Know the early signs of tick-related illness in dogs—lethargy, fever, limping, swelling, GI upset, bruising—plus daily tick-check spots, safe removal ste...
Article
•
Designer Mixes
Anaplasmosis in Dogs: Symptoms, Steps, and What to Do

Shari Shidate
Designer Mixes contributor
If your dog suddenly seems stiff, sleepy, or painful after being outdoors, it is normal to worry. One tick-borne illness I see pet parents in North Texas run into is anaplasmosis. The good news is that most dogs do very well with fast diagnosis and the right treatment. The tricky part is that the symptoms can look like lots of other issues at first.
This step-by-step guide walks you through what anaplasmosis is, the symptoms to watch for, what your veterinarian will test, and what you can do at home to support recovery and prevent future tick bites.
Quick note: This guide is educational and not a substitute for veterinary care.
What is anaplasmosis?
Anaplasmosis is a disease caused by bacteria in the genus Anaplasma that are spread through tick bites. In dogs, the two main species discussed are:
- Anaplasma phagocytophilum (often associated with fever, joint pain, and lethargy)
- Anaplasma platys (often associated with low platelets, which can affect blood clotting)
Ticks pick up the bacteria from infected wildlife, then pass it to dogs during feeding. Many dogs are exposed and never show signs, but others get noticeably sick. It can also occur alongside other tick-borne diseases, like Lyme disease or ehrlichiosis, which can complicate symptoms.
Symptoms at home
Anaplasmosis can show up after a tick bite with timing that varies by the dog and the organism. Many cases show signs around 1 to 2 weeks after exposure, but it can be sooner or take longer. Symptoms can be mild at first. Here is a practical way to think about what you might see, in the order many families notice it.
Step 1: Not themselves
- Low energy, more sleeping than usual
- Less interest in walks or play
- Decreased appetite
Step 2: Pain and movement
- Limping or shifting lameness (one leg looks sore, then another)
- Stiffness, especially when getting up
- Reluctance to jump or use stairs
Step 3: Flu-like signs
- Fever
- Shivering or seeming “off”
- Swollen lymph nodes (you may feel lumps under the jaw, in front of the shoulders, or behind the knees)
Step 4: Bruising or bleeding (more urgent)
Not every dog develops bleeding issues, but if platelet levels drop, you might see:
- Small pinpoint bruises on the gums or belly (petechiae)
- Nosebleeds
- Bruising that seems to appear easily
- Blood in urine or stool
Important: Some dogs have vague signs only, and a few have no signs at all. That is why testing matters if tick exposure is possible.

When to call the vet
Call within 24 hours
- Limping, stiffness, or sudden pain
- Fever, lethargy, or appetite drop after outdoor exposure
- A known tick bite in the last few weeks plus any symptoms
Go to urgent or emergency care
- Bleeding (nosebleeds, bleeding gums, blood in urine or stool)
- Collapse, severe weakness, or trouble breathing
- Pale gums (an emergency sign, but not specific to anaplasmosis)
- Uncontrolled vomiting with dehydration
Even if it ends up not being anaplasmosis, these signs deserve quick attention.
How dogs get it
Anaplasmosis spreads through infected ticks. Your dog does not usually get it from casual contact with another dog. (Rare, non-tick transmission routes like contaminated blood products are possible in theory, but they are not how most pet dogs are exposed.)
The risk goes up with:
- Hiking, hunting, tall grass, brush, or wooded areas
- Backyards with wildlife visitors (deer, rodents)
- Warm months, but ticks can be active outside of summer too, depending on weather
- Inconsistent tick prevention
Because ticks can be tiny and easy to miss, many families never see the tick at all.
What your vet will do
If anaplasmosis is on the list, your veterinarian will typically combine your dog’s history, a physical exam, and lab work.
Step 1: History and exam
- Tick exposure and travel history
- Temperature and pain assessment
- Checking joints, lymph nodes, and gums for bruising
Step 2: In-clinic screening
Many clinics use an in-clinic antibody screening test (for example, a SNAP 4Dx style test) that can screen for multiple tick-borne diseases. A positive antibody result can mean exposure and immune response, not always active illness, so your vet will interpret it with symptoms and other lab values.
