Blastomycosis in Dogs

If your dog loves hiking trails, chasing ducks at the lake, or sniffing every muddy riverbank, you are not alone. I live in Texas and work with a lot of active, outdoorsy pups, and one illness I always want families to know about is blastomycosis. It is a fungal infection that dogs usually pick up by breathing in spores from the environment, and it can move beyond the lungs to the skin, eyes, bones, or even the brain.
Quick Texas note: blastomycosis is generally less common in Texas than in the Great Lakes and river-valley regions, but it can happen. In East Texas, I also keep fungal disease on my radar because it can be a crossover zone where blastomycosis and histoplasmosis both show up, and travel to endemic regions absolutely counts.
The tricky part is that blastomycosis often starts looking like something much more common, like kennel cough or bacterial pneumonia. Knowing the early signs and the higher-risk regions can help you get to the right tests faster.

What is blastomycosis?
Blastomycosis is caused by a fungus called Blastomyces (most commonly Blastomyces dermatitidis in North America). The fungus lives in the environment, especially in moist soil with decaying vegetation. Dogs become infected primarily by inhalation, not by eating something or catching it from another dog.
Once inhaled, spores can cause a lung infection. In some dogs, the organism spreads through the bloodstream or lymphatic system, leading to a systemic infection.
Is it contagious to other dogs or people?
In general, blastomycosis is not considered contagious from dog to dog or dog to human because the usual route is inhaling spores from the environment. There are rare case reports of transmission through bites or direct contact with draining skin lesions, but that is unusual.
Practical takeaway: if your dog has a draining lesion and blastomycosis is being considered, use gloves if you have them, wash hands well after handling the area, and keep kids from touching drainage. In everyday life, think of blastomycosis as an environmental exposure risk, not a “catch it from your pet” disease. (Cats and people can get blastomycosis too, but usually from the same environment, not from the dog.)
Where is blastomycosis most common?
Blastomycosis is considered endemic in certain parts of North America. Risk is highest where there is wet soil, wooded areas, and waterways.
Common higher-risk regions (North America)
- Ohio and Mississippi River valleys
- Great Lakes region (Great Lakes states and provinces, especially around rivers and lakes)
- Upper Midwest, with especially high incidence reported in Wisconsin and Minnesota
- Parts of the Southeast
- Parts of Canada, including some Great Lakes and major-waterway areas
Endemic does not mean exclusive. Dogs can be diagnosed outside these classic areas. Travel history matters. If your dog visited a river cabin for a weekend two months ago, mention it.
Outdoor clues that raise suspicion
- Swimming, retrieving, or running along rivers, lakes, or marshy trails
- Digging or sniffing in damp soil
- Spending time in wooded areas with rotting leaves or decaying vegetation
- Hunting dogs or farm dogs with frequent soil exposure

Signs of blastomycosis in dogs
Symptoms vary a lot depending on whether the infection is mostly in the lungs or has spread elsewhere. Some dogs get sick quickly. Others have vague, slow-building symptoms that come and go.
Respiratory signs (lungs)
- Cough (may be persistent or mild)
- Fast breathing or increased effort to breathe
- Exercise intolerance, tiring on walks
- Fever
- Lethargy
- Decreased appetite and weight loss
Many dogs are first treated for bacterial pneumonia. If antibiotics do not help, your vet may widen the search and consider fungal disease.
