Dog UTI symptoms can mimic stones or other issues. Learn the full treatment plan: urinalysis and culture, correct antibiotics, pain control, hydration, home ...
Article
•
Designer Mixes
Blood in Dog’s Urine

Shari Shidate
Designer Mixes contributor

Seeing blood in your dog’s urine can feel scary, and I get it. As a veterinary assistant in Frisco, Texas, I have watched many loving families walk in with the same question: “Is this an emergency?” Sometimes it is. Sometimes it is not. Either way, blood in the urine is a sign we should take seriously and investigate promptly.
Quick note: This guide is for education and is not a substitute for veterinary care. If you are worried, call your veterinarian or an emergency clinic.
This handbook will help you understand what blood in urine can look like, the most common causes, what to do right now at home, what your veterinarian may recommend, and how to support recovery safely.
What “blood in urine” means
The medical term for blood in the urine is hematuria. It can be obvious, or it can be so subtle it only shows up on a urine test.
Visible vs. microscopic
- Gross hematuria: you can see red, pink, orange, brown, or tea-colored urine.
- Microscopic hematuria: urine looks normal, but red blood cells are found under a microscope.
Look-alikes
Not every red or dark tint is true “blood in the bladder.” A few common look-alikes:
- Food dyes or pigments: certain treats or foods can shift urine color.
- Medication effects: some medications and supplements can change urine color.
- Very dark brown or cola-colored urine: can be related to pigment issues (like hemoglobin or muscle pigment) and still needs prompt evaluation.
- Blood from another source: heat cycle bleeding, skin irritation, or rectal bleeding can sometimes look like urinary bleeding when it mixes in the hair or on the ground.
Important note: do not assume. When in doubt, test it.
Emergency or not?
If your dog has blood in the urine, I recommend calling your veterinarian the same day. And if any of the signs below are present, treat it as urgent.
Go to an emergency vet now
- Straining with little or no urine produced, or repeated attempts that only produce drops
- Severe pain, crying out, or a tight and painful belly
- Vomiting, collapse, extreme lethargy, pale gums, or weakness
- Known toxin exposure (rat poison, antifreeze, human medications, illicit substances)
- Heavy bleeding or blood clots
- Recent trauma (hit by car, fall, dog fight)
See your regular vet in 24 to 48 hours
- Pink-tinged urine but your dog is eating, drinking, and acting mostly normal
- More frequent urination or mild discomfort
- Licking the vulva or penis more than usual
- Accidents in the house in a previously house-trained dog
What “straining” can look like
- Straining: posturing to pee for a long time, looking uncomfortable, and producing little to no urine.
- Frequent small pees: many quick trips outside with small amounts each time. This is often seen with bladder irritation or infection, even when a dog is not blocked.
If your dog cannot pass urine, do not wait overnight. Urinary blockage, especially in male dogs, can become life-threatening fast.
Common causes
Blood can come from the kidneys, ureters, bladder, prostate (in males), urethra, or even the external genital area. Here are the most common causes we see in practice.
UTI and bladder inflammation
UTIs and sterile cystitis (inflammation without infection) can cause blood, frequent urination, urgency, and discomfort. Female dogs may be at higher risk due to anatomy, but males can absolutely get UTIs too. Other risk factors can include skin folds around the vulva, endocrine disease (like diabetes or Cushing’s), steroids or other immune-suppressing medications, and underlying bladder issues.
Bladder stones or crystals
Stones can irritate the bladder lining and cause bleeding. Some stones increase the risk of blockage, particularly in male dogs. Diet, urine pH, hydration, infections, and breed predispositions can all play roles.
Prostate disease (male dogs)
Intact male dogs can develop benign prostatic enlargement, prostatitis (infection), cysts, or tumors, which may cause bloody urine, straining, or blood dripping from the penis.
Kidney disease or infection
Kidney issues may cause blood in urine, changes in drinking and urination, decreased appetite, weight loss, or vomiting. Not every kidney case bleeds, but it is on the list.
Toxins and clotting problems
Rat bait (anticoagulant rodenticide) is a classic cause of internal bleeding. Certain medications, liver disease, tick-borne illnesses, and immune-mediated conditions can also affect clotting and trigger urinary bleeding.
Tumors or polyps
Some cancers, including transitional cell carcinoma, can cause intermittent blood in urine, straining, and frequent small pees. Older dogs are at higher risk, and early investigation matters.
Trauma
Falls, getting stepped on, rough play, or being hit by a car can injure the urinary tract. Even if your dog “seems fine,” internal injury is possible.
Heat cycle blood (not urine)
In unspayed females, vaginal bleeding from a heat cycle can be mistaken for blood in urine. Your vet can help you confirm the source.

What to do at home
You do not need to panic, but you do need a plan. Your goal is to keep your dog safe and gather helpful information for your vet.
