouth, or chewing on one side.
- Bleeding from the mouth or nose.
- A dark or pink mass on the gums, tongue, or palate.
Oral tumors can hide until they are advanced, so routine dental checks matter. If your dog will not let you look, that is also a sign to schedule an exam.

8) Non-healing sores or recurrent infections
- Skin sores that do not heal.
- Repeated ear infections, skin infections, or urinary infections.
- Bleeding or discharge from any opening (nose, mouth, vulva, penis, rectum).
Some cancers can affect immune function, but recurrent infections are more often linked to issues like allergies, anatomy, endocrine disease, or chronic inflammation. Either way, patterns that keep coming back deserve a veterinary workup.
9) Pale gums, distended belly, or sudden weakness
These can be emergency signs. In some cases, tumors of organs like the spleen can bleed internally. If you see pale or white gums, a suddenly swollen abdomen, collapse, or extreme lethargy, seek emergency care immediately.
When to call the vet (and what to track at home)
If you are unsure, I always prefer a cautious call. You are not “overreacting” when you advocate for your dog.
Call your vet soon (often within 24 to 48 hours) if:
- A lump is growing, firm or fixed, ulcerated, painful, or larger than about 2 cm (roughly grape-sized).
- Your dog stops eating, or appetite is clearly decreased for more than a day.
- Vomiting or diarrhea lasts more than 24 hours, keeps returning, or includes blood.
- Your dog seems painful, hides, or avoids touch.
Go sooner (same day) or ask for urgent guidance if your dog is a puppy, a toy breed, diabetic, has other medical conditions, is on medications that affect appetite, or if not eating comes with vomiting, marked lethargy, or signs of dehydration.
Go to urgent or emergency care now (not cancer-specific) if:
- Breathing looks difficult or rapid at rest.
- Gums are pale, gray, or white.
- Collapse, inability to stand, or severe weakness.
- Bloated belly with distress or repeated unproductive retching (this can be GDV and is an emergency regardless of the cause).
- Uncontrolled bleeding.
Helpful notes for your vet
- Photos of lumps or swelling (same angle weekly).
- Measurements of a lump using a ruler.
- Weight every 1 to 2 weeks if possible.
- Appetite log: what was eaten, how much, and interest level.
- Bathroom notes: frequency, straining, accidents, stool quality.
- Resting respiratory rate (breaths per minute while asleep), especially for coughing dogs.
What your veterinarian may recommend
Testing can feel overwhelming, but it is simply a step-by-step process to answer three key questions: What is it? Where is it? Has it spread?
- Physical exam with a full lymph node check and oral exam.
- Fine needle aspirate of a lump or lymph node (often quick and minimally invasive).
- Biopsy if the aspirate does not give clear answers.
- Bloodwork and urinalysis to evaluate organ function and overall health.
- X-rays (chest and or limb) to assess lungs and bones.
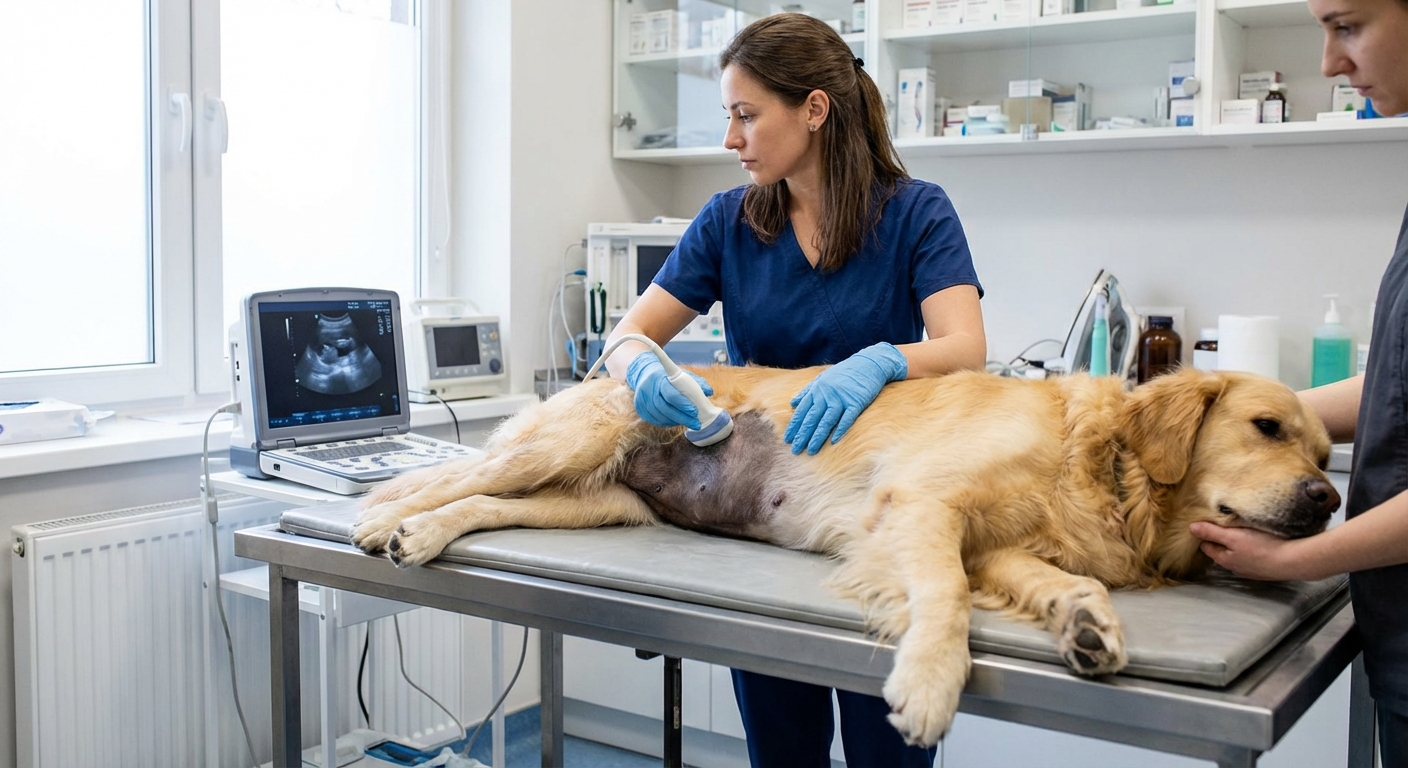