Skin and lymph node signs
- Skin sores or nodules, sometimes with draining tracts
- Crusting lesions, especially on the face, nose, or legs
- Enlarged lymph nodes
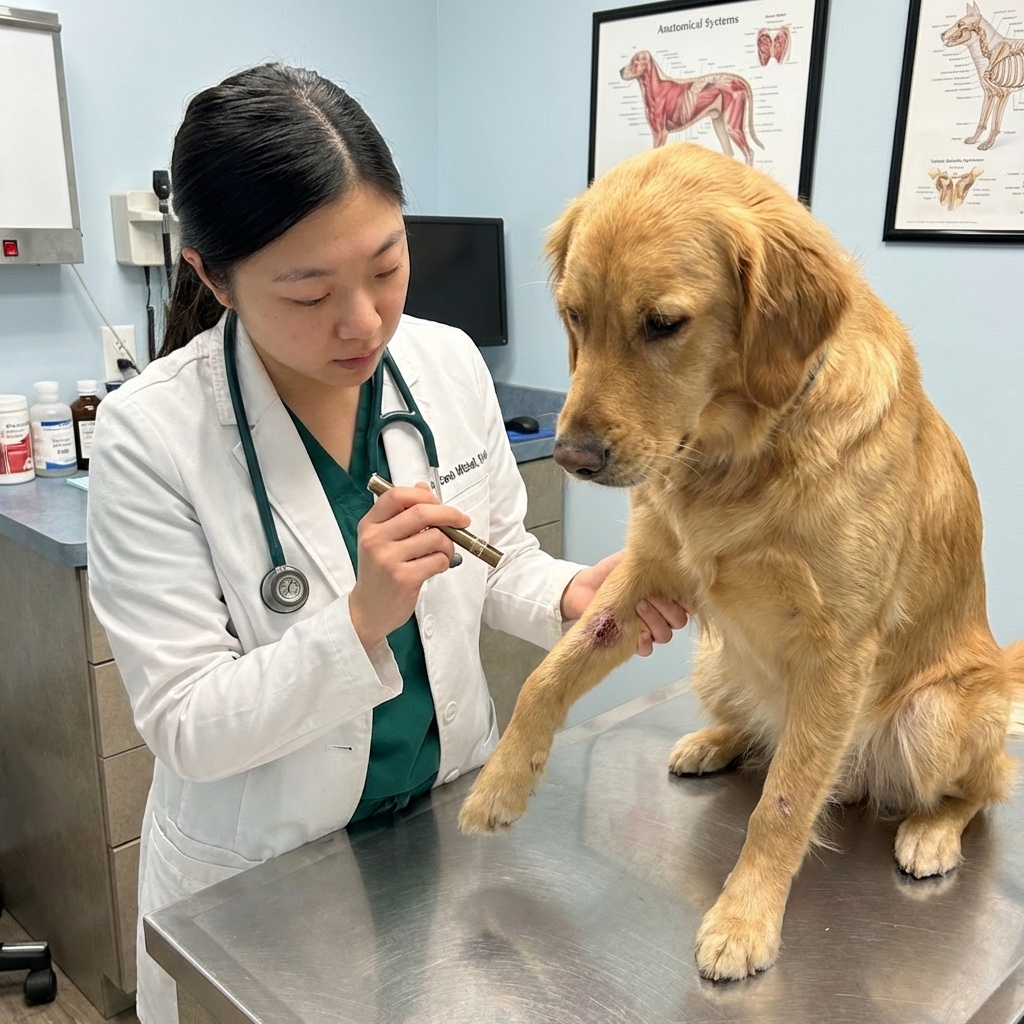
Eye signs (urgent)
Blastomycosis can involve the eyes and may lead to permanent damage.
- Red, painful eye
- Squinting, light sensitivity
- Cloudy eye or visible inflammation inside the eye
- Sudden vision loss
If you notice eye pain or sudden vision changes, treat it as same-day urgent. Early care can make a real difference.
Bone and joint signs
- Lameness that shifts from leg to leg
- Swollen joints
- Pain when walking or jumping
Neurologic signs (less common, more serious)
- Seizures
- Head tilt, stumbling
- Behavior changes
My rule of thumb as a veterinary assistant: If a dog has a cough plus any “extra” system involved like skin bumps, eye inflammation, unexplained lameness, or weight loss, it is worth asking your vet, “Could this be fungal?”
Why blastomycosis is misdiagnosed
Blastomycosis is a master of disguise. Early on, it can look like:
- Kennel cough or chronic bronchitis
- Bacterial pneumonia
- Allergies or hot spots (when skin lesions are present)
- Immune-mediated disease
- Cancer (because lung patterns and weight loss can look similar)
Another pitfall is timing. Symptoms may show up weeks to months after exposure, so families do not always connect the dots to that trip to the cabin or the new favorite creek spot.
What vets test for
Because blastomycosis can affect multiple organs, vets often combine history, imaging, and lab testing to get a confident diagnosis and start treatment quickly.