Step 3: CBC and platelets
A complete blood count (CBC) helps check for:
- Thrombocytopenia (low platelets), a common finding in tick-borne illness
- Anemia or inflammation patterns
Step 4: More testing if needed
- Chemistry panel to assess organ function and dehydration
- Urinalysis if there are urinary signs
- Specialized testing (like PCR) in some cases to look for active infection. Timing matters, and recent antibiotics can sometimes affect results.
If your dog tests positive but feels fine, your veterinarian may recommend monitoring or additional tests rather than automatically treating. The goal is to treat the dog, not just the test.
Treatment
The standard treatment many veterinarians use for clinical anaplasmosis is a course of doxycycline. Dogs often start improving within 24 to 48 hours, especially when fever and joint pain are part of the picture. In other cases, improvement is more gradual over several days, and full recovery can take longer.
Many treatment plans run about 2 to 4 weeks, but your veterinarian will choose the best length for your dog based on symptoms, test results, and response.
What else may be included
- Pain relief or anti-inflammatory medication, if appropriate
- Fluids if dehydration is present
- Activity restriction while joints are sore
Medication safety
- Give doxycycline exactly as prescribed and finish the full course, even if your dog seems better.
- Ask your vet whether to give it with food and water to reduce stomach upset and lower the risk of esophageal irritation. A practical tip is to avoid “dry pilling” and follow tablets with a small amount of water or a bite of food if your vet says it is okay.
- Doxycycline can cause GI upset in some dogs. If vomiting, refusal to eat, or trouble swallowing shows up, call your vet.
- Do not add over-the-counter human medications for pain unless your veterinarian specifically tells you to. Common ones like ibuprofen and naproxen can be dangerous for dogs.
Home care
Most dogs recover smoothly, but they do need a little extra support while their body rebounds.