1) Check overall condition
- Is your dog bright and responsive or lethargic?
- Any vomiting, diarrhea, weakness, or pale gums?
- Is your dog able to urinate a normal stream?
2) Offer water and take leash walks
Hydration supports the urinary tract. Do not force water. If your dog will drink, let them drink freely. Take them out on leash so you can observe the urine stream and color.
3) Collect a urine sample if you can
A fresh sample can be extremely helpful. Use a clean, dry container. Bring it to your clinic within 4 to 6 hours if possible. If you cannot get in right away, refrigerate it and tell the clinic when it was collected, since cells and crystals can change over time.
4) Take a photo or video
It may feel strange, but a quick photo of the urine color or a short video of your dog straining can help your veterinarian make faster decisions.
5) Avoid common mistakes
- Do not give human pain meds like ibuprofen, naproxen, or aspirin unless your veterinarian specifically directs it. These can be dangerous for dogs.
- Do not give leftover pet pain meds either (including dog NSAIDs like carprofen or meloxicam) unless your veterinarian tells you to, since the wrong drug or dose can cause serious harm.
- Do not start leftover antibiotics. The wrong antibiotic or wrong duration can mask symptoms and make infections harder to treat.
- Do not restrict water. Concentrated urine can worsen irritation.
- If you suspect a blockage, do not “wait it out” and do not attempt to express the bladder or catheterize at home. Go in.
How vets diagnose it
Most cases start with basic tests that give us a lot of information quickly. Your vet will recommend what fits your dog’s symptoms, age, and risk factors.
History and exam
- When did it start? Is it every time or intermittent?
- Any accidents in the house, increased frequency, or straining?
- Diet, treats, supplements, and any new meds?
- For males: prostate check if appropriate.
Urinalysis (UA)
A urinalysis checks for red and white blood cells, bacteria, crystals, pH, protein, and concentration. This is one of the most important tests for urinary issues.
Urine culture
If infection is suspected, a culture confirms the bacteria and identifies which antibiotics work best. This matters for recurrent UTIs and for dogs with risk factors like diabetes or Cushing’s.
Bloodwork
Blood tests can assess kidney function, hydration status, infection markers, anemia, and clotting concerns.
Imaging
- X-rays: can identify many bladder stones and evaluate anatomy. Some stone types can be harder to see on X-ray, so a normal X-ray does not always rule stones out.
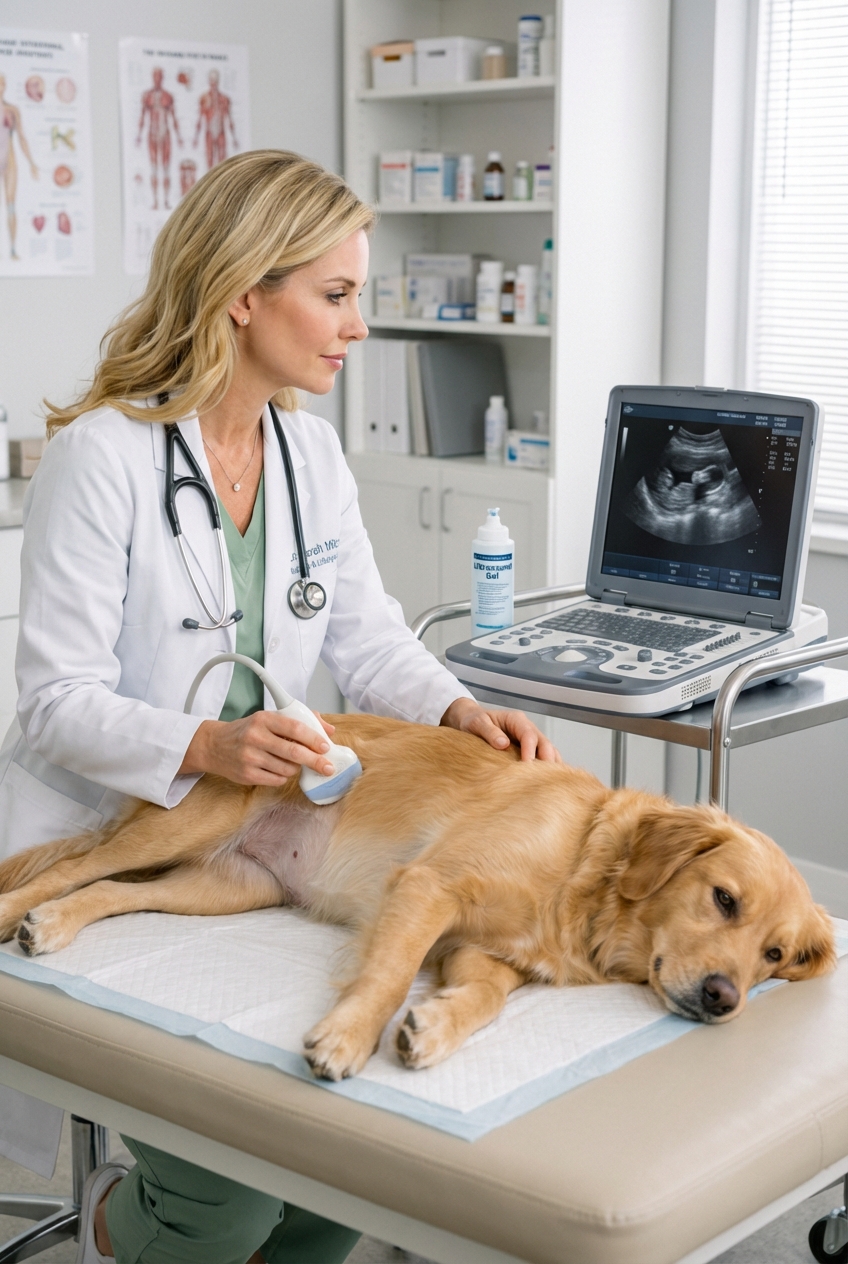
- Ultrasound: excellent for bladder wall changes, tumors, prostate evaluation, and some stones.