1) Physical exam and history
Your vet will ask about travel, outdoor access, hunting, swimming, and where your dog spends time. This is not small talk. It helps determine if fungal testing is worth prioritizing.
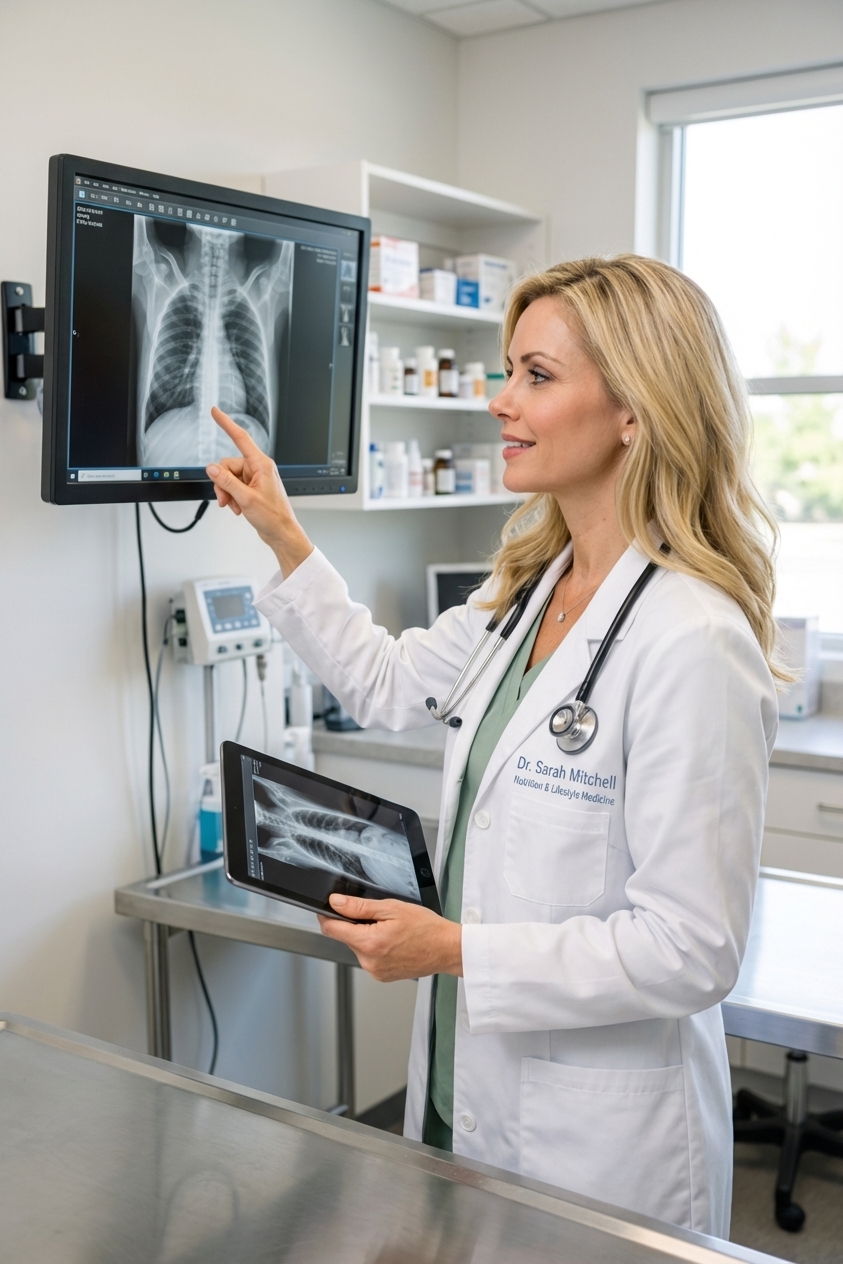
2) Chest X-rays (radiographs)
Chest X-rays can show lung changes consistent with fungal pneumonia. These findings are not always specific, but they help your vet gauge severity and decide next steps.
3) Antigen testing (urine and sometimes blood)
Many clinics use a Blastomyces antigen test, often run on urine (and sometimes serum). It can be very helpful for screening and monitoring response to treatment.
Important nuance: Antigen tests can sometimes cross-react with other fungal diseases (for example histoplasmosis). Also, a negative antigen test does not always rule it out, especially early in disease or in more localized infections. That is why results are interpreted alongside clinical signs, geography, and other tests.
