Cushing’s Disease Skin Problems in Dogs

If your dog seems to be getting thin skin, random bruises, recurring infections, or wounds that just will not heal, it can feel confusing and scary. As a veterinary assistant, I have seen how often these skin changes are brushed off as “just aging” or “allergies,” when they can actually be part of a bigger hormone picture called Cushing’s disease, also known as hyperadrenocorticism.
Cushing’s is a condition where the body is exposed to too much cortisol over time. Cortisol is not “bad” on its own. Dogs need it for normal stress response and metabolism. The problem is chronic excess, which can affect the skin, immune system, muscles, liver, and more.

In this article, we will stay dermatology-forward and talk about what Cushing’s can do to your dog’s skin, why it happens, and how these clues connect with other classic signs like increased drinking and urination.
Why Cushing’s affects the skin
Your dog’s skin is a busy organ. It is constantly renewing itself, producing oils, growing hair, and acting as a barrier against bacteria and yeast. Chronic high cortisol disrupts many of those normal processes.
- Skin becomes thinner and more fragile because cortisol affects collagen production and skin turnover.
- Immune defenses drop, making infections more likely.
- Hair follicles cycle abnormally, leading to thinning hair or bald patches.
- Blood vessels become more fragile, contributing to bruising and bleeding under the skin.
These changes tend to be gradual. That is why owners often say, “It started small, and then suddenly it was everywhere.”
Thin skin in dogs with Cushing’s
Thin skin is one of the most classic Cushing’s skin findings. You might notice:
- Skin that feels paper-thin or delicate when you pet your dog
- Visible veins or a more “see-through” look, especially on the belly
- Tearing easily during grooming, scratching, or even normal play
Thin skin matters because it increases the risk of injury, infection, and painful sores. If your dog’s skin seems fragile, it is a strong reason to ask your veterinarian whether Cushing’s should be on the rule-out list.

Easy bruising and dark patches
Some dogs with Cushing’s bruise easily. You may find purple or dark spots on the belly, inner thighs, or sides that appear without a clear bump or injury.
There are a few reasons this can happen:
- Fragile blood vessels under thin skin
- Delayed tissue repair after minor trauma
- In some cases, changes in clotting and liver function that can accompany Cushing’s
Not every bruise means Cushing’s. Bruising can also be related to platelet disorders, toxins, trauma, or other illnesses. But when bruising shows up alongside hair loss, infections, and the classic drinking and peeing increase, it is worth investigating quickly.
Comedones and clogged pores
Another common, easy-to-miss Cushing’s clue is the appearance of comedones, basically blackheads. Owners often describe them as “little pepper specks” or “dirt that will not wash off.”
You may notice:
- Blackheads on the belly, chest, or groin
- Clogged pores that are more visible as the coat thins
- Occasional pimples or folliculitis if bacteria take advantage of the plugged follicles
Comedones can show up with other skin conditions too, but when they appear along with thin skin, symmetrical hair loss, and recurrent infections, they are a classic piece of the Cushing’s pattern.
Calcinosis cutis
Calcinosis cutis is a hallmark Cushing’s skin problem that is not as common as hair loss, but when it appears it is a big clue. It happens when calcium deposits form in the skin, often because the skin has been chronically damaged by excess cortisol.
What it can look or feel like:
- Firm plaques or nodules under the skin
- A gritty or sand-like texture when you run your fingers over the area
- White crusts or draining spots if the deposits ulcerate
- Skin that is painful, inflamed, or slow to heal in those patches
Calcinosis cutis can be uncomfortable and it can get infected. If you notice gritty, crusty, or ulcerated patches, especially on the back, flanks, or belly, contact your veterinarian promptly.
Slow healing and recurring sores
“Why is this taking so long to heal?” is a common Cushing’s story. Cortisol can slow wound healing by interfering with inflammation and collagen formation, which are essential steps in repair.
You might notice:
- Scratches that linger for weeks
- Hot spots that keep returning
- Small scabs that repeatedly reopen
- Surgical incisions that heal more slowly than expected
If your dog has a wound that is worsening, oozing, painful, or smells bad, do not wait. Infections can spread faster in dogs whose immune defenses are compromised.