At home, focus on
- Rest: Short potty walks only until your vet clears normal exercise.
- Hydration: Encourage water intake. Ask your vet about adding a little warm low-sodium broth if appetite is poor.
- Comfort: Soft bedding and easy access to favorite spots, especially if stairs hurt.
- Nutrition: Offer a gentle, balanced diet if the stomach is sensitive. If appetite is low for more than a day, call your vet.
If your dog seems better quickly, that is wonderful, but keep watching energy level, appetite, and mobility through the full medication course.
Can it be chronic?
Some dogs fully clear signs after treatment and never have another issue. Others may have lingering fatigue or joint sensitivity, especially if diagnosis was delayed or if there is a co-infection. The biggest “chronic” concern I see is that ticks do not always travel alone. Dogs can be exposed to more than one organism, and each may need its own management plan.
If symptoms return after treatment, ask your veterinarian about:
- Rechecking a CBC and platelet count
- Testing for other tick-borne illnesses
- Evaluating joints, pain control, or other underlying conditions
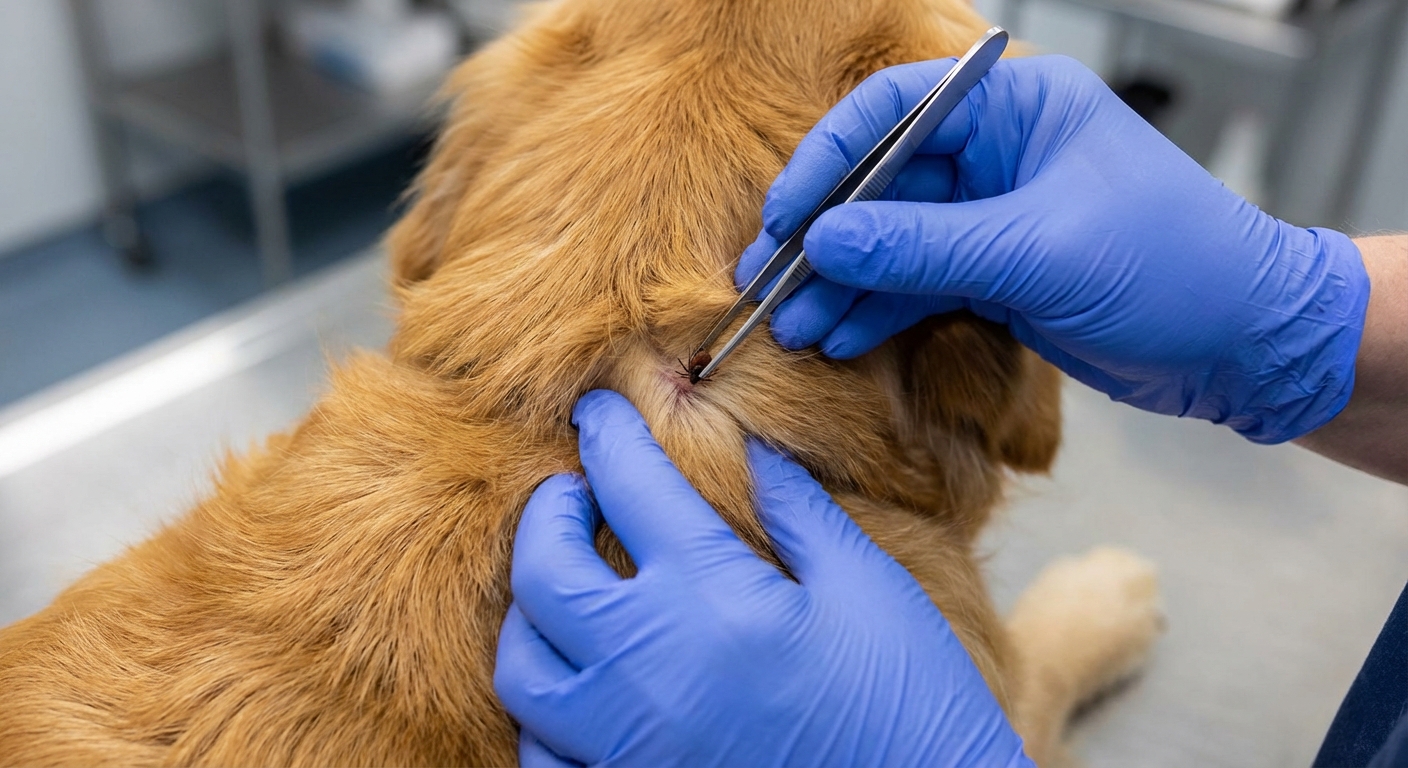
Tick removal
If you find a tick, removing it promptly is helpful. Use fine-tipped tweezers or a tick tool.
- Part the fur and grasp the tick as close to the skin as possible.
- Pull straight out with steady, even pressure.
- Clean the area with mild soap and water or a pet-safe antiseptic.
- Wash your hands.
Avoid home remedies like burning the tick or using oils to make it “back out.” Those methods can increase irritation and do not make removal safer.

Prevention
As a veterinary assistant, I can tell you prevention is where you win the battle. Tick-borne illnesses are stressful, and they are often preventable.
Build a routine
- Use veterinarian-recommended tick prevention: Oral or topical options can be very effective, and some require a prescription. The best choice depends on your dog’s age, health history, and lifestyle. The biggest factor is using it consistently, on schedule.
