Learn how to feed a cat with cancer: high-protein wet food, calorie-dense options for weight loss, safe omega-3 support, foods to avoid, and appetite tips to...
Article
•
Designer Mixes
Cat Liver Issues Handbook

Shari Shidate
Designer Mixes contributor
If your cat has been diagnosed with “elevated liver enzymes” or “liver disease,” you are not alone, and you are not powerless. As a veterinary assistant in Frisco, Texas, I have seen how scary liver issues can feel at first. The good news is that many liver problems are treatable, and supportive care at home can make a real difference.
This handbook walks you through what the liver does, why cats get liver issues, what symptoms to watch for, which tests your veterinarian may recommend, and the practical steps that support recovery and long-term wellness.

What the liver does
The liver is your cat’s behind-the-scenes powerhouse. It is involved in hundreds of jobs, including:
- Filtering toxins from the blood
- Processing nutrients from food
- Making bile to help digest fats
- Storing vitamins and energy (like glycogen)
- Producing proteins needed for normal blood clotting
Cats can look “fine” until the liver is significantly stressed, which is why early clues matter and why routine lab work can be so helpful.
Common liver problems
Hepatic lipidosis (fatty liver)
This is one of the most common and urgent liver conditions in cats. It often happens when a cat stops eating. The body starts mobilizing fat for energy, and the liver gets overwhelmed processing it.
Key point: for cats, not eating is not something to ignore. In some cats, especially overweight cats, 24 to 72 hours of very low intake can become dangerous.
Cholangitis and cholangiohepatitis
These terms describe inflammation in the bile ducts and sometimes the liver itself. It can be related to infection, immune-mediated inflammation, or conditions involving the intestines and pancreas.
Toxin exposure
The liver processes many substances, so certain medications, household chemicals, toxic plants, and concentrated essential oils can cause serious toxicity in cats. That toxicity may involve the liver, but it can also affect the nervous system, breathing, and the gastrointestinal tract.
Hepatitis and chronic liver disease
Some cats develop ongoing inflammation and scarring over time. Management may involve diet changes, supplements, and ongoing lab monitoring.
Gallbladder and bile flow issues
Problems with bile flow can lead to jaundice and digestive upset. Your veterinarian may evaluate the gallbladder closely on ultrasound.
Portosystemic shunt (less common)
This is an abnormal blood vessel that routes blood around the liver instead of through it. It can be congenital (present at birth) or acquired. It is less common, but important to identify because treatment choices differ.

Signs to watch for
Some signs are obvious, and others are subtle. Call your veterinarian promptly if you notice:
- Not eating or eating much less than normal
- Vomiting or frequent nausea (lip smacking, drooling)
- Weight loss or muscle loss
- Lethargy, hiding, or reduced grooming
- Diarrhea or pale stools
- Yellow tint to the whites of the eyes, gums, or skin (jaundice)
- Increased thirst or urination
- Behavior changes such as disorientation, staring, or seeming “spacey” (can occur with hepatic encephalopathy)
- Bruising or bleeding more easily (clotting issues)
Urgent red flags: jaundice, repeated vomiting, collapse, extreme lethargy, trouble breathing, or sudden neurologic signs (disorientation, tremors, seizures).
About not eating: if your cat has eaten little or nothing for about 24 hours, contact your veterinary team the same day if you can. Go sooner for kittens, seniors, medically fragile cats, and overweight cats.
High liver enzymes explained
“High liver enzymes” is not a diagnosis. It is a clue. Enzymes can rise for different reasons, such as inflammation, bile backup, stress on liver cells, pancreatitis, intestinal disease, endocrine issues, or toxin exposure.
It also helps to know this difference:
- Liver enzymes (ALT, AST, ALP, GGT) suggest irritation or injury, but they do not automatically mean liver failure.
- Liver function markers (bilirubin, albumin, glucose, cholesterol, bile acids, and clotting tests) help your vet assess how well the liver is actually doing its jobs.
In cats, the lab values your vet may discuss include:
- ALT: often rises with liver cell injury
- AST: can rise with liver injury or muscle injury
- ALP: cats tend to show smaller ALP increases than dogs, and because ALP has a shorter half-life in cats, even modest elevations can be meaningful depending on the whole picture
- GGT: another bile-associated enzyme; patterns can help narrow causes
- Bilirubin: often elevated with jaundice and bile flow problems
- Albumin, glucose, cholesterol: can change with liver function issues
- Clotting tests (PT/aPTT): may be recommended if liver function is compromised
Because numbers do not tell the whole story, vets combine lab work with your cat’s symptoms, exam, and imaging.
Tests your vet may do
Your veterinarian will tailor testing to your cat, but a typical workup may include:
- History and physical exam (including weight trends and hydration)
- Complete blood count and chemistry (liver enzymes, bilirubin, proteins)
- Urinalysis (hydration status and overall clues)
- Thyroid testing in older cats, since hyperthyroidism can affect weight and lab values
- FeLV/FIV testing when indicated
- Abdominal ultrasound to evaluate liver texture, bile ducts, gallbladder, pancreas, and intestines
- Bile acids test in some cases to evaluate liver function and blood flow patterns
- Fine needle aspirate or biopsy when the cause is unclear or when cancer or specific inflammatory diseases are suspected
If your vet recommends an ultrasound, it is often a very helpful next step because it can reveal bile duct disease, gallbladder issues, masses, or signs of pancreatitis and inflammatory bowel disease that can travel together in cats.