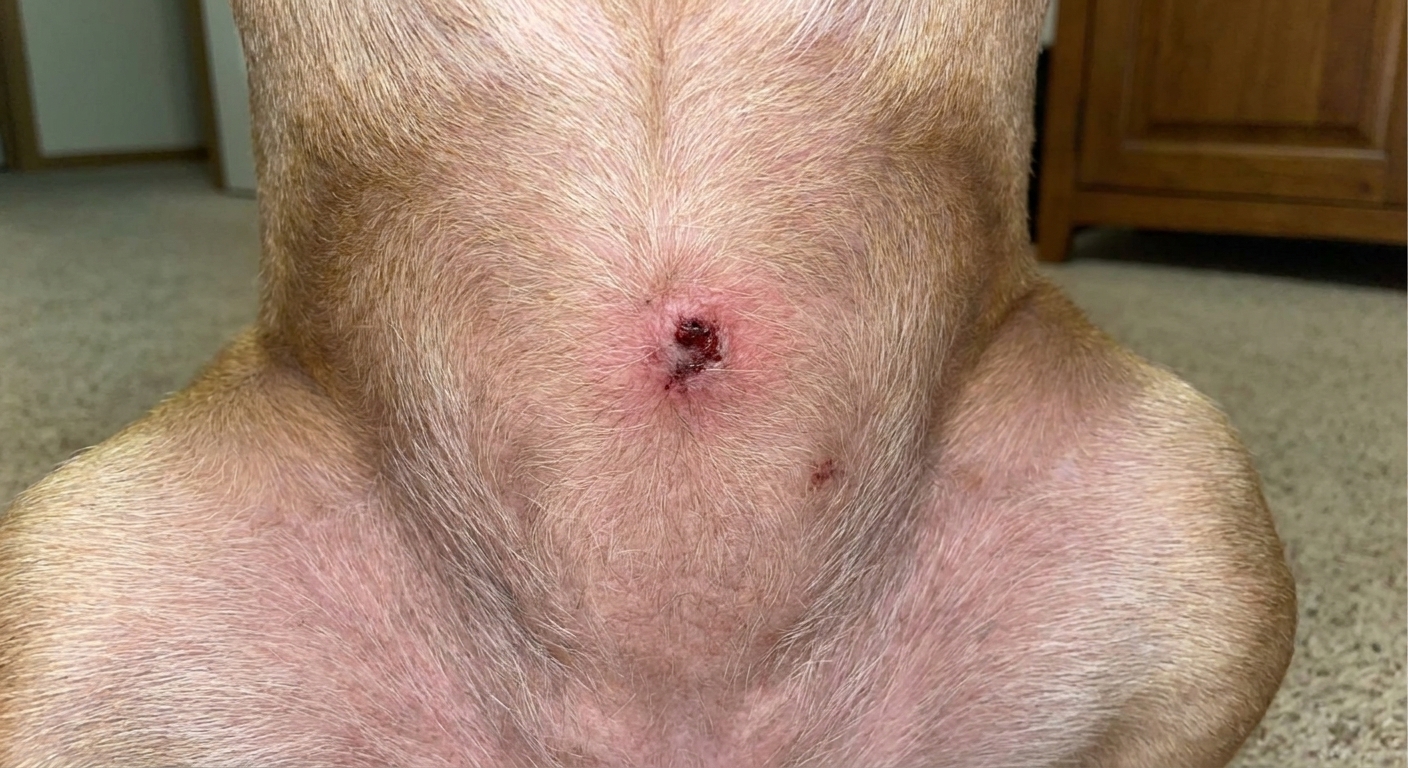
Recurrent skin infections
Cushing’s dogs are prone to recurrent pyoderma (bacterial skin infection) and Malassezia dermatitis (yeast overgrowth). Sometimes it looks like “allergies,” but it does not fully respond to the usual plan or it comes right back.
Signs of infection to watch for
- Redness, pimples, or crusts on the belly or groin
- Musty or “corn chip” odor
- Greasy skin or dandruff
- Itching that suddenly worsens
- Darkened skin from chronic inflammation
These infections often require targeted treatment like topical antiseptic shampoos, prescription medications, and follow-up rechecks. If the underlying cortisol problem is not addressed, infections tend to recur.
Hair loss patterns
Hair changes with Cushing’s are often distinctive. Many dogs develop symmetrical hair loss along the trunk, flanks, and belly, while the head and legs may look relatively normal.
Common coat changes include:
- Thinning coat that feels dry or dull
- Slow regrowth after clipping (for grooming or surgery)
- Hair loss on both sides of the body in a similar pattern
Hair loss can happen for other reasons too, including hypothyroidism, allergies, parasites, or chronic skin infection. The overall pattern and the presence of other Cushing’s signs help your veterinarian decide what to test next.