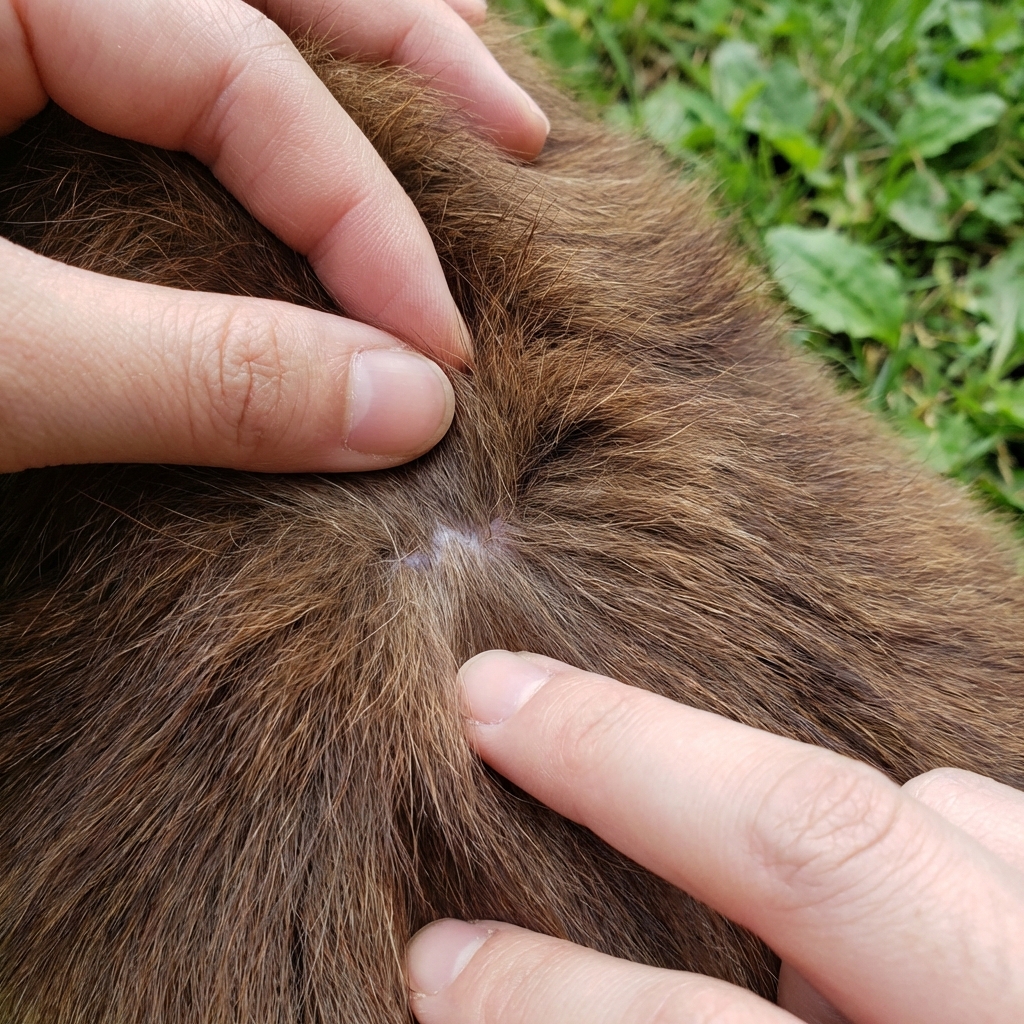
- Do tick checks daily: Especially after walks in tall grass. Feel for small bumps around the ears, collar area, armpits, groin, and between toes.
- Keep your yard less tick-friendly: Trim tall grass, remove brush piles, and keep wildlife attractants managed.
- Ask about regional risk: Tick activity and species vary. Your vet can tell you what is most common where you live and travel.
If you are already using prevention and still found ticks, do not blame yourself. No product is perfect. It is still worth reviewing your routine and product choice with your veterinarian.
Quick checklist
If you want a fast recap, these are the signs that most often raise suspicion for anaplasmosis:
- Lethargy and decreased appetite
- Fever
- Limping, stiff gait, or joint pain
- Swollen lymph nodes
- Low platelets, bruising, or bleeding
If your gut says something is off, trust that feeling and call your veterinary team. Early care is the best care.
Common questions
Is it contagious to other pets or people?
The bacteria are mainly transmitted by ticks. Your dog is not typically a direct contagious risk to you or other pets through normal contact. The bigger concern is shared tick exposure in the same environment.
Can my dog get it more than once?
Yes. A prior infection does not reliably protect against future infections. That is why ongoing tick prevention matters.
Will my dog always test positive?
Some antibody tests can stay positive for months after exposure. Your veterinarian will interpret results based on symptoms and other lab work, not just a single positive line.