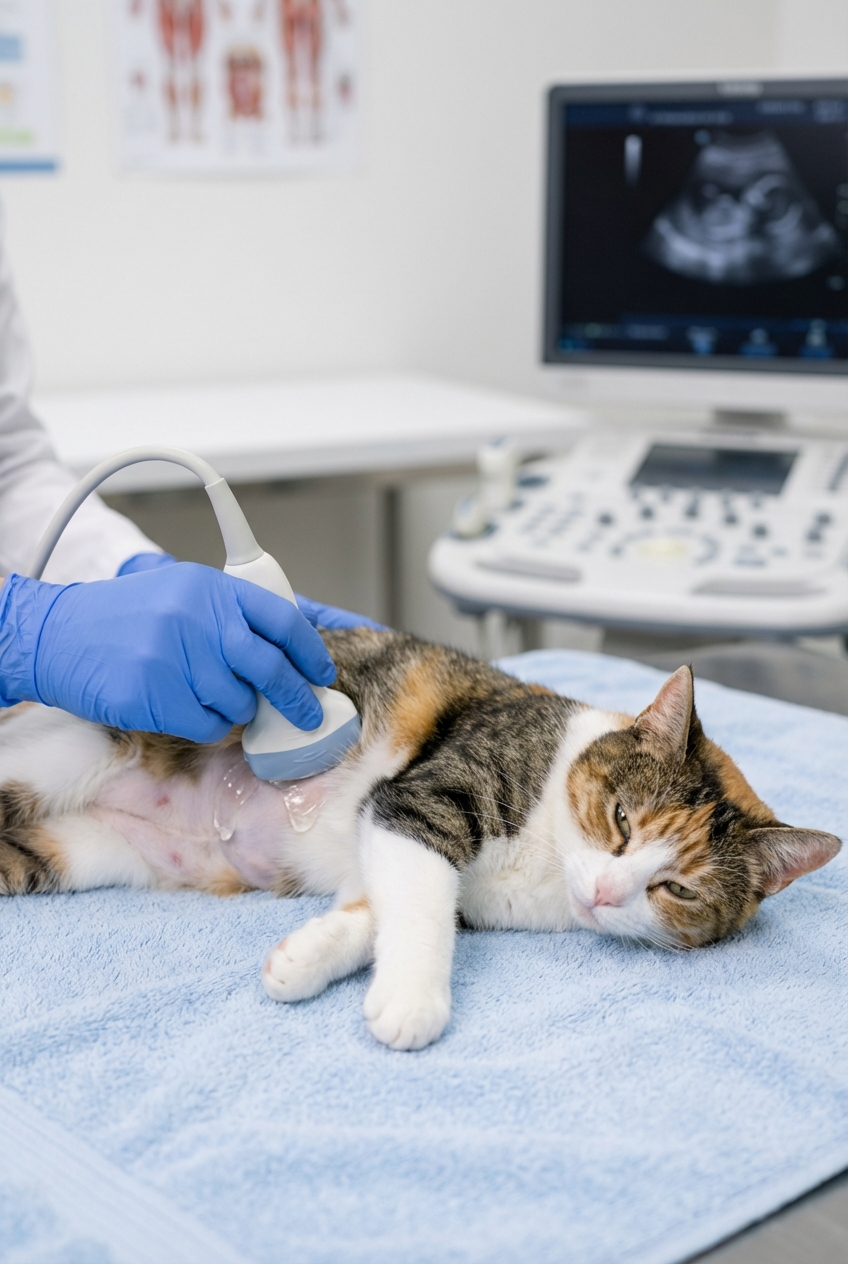
Nutrition is treatment
For many feline liver problems, especially hepatic lipidosis, calories and protein are medicine. The liver cannot recover well if your cat is not getting enough nutrition.
Do not wait it out
If your cat is not eating, call your vet quickly. In some cats, a short period of poor intake can spiral into fatty liver disease, particularly if your cat is overweight or already sick.
What to feed
Your veterinarian may recommend a prescription liver diet in some cases, but the right choice depends on the diagnosis. In many liver conditions, cats still need:
- A highly palatable diet they will reliably eat
- High-quality protein to maintain muscle and support healing
- Adequate calories to prevent fat mobilization to the liver
- Consistent routines that reduce stress around meals
If hepatic encephalopathy is present, your vet may adjust protein type and amount. Do not restrict protein on your own.
Feeding tips
- Warm wet food slightly to increase aroma.
- Offer small meals 4 to 6 times daily.
- Try different textures like pate, shreds, or mousse.
- Use a quiet feeding area away from other pets.
- Track intake so you know whether your cat is improving.
