Acral Lick Granuloma in Dogs

If your dog has one specific spot they cannot stop licking, especially on a leg, you are not dealing with “a little itch.” One common cause is an acral lick granuloma, also called lick dermatitis. It can start small, then the constant licking inflames the skin, breaks the barrier, and can invite secondary infection. Over time it may turn into a thickened, hairless, sometimes oozing sore that feels impossible to heal.
Here is the hopeful part: many dogs do get better when we treat this like a medical problem first, and a behavior problem second. The key is figuring out what is driving the licking in your dog: boredom and anxiety, pain, allergies, or a mix of all three.
Quick note: This guide is educational and not a substitute for a veterinary exam. Several skin conditions can look similar at home, so it is worth getting confirmation early.
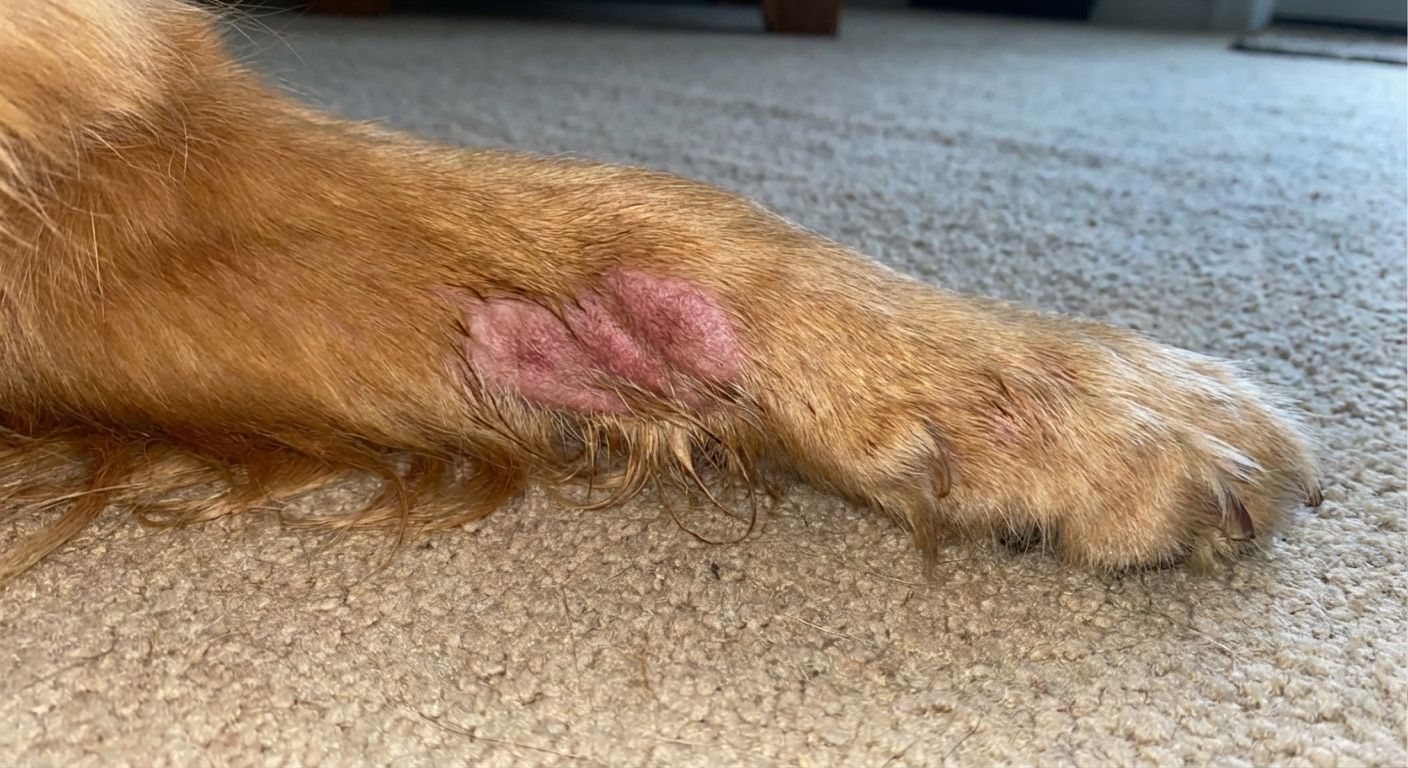
What it can look like
Acral lick granulomas typically look like:
- One main lesion (not usually multiple scattered hot spots)
- Hair loss over a well-defined area
- Red, raw, moist skin early on
- Thick, raised, firm skin later (a “callus-like” plaque or nodule)
- Brown staining from saliva over time
- Reopening and bleeding after it starts to scab
Because dogs lick when it hurts or itches, a granuloma is often your dog’s way of telling you something is going on under the surface.