How skin clues fit the bigger Cushing’s picture
Cushing’s is not just a skin disease, but the skin can be one of the loudest “early warning systems.” When I am helping clients organize symptoms for a vet visit, I encourage them to look for this common cluster:
- Increased thirst (water bowl empties faster)
- Increased urination (more frequent potty trips or accidents)
- Increased appetite (acting constantly hungry)
- Panting more than usual
- Pot-bellied appearance or muscle loss
- Thin skin, bruising, slow healing
- Comedones or gritty plaques (blackheads or calcinosis cutis)
- Recurrent skin or ear infections
Not every dog has every sign, especially early on. But if your dog has skin changes plus increased drinking and urinating, that combination should put Cushing’s high on the discussion list with your veterinarian.
What your veterinarian may do next
Skin symptoms can overlap with many conditions, so diagnosis matters. Your veterinarian may recommend a mix of skin testing and hormone testing.
Skin-focused tests
- Skin cytology (a quick microscope check for bacteria or yeast)
- Skin scraping to look for mites
- Fungal culture if ringworm is a concern
- Culture and sensitivity for stubborn infections
- In some cases, a skin biopsy if calcinosis cutis or another unusual skin disorder is suspected
Cushing’s workup (common components)
- Bloodwork and urinalysis to look for patterns that support Cushing’s and rule out look-alikes
- Urine culture because Cushing’s dogs can get urinary tract infections without obvious symptoms
- Screening and confirmatory hormone tests, often an ACTH stimulation test or a low-dose dexamethasone suppression test, depending on the case
- Abdominal ultrasound in some dogs to evaluate adrenal glands and other organs
If Cushing’s is confirmed, treatment can reduce cortisol effects and many skin issues improve over time. Skin recovery is rarely instant. Hair regrowth and thicker skin often take weeks to months, and infections need active management along the way.
At-home care for fragile skin
While you work with your veterinarian on diagnosis and treatment, small practical steps can make your dog more comfortable and help prevent complications.
Gentle handling and safer routines
- Use a harness instead of a neck collar if your dog’s skin bruises easily.
- Choose soft bedding and wash it regularly to reduce bacteria and yeast buildup.
- Trim nails to reduce self-scratching injuries.
- Avoid harsh grooming and ask your groomer to be extra gentle with clipping and brushing.
Skin hygiene that supports treatment
- Use only the medicated shampoo or wipes your veterinarian recommends. Over-the-counter products can irritate thin skin or worsen dryness.
- Keep skin folds, belly, and groin areas clean and dry, especially after outdoor time.
- Do not apply human antibiotic ointments unless your veterinarian approves. Dogs often lick them, and some ingredients are not a good fit.
Nutrition and weight support
Many dogs with Cushing’s gain weight or lose muscle. A nutrition plan that supports lean body condition can reduce strain on the skin and immune system. If you are interested in adding fresh, whole foods, do it slowly and ask your veterinarian for guidance, especially if your dog also has other conditions.
When to seek urgent care
Skin changes can become emergencies when infection or poor healing gets out of control. Contact your veterinarian promptly if you notice:
- Rapidly spreading redness, swelling, or pain
- Pus, strong odor, or oozing from the skin
- Fever, lethargy, or refusal to eat
- Large bruises, bruises that keep expanding, or bleeding
- A wound that is open and not closing
- Gritty plaques, draining tracts, or painful crusting that could fit calcinosis cutis
If your dog has thin skin plus increased drinking and urinating, you are not overreacting by asking about Cushing’s. Catching it earlier can mean fewer infections, better comfort, and a smoother treatment path.
Quick symptom tracker
It helps your veterinarian if you come in with specific examples. You can jot down:
- How many times you fill the water bowl per day, or how often your dog asks to go out
- Where the hair loss is located (belly, sides, tail, neck)
- Whether you have noticed blackheads on the belly or groin
- Whether any patches feel gritty, crusty, or firm (possible calcinosis cutis)
- How many skin infections or ear infections happened in the last 6 to 12 months
- Photos of bruises, scabs, or wounds with dates
- Any medications, including steroids (prednisone, dexamethasone, steroid ear drops), since steroid exposure can cause Cushing’s-like effects
That level of detail can shorten the time to answers, and it helps your vet choose the most appropriate tests.