If your cat cannot or will not eat enough, your vet may prescribe appetite stimulants, anti-nausea medication, or discuss assisted feeding. Feeding tubes can sound intimidating, but they can be life-saving and often reduce stress because you can deliver consistent nutrition without forcing your cat to eat.
Medications and supplements
Always follow your veterinarian’s plan and dosing. Liver patients are not the place for guesswork.
Nausea and appetite support
- Anti-nausea medications can help cats feel well enough to eat.
- Appetite stimulants may be used short term.
- Fluids may be needed if dehydration is present.
Common supplements (varying evidence)
- SAMe (S-adenosylmethionine): commonly used to support antioxidant pathways in the liver.
- Silybin or milk thistle extracts: evidence is mixed and formulation-dependent, but some veterinarians use them as supportive care.
- Vitamin B complex: cats with liver disease may have increased needs.
- Vitamin K: used when clotting concerns are identified.
Supplement quality matters. Ask your veterinarian which brands and forms they trust, and think of supplements as support, not a cure.
Targeted therapies
If cholangitis or infection is suspected, antibiotics may be prescribed. Some inflammatory conditions require immunosuppressive medications. If your cat has an underlying issue like pancreatitis, intestinal disease, or hyperthyroidism, treating the root cause is a big part of liver recovery.
If your cat shows signs of hepatic encephalopathy, your veterinarian may use medications such as lactulose and sometimes antibiotics to reduce toxin buildup that can affect the brain.
Home monitoring
One of the most powerful things you can do at home is collect simple, consistent information. Here is what I recommend tracking:
- Appetite: how much is eaten in 24 hours
- Water intake: increased or decreased
- Vomiting: frequency and what it looks like
- Stool: color, consistency, frequency
- Energy: normal, reduced, or withdrawn
- Weight: weekly weigh-ins can catch problems early
- Jaundice: check gums and whites of the eyes in good light
If something feels off, trust that instinct and call your veterinary team. Liver cases can change quickly, and early adjustments often prevent hospitalization.

What not to do
- Do not give human pain medications. Acetaminophen (Tylenol), ibuprofen (Advil), and naproxen (Aleve) can be dangerous or fatal to cats.
- Do not use essential oils around your cat without veterinary guidance. Cats are particularly sensitive, and exposure can cause serious illness.
- Do not force fasting. Cats are not small dogs. Not eating can trigger fatty liver disease.
- Do not change diets repeatedly in panic. Make changes with a plan so you can tell what helps.
- Do not stop prescribed meds early because your cat “seems better.”
Prevention and long-term care
Not all liver disease is preventable, but you can lower the risk and support long-term health.
Keep eating consistent
Any appetite change deserves attention. For multi-cat homes, separate feeding can reduce stress and ensure each cat is eating enough.
Support a healthy weight
Overweight cats are at higher risk for hepatic lipidosis if they stop eating. Work with your vet on safe weight loss. Cats should not crash diet.
Vaccines and parasite prevention
These steps support overall resilience and reduce the odds of infections or parasite burdens that can complicate chronic illness and recovery.
Toxin-proof your home
- Store medications and chemicals securely.
- Ask your vet before using any flea products not labeled for cats.
- Be cautious with lilies and other toxic plants in the home. If your cat may have chewed a lily, treat it as urgent and call a veterinarian or poison hotline right away.
Schedule rechecks
Liver issues usually require follow-up lab work. Recheck timelines vary, but many cases benefit from repeat testing in a few weeks, then spacing out as values improve.
Prognosis basics
Outcomes depend on the cause and how quickly treatment starts. Many cats with hepatic lipidosis can recover well with aggressive nutritional support and close monitoring. Chronic inflammatory disease may be manageable long-term with the right plan. Advanced scarring or cancer can be more unpredictable, so your veterinarian will help you set realistic goals and next steps.
Questions to ask
- What is the most likely cause of my cat’s liver changes?
- Is this primarily a liver disease, or could it be secondary to pancreatitis or intestinal disease?
- Which results suggest enzyme leakage versus reduced liver function?
- Does my cat need an ultrasound, and what are you looking for?
- How many calories should my cat eat per day right now?
- Should we use an appetite stimulant or anti-nausea medication?
- Which supplements do you recommend, and why?
- When do we recheck lab work, and which values matter most?
- What signs mean I should go to an emergency clinic?
When to get urgent care
Please seek urgent veterinary care if your cat has:
- Yellow gums or eyes
- Repeated vomiting or cannot keep food down
- Severe lethargy, collapse, or trouble breathing
- Disorientation, tremors, seizures, or sudden behavior changes
- Evidence of bleeding or bruising
- Eaten little or nothing for about 24 hours, or sooner if your cat is a kitten, senior, overweight, or has other illnesses
If you take only one thing from this guide, let it be this: in cats, appetite is a vital sign. When a cat is not eating, the liver often gets dragged into the story.
Closing
Liver issues can be serious, but many cats do very well with timely care, consistent nutrition, and a plan you can actually follow at home. If you are feeling overwhelmed, start with the basics: keep your cat eating, keep follow-up appointments, and communicate openly with your veterinary team. You are doing the right thing by learning, and your cat is lucky to have you.