Treatment options
Treatment depends on the cause. The goal is to address the underlying issue, relieve discomfort, and prevent recurrence.
UTIs and bladder inflammation
- Antibiotics if infection is confirmed or strongly suspected
- Pain relief and anti-inflammatory medication prescribed by your veterinarian
- Follow-up urinalysis or culture to confirm the infection cleared, especially for repeat cases
Bladder stones
- Prescription dissolution diets for certain stone types, when appropriate
- Surgery or other removal methods for stones that cannot dissolve or that are causing obstruction
- Long-term prevention plan based on stone analysis and urine testing
Urinary blockage (emergency)
- Catheterization under sedation or anesthesia
- IV fluids and electrolyte monitoring
- Medications and a strict follow-up plan
Toxin exposure or clotting disorders
- Antidotes when available (for example, vitamin K1 for certain rat poisons)
- Hospitalization, supportive care, and coagulation testing
Tumors or complex cases
Your vet may recommend referral to internal medicine, oncology, or surgery. Early diagnostics can expand your options.
Food and recovery support
Food and hydration do not replace medical care, but they can support the urinary tract and overall healing once your veterinarian has identified the cause.
Hydration helps
- Offer fresh water in multiple locations.
- Consider adding water or low-sodium broth to meals if your vet approves.
- Wet food can increase water intake compared to kibble alone.
Do not switch diets blindly
Different stone types require different strategies. Some stones dissolve with targeted diets, while others do not. Switching diets without knowing the stone type can accidentally make the urine environment more favorable for stone growth.
Ask before supplements
Some supplements may help certain dogs, but they can also interfere with medications or alter urine pH. Common examples people ask about include cranberry products, D-mannose, probiotics, omega-3s, and urinary support blends. These should be individualized.
Prevention
Not every case is preventable, but many are. These habits can make a real difference, especially for dogs prone to UTIs or crystals.
- Regular potty breaks: frequent opportunities to urinate may help reduce discomfort and can be especially helpful for dogs with irritated bladders.
- Hydration routines: clean bowls daily, refresh water often.
- Weight management: obesity is linked with inflammation and health complications.
- Vet-guided nutrition: especially if your dog has had stones or recurring urinary issues.
- Follow-up testing: repeat urinalysis or culture when recommended, even if symptoms improved.

Common questions
Can it clear up on its own?
It can, but that does not mean the underlying cause is harmless. UTIs, stones, and even more serious issues can have waxing-and-waning symptoms. It is safer to test than to guess.
My dog is acting normal. Do I still go in?
Yes, schedule an appointment soon. “Acting normal” is common early in urinary problems. Dogs are very good at hiding discomfort until it becomes intense.
Is it always a UTI?
No. UTIs are common, but stones, prostate issues, inflammation, toxins, trauma, and tumors are also on the list. That is why urinalysis and sometimes imaging are so important.
When in doubt, call
If you are staring at a pink puddle in the yard and your mind is racing, take a breath. Then take action. Call your veterinarian, describe what you are seeing, and ask if they want a urine sample brought in. Prompt care can prevent bigger problems and help your dog feel better faster.
Quick recap: If your dog cannot urinate or is straining hard, treat it as an emergency. If your dog is urinating normally but you see blood, schedule a vet visit as soon as possible and bring a fresh urine sample if you can.
References
- Merck Veterinary Manual: “Hematuria in Dogs” and related urinary tract disorder pages (accessed 2026-02-18)
- American College of Veterinary Internal Medicine (ACVIM): urolithiasis and urinary disease resources and consensus guidance (accessed 2026-02-18)
- American Veterinary Medical Association (AVMA): pet toxin safety and emergency care guidance (accessed 2026-02-18)