Common locations
The word acral points to the extremities. Most lick granulomas show up on:
- Front legs, especially the wrist (carpus)
- Back legs, especially near the hock (ankle)
- Less commonly, the top of a paw or an area the dog can easily reach
Dogs tend to pick a spot that is easy to access and easy to “self-soothe.” Once the brain links licking with relief, it becomes a loop: itch or pain leads to licking, licking causes inflammation, inflammation increases itch, and around we go.

Boredom vs pain vs allergies
In a veterinary setting, we often think of lick granulomas as a three-lane highway. More than one lane can be active at the same time.
1) Boredom, stress, and compulsive licking
This is the “habit” piece, but it is rarely the whole story. Clues include:
- Licking ramps up when the dog is alone or in the evening
- Your dog struggles with separation anxiety or noise sensitivity
- They lick during downtime, after excitement, or when routines change
- They may also over-groom other areas or chew paws intermittently
Important: even if it began as stress licking, once the skin is damaged, there is often pain and sometimes secondary infection keeping it going.
2) Pain under the skin
Pain is a very common driver, especially in adult and senior dogs. Clues include:
- The spot is right over a joint (wrist or hock are classic)
- Limping, stiffness getting up, slower on stairs, less jumping
- Licking increases after exercise or cold weather
- Your dog resists having that leg handled
Dogs cannot point to a sore joint. They lick it.
3) Allergy and itch
Allergies can absolutely contribute, even if there is only one main lesion. Clues include:
- History of paw licking, ear infections, or seasonal itch
- Other itchy spots: belly, armpits, face, base of tail
- Flare-ups in certain months, after mowing, or after travel
- Other pets in the home itching (think fleas)
If allergies are part of the picture, controlling the itch helps prevent relapse. That said, some dogs will still relapse if pain or stress is not addressed too, so it is best treated as a multi-trigger problem.
Why cones and wraps fail
I know the first instinct is, “I will just cover it or stop the licking.” That sounds logical, but there are common pitfalls.
E-collars and cones
An e-collar can be a necessary tool, especially early on, because every lick resets healing. The problem is that a cone alone does not address the cause. Many dogs will start licking the moment the collar comes off if pain, itch, infection, or anxiety is still there.
Anti-lick bitter sprays
Owners almost always try bitter sprays first. Sometimes they help with mild, casual licking, but dogs with true lick granulomas often lick right through them. Some products also sting on broken skin or cause extra irritation, which can make the cycle worse.
Soft collars, donuts, and sleeves
Some dogs can still reach the spot with a donut collar. Sleeves can work short-term, but if they rub, trap moisture, or slide, you can end up with:
- Maceration (waterlogged skin that breaks down)
- More infection from heat and humidity
- Pressure sores from a tight wrap
Bandages at home
Bandaging limbs is tricky even for professionals. A wrap that is too tight can compromise circulation. A wrap that is too loose can slip and chafe. And a wrap left on too long can create the perfect environment for bacteria and yeast.
If your vet recommends a bandage, ask these exact questions:
- How tight should it be and how can I check toes for swelling?
- How often should it be changed?
- What do I do if it gets wet or slips?
If you only remember one thing: preventing licking helps healing, but stopping the licking without treating the driver is like putting a lid on a boiling pot.
What your vet should check
A good workup saves time and money because it prevents the cycle of “try a cream, it comes back.” Here are the most common steps.
1) Confirm what it is
Several conditions can mimic a lick granuloma, including hot spots (pyotraumatic dermatitis), deep pyoderma, demodex mites, ringworm, foreign body reactions, autoimmune skin disease, vasculitis, or even tumors. If the lesion looks unusual or keeps growing, your vet may recommend cytology, a skin scraping, culture, or a biopsy.
2) Check for infection
Once skin is licked raw, secondary infection is common but not guaranteed. Your vet may:
- Do a tape prep or impression smear to look for bacteria and yeast
- Prescribe topical antiseptics (often chlorhexidine-based)
- Use oral antibiotics if the infection is deeper, spreading, or severe
- Recommend a culture if it is chronic, deep, recurrent, or not responding, to target the right antibiotic
Stewardship matters here. Avoid using leftover antibiotics, and do not stop a prescribed course early just because the surface looks better.