4) Cytology (looking for the organism under the microscope)
This is one of the most direct ways to diagnose blastomycosis. A veterinarian may collect samples from:
- Skin lesions or draining tracts
- Enlarged lymph nodes (fine needle aspirate)
- Airway samples in some cases (with appropriate precautions)
Under the microscope, Blastomyces can have a characteristic appearance, which helps confirm the diagnosis.
5) Other tests your vet may use
- Eye exam (sometimes by a veterinary ophthalmologist) if eye involvement is suspected
- Bloodwork to assess inflammation and organ function before antifungal therapy and for monitoring
- Urinalysis to evaluate overall health and support medication planning
- Biopsy and histopathology if a tissue diagnosis is needed
- PCR in some settings
- Fungal culture is sometimes considered, but it can pose exposure risk and is not always pursued
- Advanced imaging (CT, ultrasound) if the case is complicated
Why early care matters
Blastomycosis is treatable, but it is not something to “wait out.” Dogs can deteriorate quickly, especially when the lungs are heavily affected.
Early diagnosis matters because:
- It reduces the time a dog spends on antibiotics that will not help a fungus.
- It helps prevent further spread to eyes, bones, and the nervous system.
- It gives your vet a chance to start antifungal therapy before breathing becomes critical.
Treatment overview
Treatment is usually long-term antifungal medication. For many dogs, “long-term” means at least 3 to 6 months, and it is common to continue treatment for a period after a dog is doing well clinically and follow-up testing has improved. Your veterinarian will tailor the plan to your dog’s organs involved, severity, and test trends.
The most common first-line medication many owners hear about is itraconazole. In more severe cases, especially with heavy lung involvement, veterinarians may use amphotericin B (often in a hospital setting) as part of the initial approach.
What to expect during treatment
- Recheck visits to make sure breathing, appetite, weight, and energy are moving in the right direction
- Repeat antigen testing (often urine) or other monitoring to track response and help guide duration
- Monitoring bloodwork, because some antifungals can affect the liver and some dogs get GI upset
- Patience and consistency, since missed doses can set progress back
Do not start or stop antifungals without your vet’s guidance. Dose and duration matter, and monitoring helps keep treatment as safe as possible.
Prognosis basics
Outcomes vary. Dogs tend to do better when the disease is caught earlier and lung involvement is not severe. Eye involvement and nervous system involvement can be more complicated, and vision loss can be permanent even with treatment. Relapses can happen, which is one reason follow-up testing and rechecks matter.
When to call your vet
Please seek veterinary care promptly if your dog has any of the following, especially with a history of outdoor water or wooded exposure:
- Labored breathing, open-mouth breathing, or blue-tinged gums
- High fever, extreme lethargy, or refusal to eat
- Any eye redness, squinting, or sudden vision changes
- Persistent cough that does not improve with initial treatment
- Skin sores that drain or do not heal
- Unexplained lameness plus respiratory signs
If breathing looks difficult, treat it like an emergency.
Prevention tips
Because the fungus lives in the environment, prevention is not perfect, but you can reduce risk and catch problems earlier.
- Know your region. If you live in or travel to an endemic area, keep fungal disease on your radar.
- Avoid high-risk spots when possible. Damp, swampy areas with lots of decaying vegetation can be higher risk.
- Rinse and dry after muddy adventures. This does not prevent inhalation exposure, but it helps overall skin health and makes it easier to notice lesions early.
- Track symptoms after travel. If your dog develops a cough or fever weeks later, mention where you went.
And most importantly, trust your instincts. If your dog is “just not right” and the symptoms are lingering, keep asking questions and advocate for the next step in diagnostics.
Quick FAQ
How long after exposure do signs show up?
It varies. Many dogs show signs within weeks, but it can be longer. That delay is one reason it gets missed.
Can a dog have blastomycosis without a cough?
Yes. Some dogs present mainly with skin lesions, eye inflammation, or lameness even though the lungs were the entry point.
Is blastomycosis the same as Valley Fever?
No. They are different fungal diseases caused by different organisms and with different primary endemic regions, but they can look similar clinically. That is why region and testing are so important.