- Ultrasound to evaluate organs like liver, spleen, and intestines.
- CT or MRI for detailed imaging in certain cases.
If cancer is diagnosed, your vet may refer you to a veterinary oncologist. Oncology visits often focus on options, comfort, and realistic outcomes, not pressure. For some dogs and some cancer types, treatment may include surgery, chemotherapy, radiation, and in select cases targeted therapies or immunotherapy.
A gentle reminder: internet checklists can help you notice patterns, but cytology and biopsy are what identify many tumors.
Supportive care you can start today
Even before a final diagnosis, you can support your dog in gentle, evidence-based ways. Always run supplements and diet changes by your veterinarian, especially if your dog is starting medications or has kidney, liver, or pancreas concerns.
Nutrition: keep it simple
- Prioritize calories and protein if appetite is reduced. Preventing weight loss is a big deal.
- Offer small, frequent meals and warm food slightly to increase aroma.
- Choose highly digestible foods if the stomach is sensitive.
- Ask about a balanced home-prepared plan if you want to cook. Balance matters, especially for long-term feeding.
If you want to add fresh foods, keep it conservative unless your vet or a veterinary nutritionist guides you. A safe default is to keep “extras” to under 10 percent of daily calories so you do not accidentally unbalance a complete diet.

Pain control and comfort
- Do not use human pain meds unless your vet specifically instructs you. Many are toxic to dogs.
- Use non-slip rugs and a supportive bed to reduce strain.
- Keep nails trimmed to improve traction.
- Ask your vet about a pain plan if your dog is limping, panting, restless, or reluctant to move.
Stress reduction
- Keep routines predictable.
- Use quiet time, gentle grooming, and sniff walks if your dog enjoys them.
- Give medication and meals in calm, low-pressure moments.
If your dog is diagnosed: next steps
A cancer diagnosis can feel like the floor drops out from under you. But there are often more options than people realize, from surgery and chemotherapy to radiation and strong palliative care.
One of the most helpful questions to ask your vet or oncologist is: “What does a good day look like for my dog, and how do we protect that?” From there, you can make a plan that matches your dog’s personality, your family’s capacity, and your goals.
You do not have to do everything. You just have to do the next right step for your dog.
Quick FAQ
Are lumps always cancer?
No. Many lumps are benign. But because some dangerous tumors can look harmless, the safest path is to test new or changing lumps.
What age do dogs get cancer?
Risk increases with age, but cancer can occur at any age. That is why “new and unusual” changes should be checked regardless of age.
Is there one best screening test?
There is no single perfect screening test for all cancers. Most early detection comes from routine exams, timely evaluation of changes, and appropriate diagnostics like cytology, imaging, and lab work.