3) Screen for allergy triggers
Depending on history, this may include:
- Strong flea control recommendations (flea allergy can be dramatic)
- Discussing seasonal patterns and indoor allergens
- Considering a veterinarian-guided food elimination trial if symptoms fit
- Discussing itch control options (including newer targeted medications)
4) Evaluate for pain and orthopedic disease
This is the step people are most surprised by. Your vet may palpate joints, check range of motion, and recommend:
- X-rays of the wrist, elbow, hock, or spine
- A trial of pain control if arthritis is suspected
- Physical therapy or controlled exercise plans
5) Add-on treatments for stubborn cases
Some dogs need a little more help once the basics are covered. Depending on the case, your vet may discuss options like cold laser therapy (often Class IV laser) to stimulate healing, intralesional medications, or referral to dermatology or behavior support for difficult, chronic loops.

What actually helps
In my experience as a veterinary assistant, the best results come from a stacked approach. You are not looking for one magic product. You are building a plan that covers skin healing, itch or pain control, and brain habits.
Step 1: Stop the damage
- Use an e-collar or vet-approved barrier consistently, especially when you cannot supervise.
- Keep nails trimmed to reduce trauma if scratching starts too.
- Ask about safe topical options. Avoid random human ointments unless your vet approves. Zinc oxide (common in diaper rash creams) can be toxic if licked, and frequent use of hydrocortisone can thin the skin and slow healing.
Step 2: Treat infection if present
If cytology shows bacteria or yeast, treating infection is not optional. Chronic granulomas can involve deeper tissue, and they often need a longer, more targeted course of treatment than a simple hot spot. Your vet may also lean heavily on topical therapy, then add oral medication when the depth and severity truly call for it.
Step 3: Control itch if allergies are in the mix
Depending on your dog, your vet may recommend flea prevention, medicated bathing routines, prescription itch medications, allergy testing, or immunotherapy. The best plan is the one you can do consistently.
Step 4: Treat pain if it sits over a joint
If arthritis or orthopedic pain is contributing, treating pain can dramatically reduce licking. That may include prescription pain relief, joint supplements, weight management, rehab exercises, or arthritis-focused plans.
Step 5: Replace the licking
This part matters, especially after weeks of licking. Practical options include:
- Increase structured enrichment: food puzzles, sniff walks, training sessions
- Predictable routines for anxious dogs
- Reward calm behavior away from the lesion
- For severe compulsive cases, talk to your vet about behavior medication and a trainer who uses positive reinforcement
Think of it this way: we do not just remove the bad habit. We give your dog a better job.
How long healing takes
This is the section that keeps families from giving up too soon.
Early lesions
If the spot is newly bald and irritated, you may see improvement in 7 to 14 days with consistent licking prevention and the right treatment.
Chronic, thickened lesions
If the lesion is raised, firm, or has been there for weeks to months, expect:
- 2 to 4 weeks to get inflammation and any infection under control
- 6 to 12 weeks (and sometimes a few months) for the skin to remodel and hair to start returning
Some dogs need ongoing management for allergies, arthritis, or anxiety to prevent relapse. That is not failure. That is chronic care, like managing ear infections or joint disease.
When it is urgent
Please contact your veterinarian promptly if you notice:
- Rapid swelling, heat, or spreading redness
- Pus, a strong odor, or significant oozing
- Lameness that appears suddenly
- Fever, lethargy, or your dog seems painful
- A lesion that looks atypical, ulcerated, or keeps growing despite prevention
Deep infections can become complicated quickly, and some masses can mimic granulomas.
At-home support
While you are scheduling a vet visit or waiting on results, here are gentle, practical steps that support healing without overcomplicating things:
- Prevent licking during the times it is most intense (often evenings and when you are out).
- Increase low-stress activity: two sniff-heavy walks are often more calming than one high-intensity session.
- Check flea control for every pet in the home.
- Keep the area clean and dry as directed by your vet. Moisture is the enemy of healing.
- Track triggers: note time of day, after exercise, after lawn exposure, after certain treats.

The bottom line
An acral lick granuloma is not stubborn because your dog is stubborn. It is stubborn because it is usually multifactorial: skin inflammation plus self-trauma plus an itch or pain trigger, often layered with stress or habit, and sometimes complicated by infection.
If you and your vet can answer these three questions, you are on the right path:
- Is there infection that needs to be treated?
- Is there an itch driver like allergies or fleas?
- Is there pain in the joint or limb under the lesion?
With a layered plan and a realistic timeline, many dogs can heal and stay healed. And you do not have to do it perfectly. You just have to do it consistently.
